Thyroid gland pathology includes:
- Thyroglossal duct cyst
- Lingual thyroid
- Hyperthyroidism
- Graves’ disease
- Multinodular goiter
- Cretinism
- Myxedema
- Hashimoto thyroiditis
- Subacute granulomatous thyroiditis
- Riedel fibrosing thyroiditis
- Follicular thyroid adenoma
- Follicular thyroid carcinoma
- Papillary thyroid carcinoma
- Medullary thyroid carcinoma
- Anaplastic thyroid carcinoma
Thyroglossal Duct Cyst
Thyroglossal duct cyst is a cystic dilation of thyroglossal duct remnant.
The thyroglossal duct leads from the base of the tongue to the anterior neck, where the thyroid develops.
While the thyroglossal duct ordinarily involutes, a prolonged duct may enlarge cystically.
Thyroglossal duct cyst presents as an anterior neck mass.
Lingual Thyroid
The presence of thyroid tissue at the base of the tongue is known as lingual thyroid.
Lingual thyroid appears as a mass of tongue at the base.
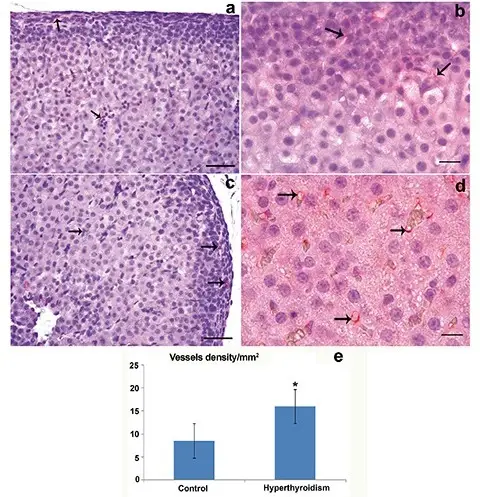
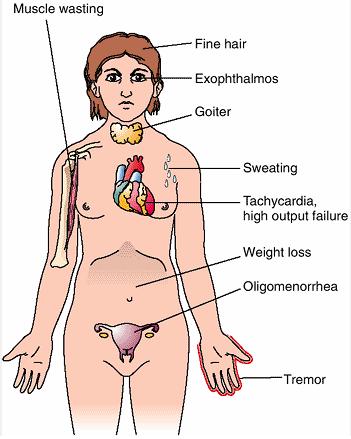
Hyperthyroidism
When the thyroid gland overproduces the hormone thyroxine, hyperthyroidism (overactive thyroid) occurs.
Hyperthyroidism causes an increase in sympathetic nervous system activity and a rise in basal metabolic rate as a result of increased Na+-K+ ATPase production and B1-adrenergic receptor expression, respectively.
Symptoms of hyperthyroidism include:
- Weight loss despite increased appetite
- Heat intolerance
- Sweating
- Tachycardia
- Tremor
- Anxiety
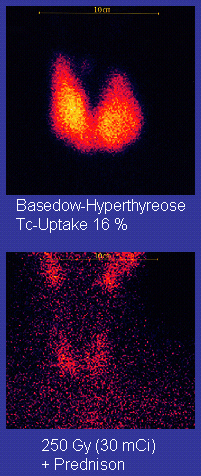
Graves’ Disease
Graves’ disease is an autoimmune disorder that affects the thyroid.
In Graves’ disease, autoantibody IgG activates the thyroid stimulating hormone (TSH) receptor which increases thyroid hormone production and release.
In women of childbearing age (between the ages of 20-years-old and 40-years-old) this condition is the most common cause of hyperthyroidism.
Hyperthyroidism, diffuse goiter, and persistent thyroid stimulating hormone (TSH) stimulation cause thyroid hyperplasia and hypertrophy as clinical characteristics.
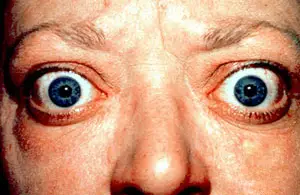
Clinical features of Graves’ disease include:
- Exophthalmos aka proptosis
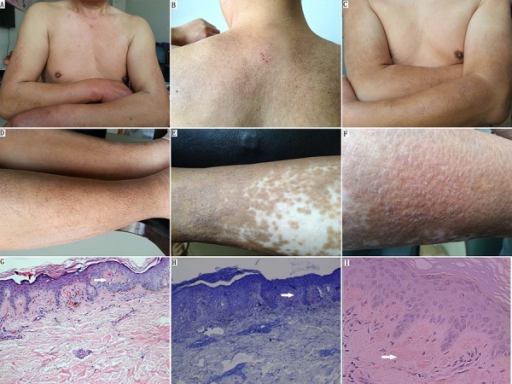
- Pretibial myxedema may occur as well
Thyroid stimulating hormone (TSH) activation causes glycosaminoglycan buildup, including chondroitin sulfate and hyaluronic acid, as well as inflammation, fibrosis, and edema, which result in exophthalmos and pretibial myxedema.
Fibroblasts behind the orbit and atop the shin express the thyroid stimulating hormone (TSH) receptor.
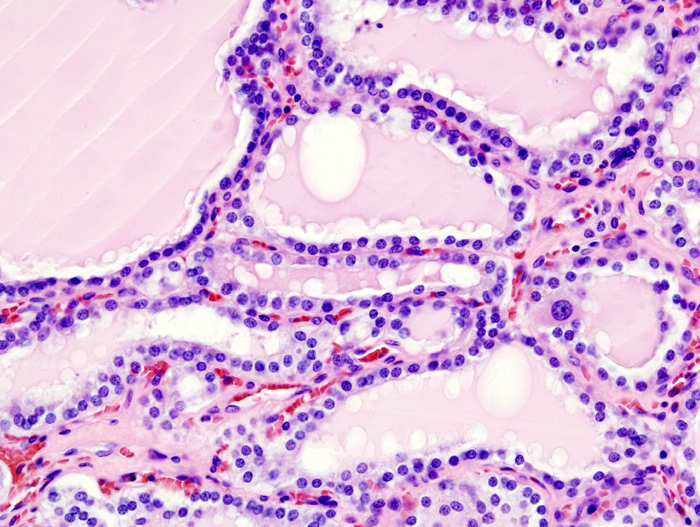
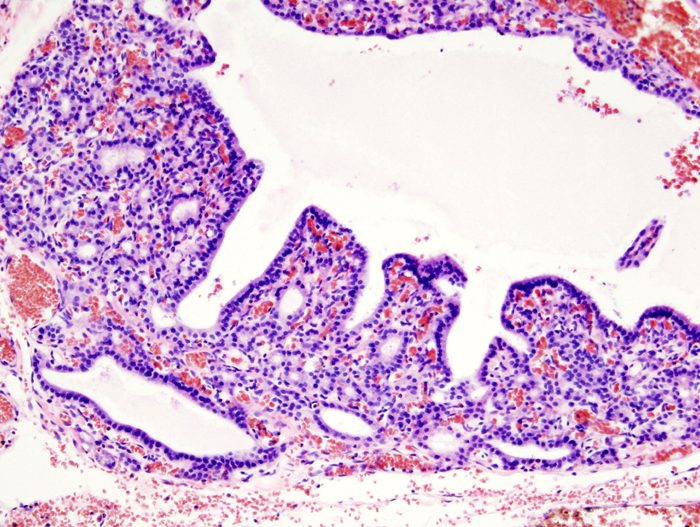
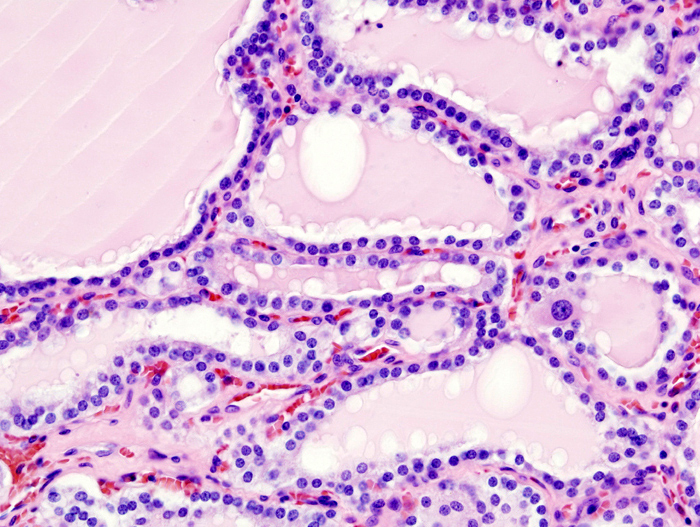
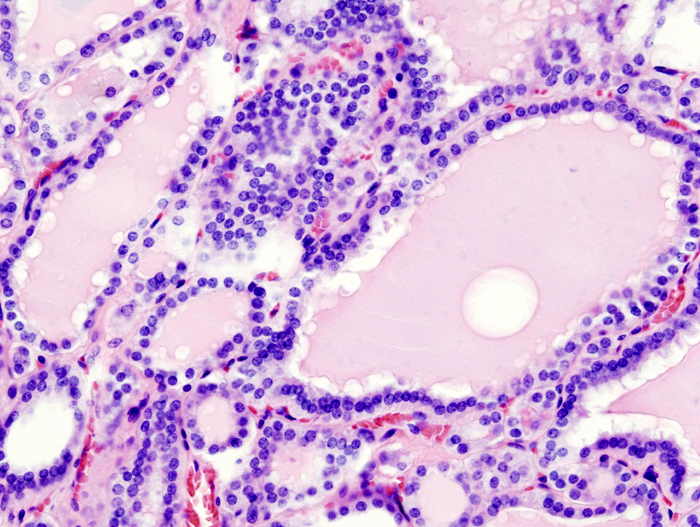
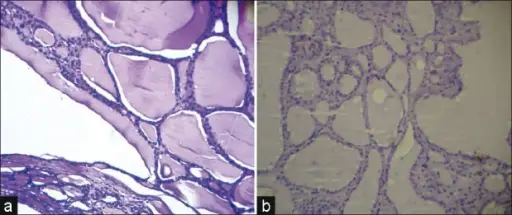
Histology of Graves’ disease shows irregular follicles with scalloped colloids and chronic inflammation are seen in histology.
Laboratory findings of Graves’ disease show:
- Increased total and free T4
- Decreased thyroid stimulating hormone (TSH)
- Hypocholesterolemia
- Elevated blood glucose
Free T4 downregulates thyrotropin-releasing hormone (TRH) receptors in the anterior pituitary to reduce thyroid stimulating hormone (TSH) release.
Treatment of Graves disease includes thioamide and radioiodine ablation.
Thyroid storm is a potentially fatal condition caused by huge hormone excess and high catecholamines, which are typically produced in reaction to stressors like surgery or delivery.
The symptoms of thyroid storm include:
- Hypovolemic shock
- Tachycardia
- Heat intolerance
- Vomiting
Beta-blockers, steroids, and propylthiouracil (PTU) are potential treatment options.
Propylthiouracil (PTU) prevents peripheral T4 to T3 conversion as well as the peroxidase-mediated oxidation, organification, and coupling phases of thyroid hormone production.
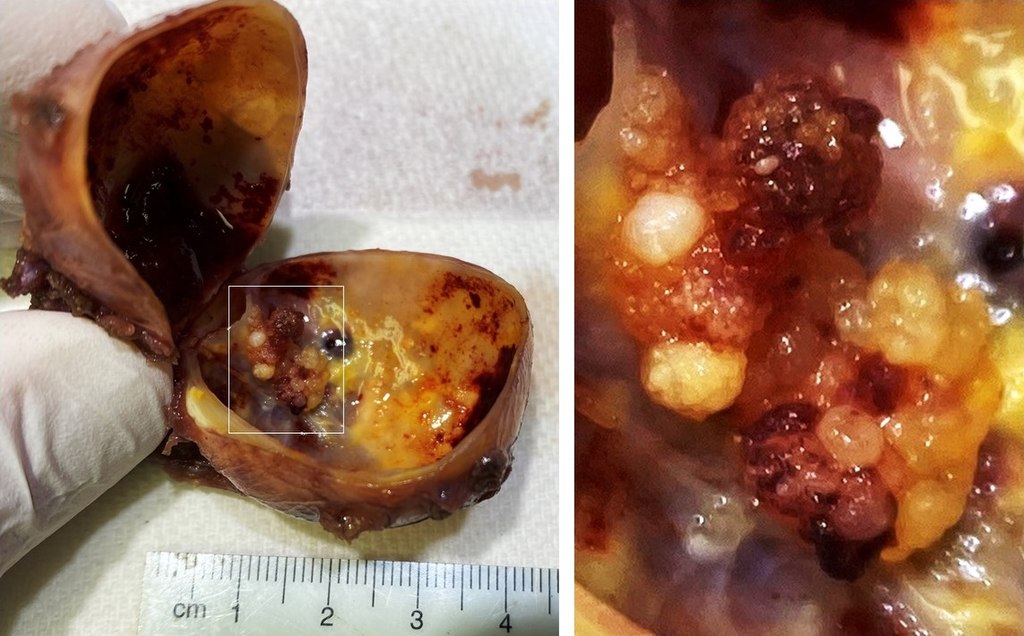
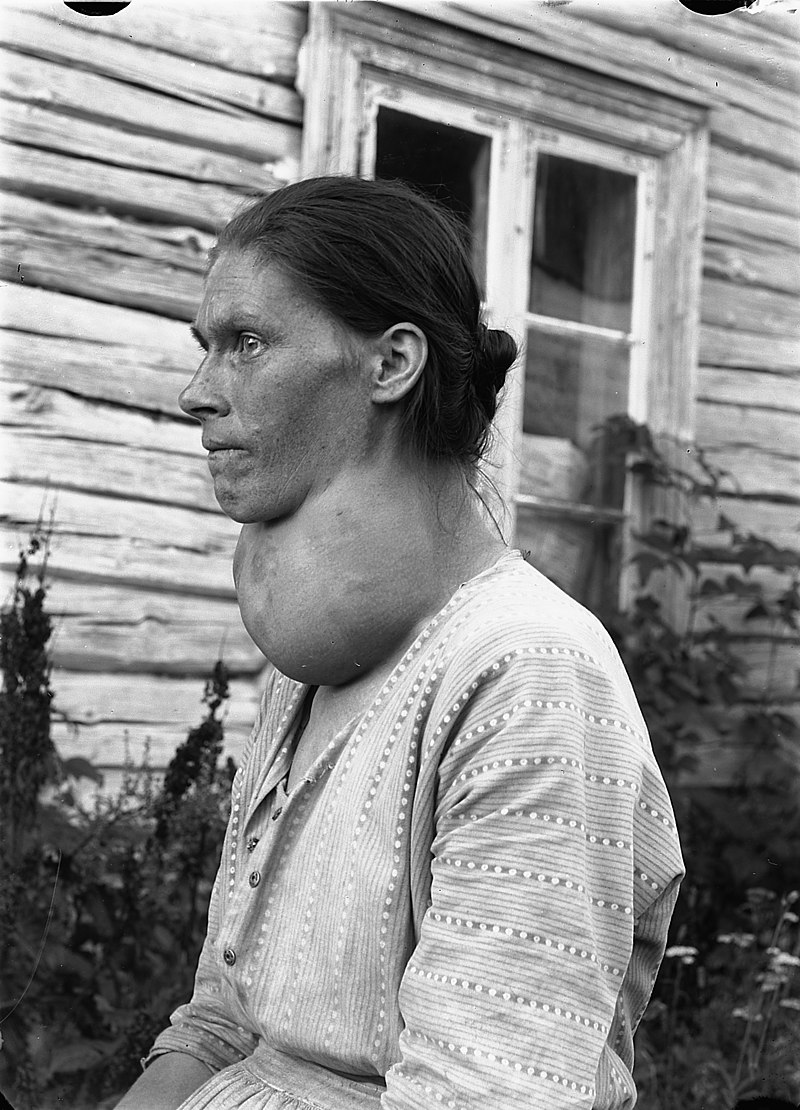
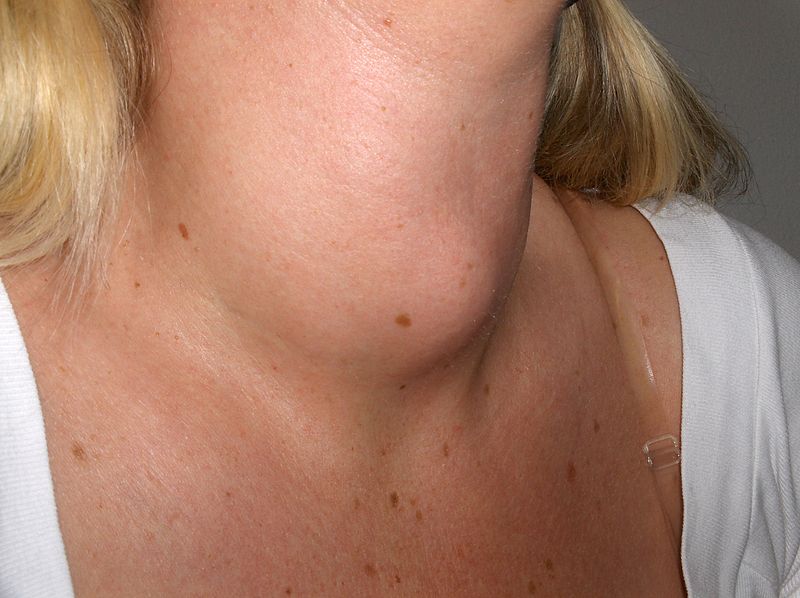
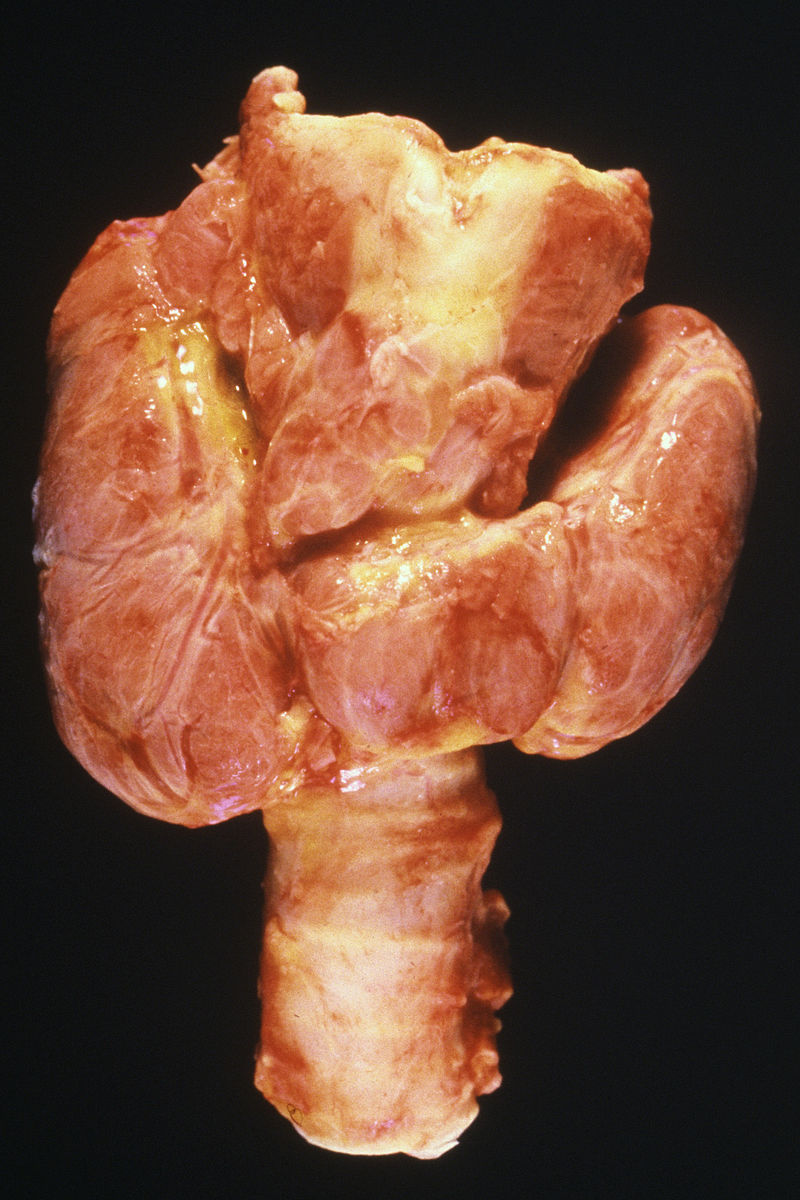
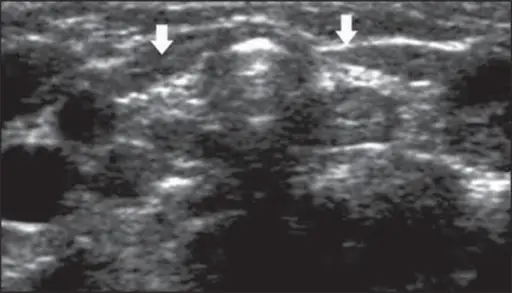
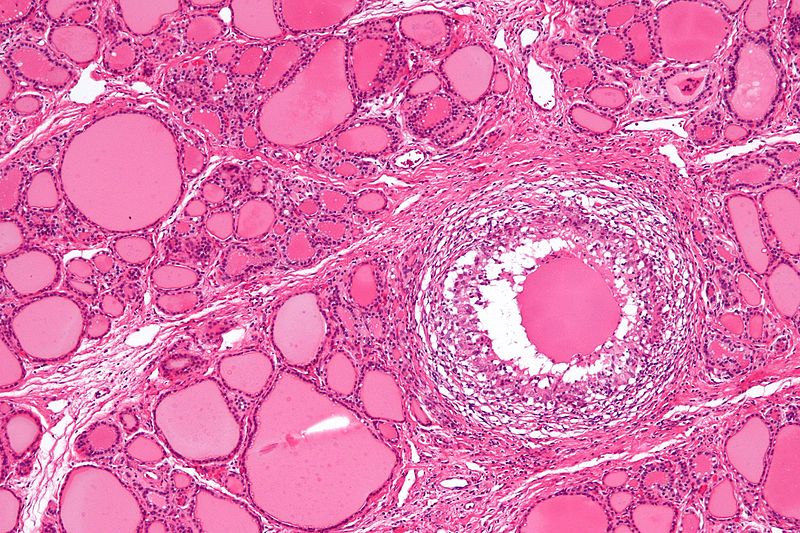
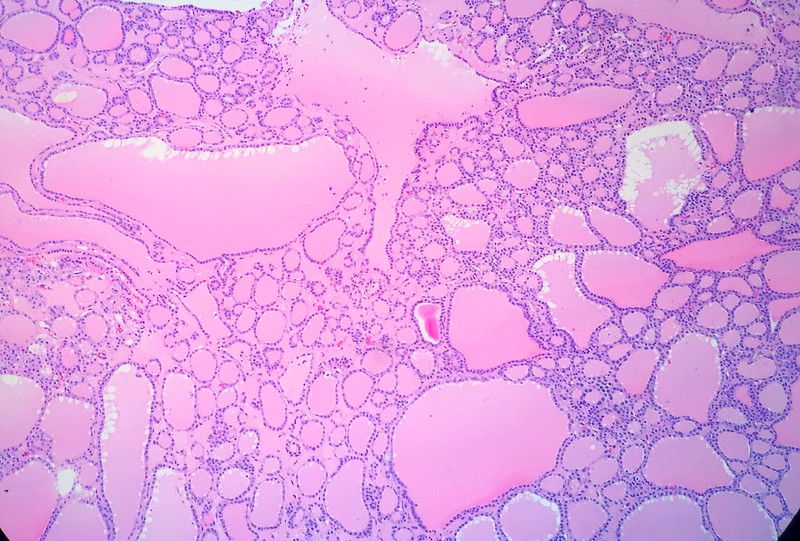
Multinodular Goiter
Multinodular goiter is described as numerous nodules in an enlarged thyroid gland caused by a relative iodine deficit.
Multinodular goiters are typically nontoxic (euthyroid).
Rarely, an area will lose its thyroid stimulating hormone (TSH)-dependent state, causing T1 release, hyperthyroidism, or toxic goiter.
Hypothyroidism
Cretinism
Hypothyroidism in newborns may result in cretinism.
Symptoms of cretinism include:
- Mental retardation
- Oversized tongue
- Small stature
- Macroglossia (enlarged tongue)
- Skeletal deformities
- Coarse facial characteristics
Thyroid hormone is required for normal brain and skeletal development.
Cretinism may be caused by:
- Maternal hypothyroidism during early pregnancy
- Thyroid agenesis
- Dyshormonogenetic goiter
- Iodine deficiency
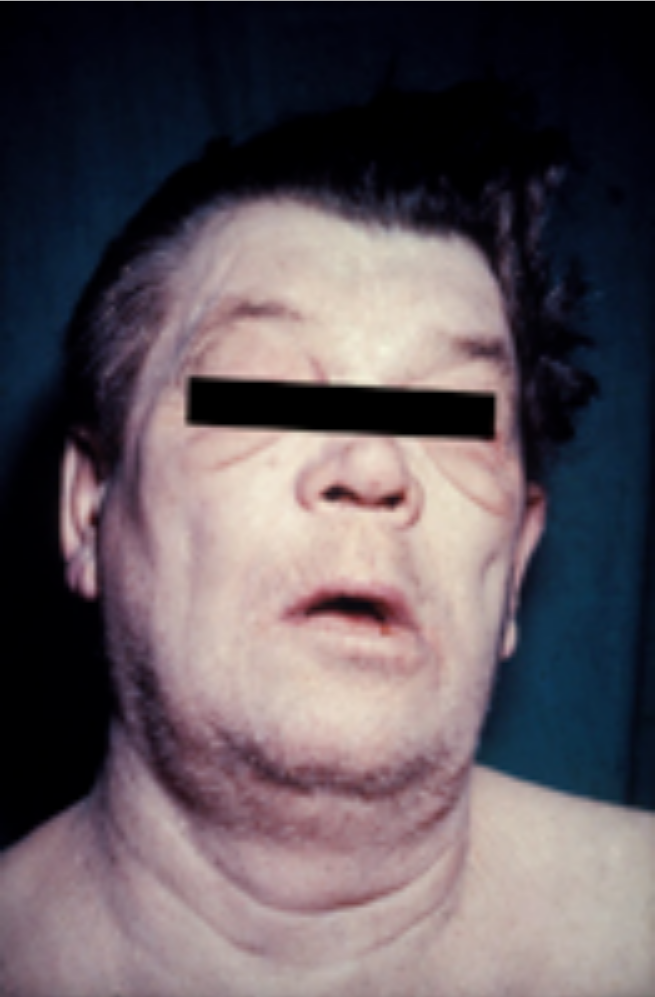
Myxedema
Older children or adults with myxedema have hypothyroidism, which is characterized by a decline in basal metabolic rate and a reduction in sympathetic nervous system activity.
Myxedema is the accumulation of glycosaminoglycans in the skin and soft tissue, which causes weight gain despite a normal appetite and a slowing of mental activity.
Myxedema also causes a deepening of voice and tongue enlargement.
Myxedema also results in muscle weakness, cold sensitivity with decreased sweating, bradycardia with decreased cardiac output, weariness, oligomenorrhea, hypercholesterolemia, and constipation.
Causes of myxedema include:
- Iodine deficiency
- Hashimoto thyroiditis
- Lithium medication use
- Surgical removal of the thyroid
- Radioactive ablation of the thyroid
Thyroiditis
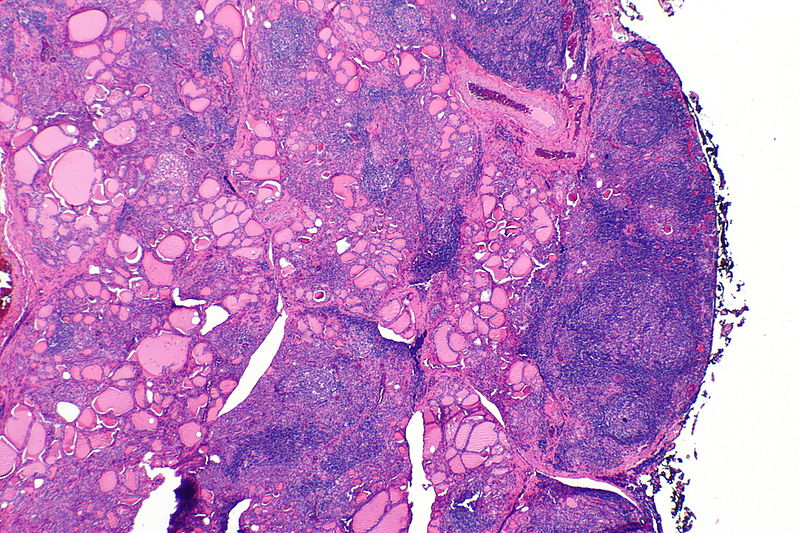
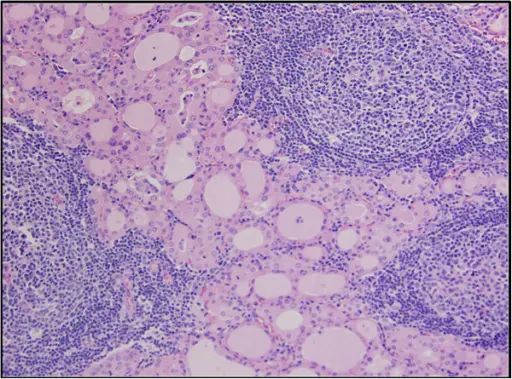
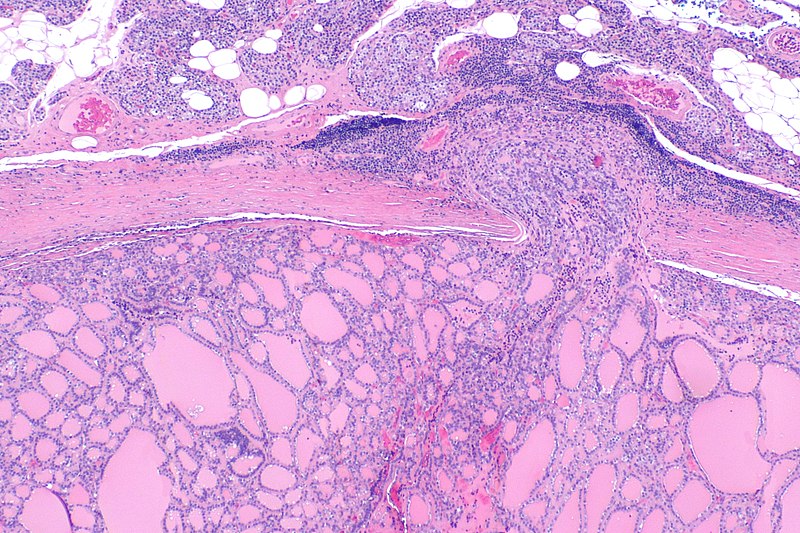
Hashimoto Thyroiditis
Hashimoto thyroiditis is the HLA-DRS-related autoimmune destruction of the thyroid gland.
The most frequent reason for hypothyroidism in areas with sufficient iodine levels.
The progression from hyperthyroidism to hypothyroidism may begin out as follicular damage-induced hyperthyroidism.
The presence of antithyroglobulin and antimicrosomal antibodies is frequently indicative of thyroid impairment.
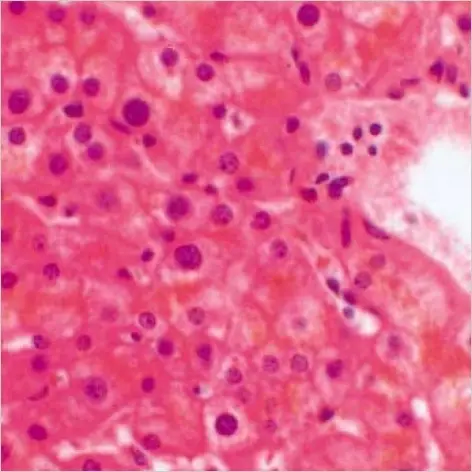
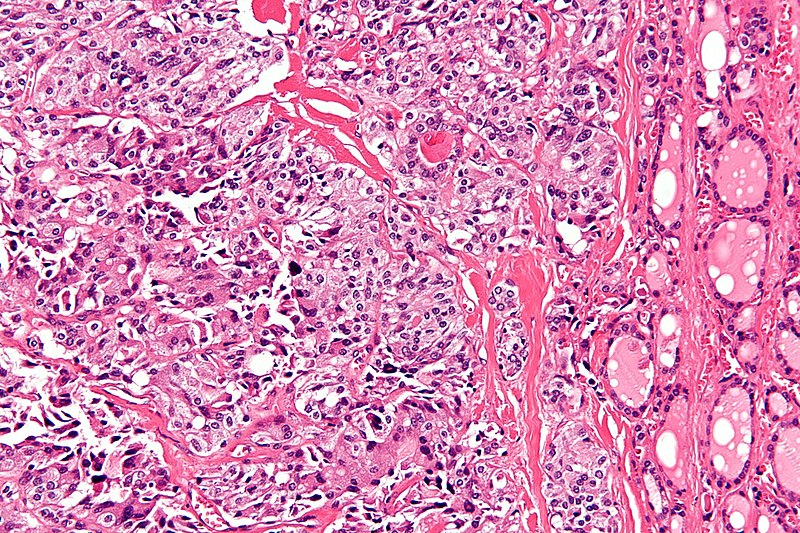
Histologically, Hashimoto thyroiditis shows chronic inflammation with germinal centers and Hürthle cells is associated with eosinophilic metaplasia of cells lining follicles.
There is an elevated risk for B-cell lymphoma in Hashimoto thyroiditis.
Subacute Granulomatous (De Quervain) Thyroiditis
Subacute granulomatous thyroiditis is due to a viral infection that manifests as a sensitive thyroid and temporary hyperthyroidism.
Subacute granulomatous thyroiditis is also called de Quervain thyroiditis.
Subacute granulomatous thyroiditis is self-limited and does not progress to hypothyroidism.
Riedel Fibrosing Thyroiditis
Riedel fibrosing thyroiditis manifests as hypothyroidism with a “hard as wood,” non-tender thyroid gland and is a chronic inflammation with significant thyroid fibrosis.
Local structures like the airway may get affected by a fibrosis that has spread.
Clinically, Riedel fibrosing thyroiditis resembles anaplastic carcinoma, but the patients are younger, no malignant cells are present.
Thyroid Neoplasia
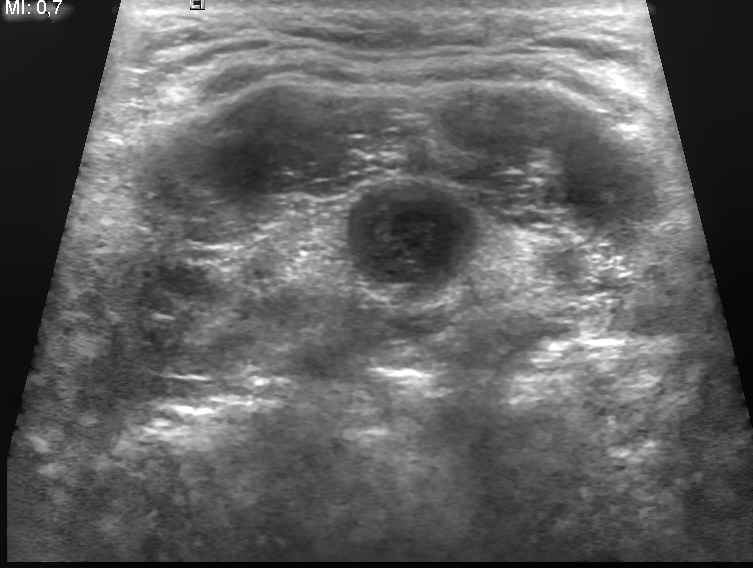
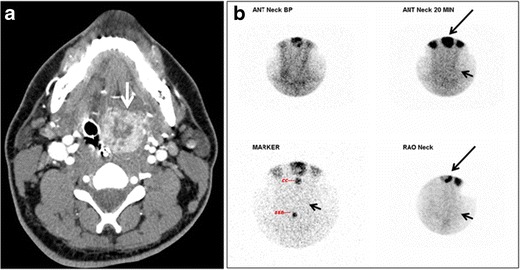
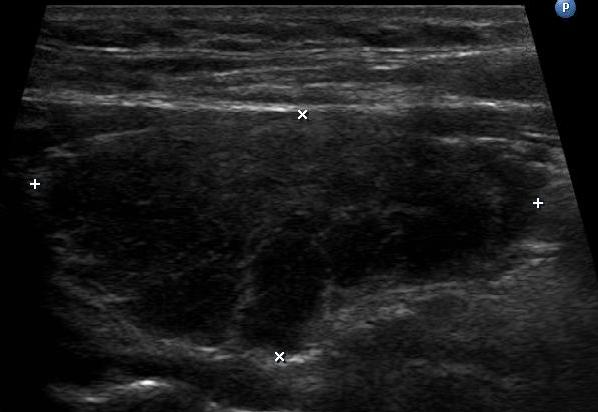
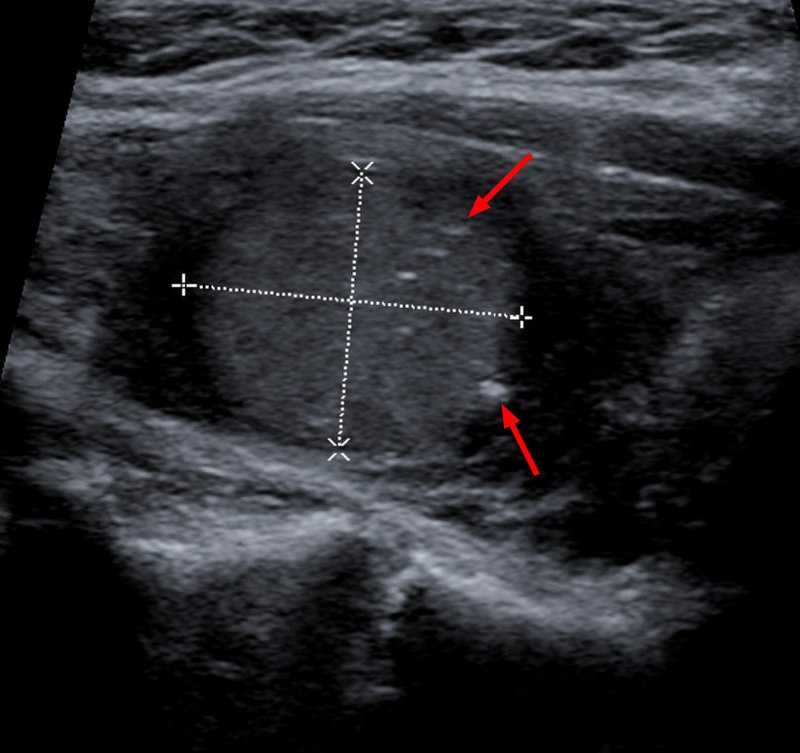
Thyroid nodules are more likely to be benign than malignant, and thyroid neoplasia usually appears as a distinct, solitary nodule.
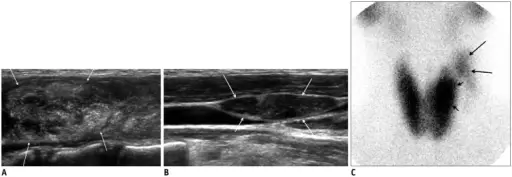
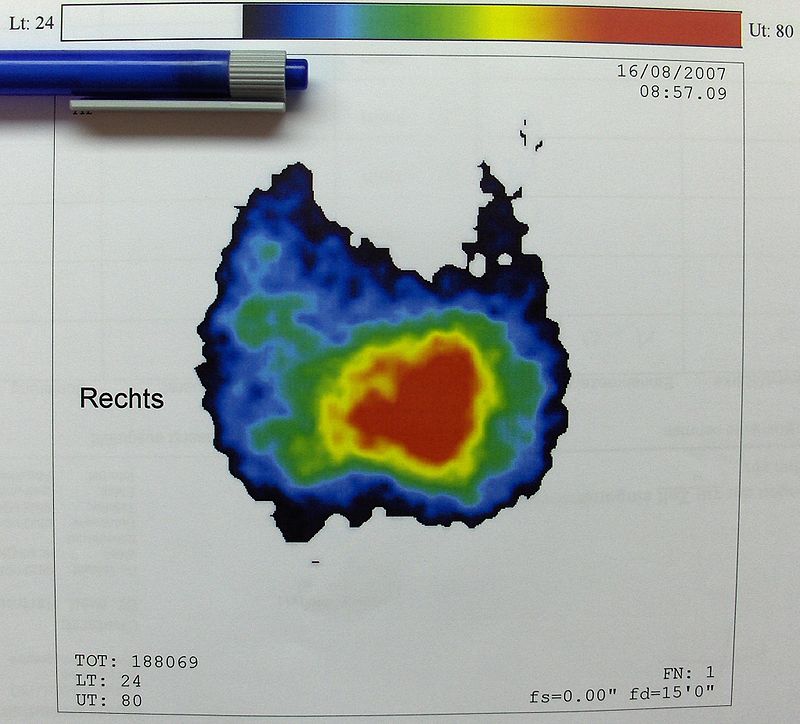
I-131 radioactive uptake studies are useful to further characterize nodules.
Increased uptake (hot nodule) is seen in Graves’ disease or nodular goiter.
Decreased uptake (cold nodule) is seen in adenoma and carcinoma and they often warrant biopsy.
Biopsy is performed by fine needle aspiration (FNA).
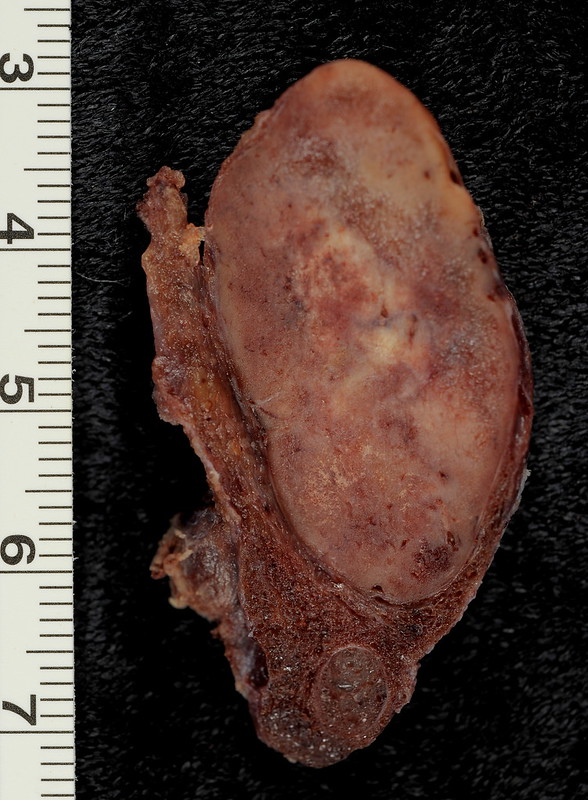
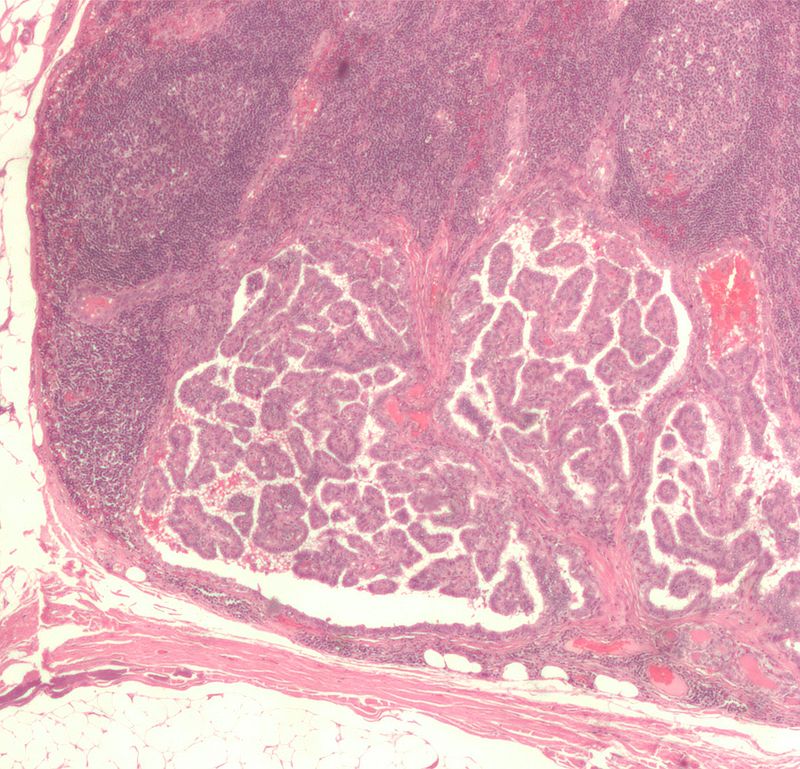
Follicular Thyroid Adenoma
Follicular thyroid adenoma is characterized by a benign proliferation of follicles encased in an inactive fibrous capsule.
Follicular thyroid adenoma does not invade the capsule.
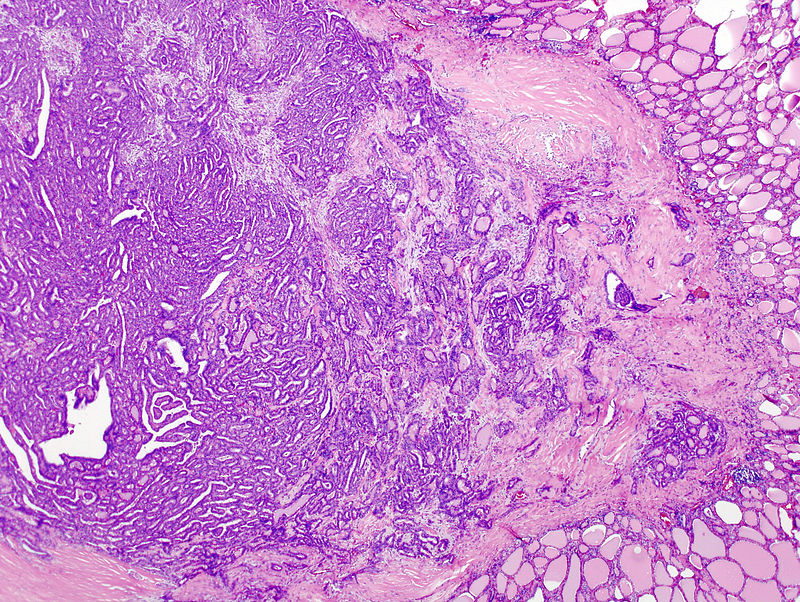
Follicular Thyroid Carcinoma
Follicular thyroid carcinoma (FTC) is the malignant proliferation of thyroid follicles with invasion through the capsule.
Follicular thyroid carcinoma invades the capsule.
The distinction between a follicular adenoma and a follicular carcinoma cannot be made by fine needle aspiration (FNA) because FNA only looks at the cells and not the entire capsule under a microscope.
Metastasis of papillary thyroid carcinoma (PTC) generally occurs via hematogenous spread.
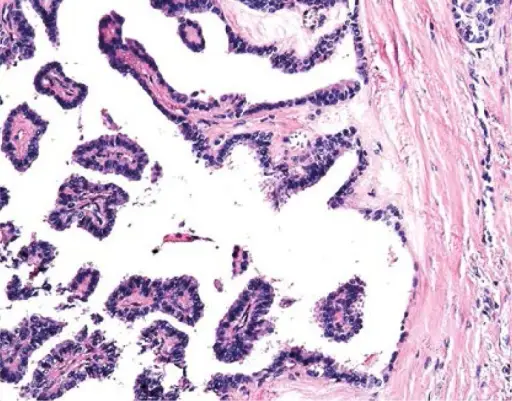
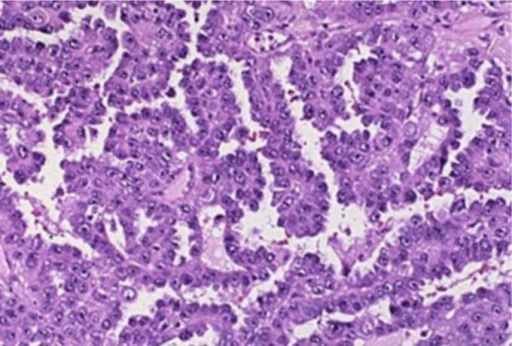
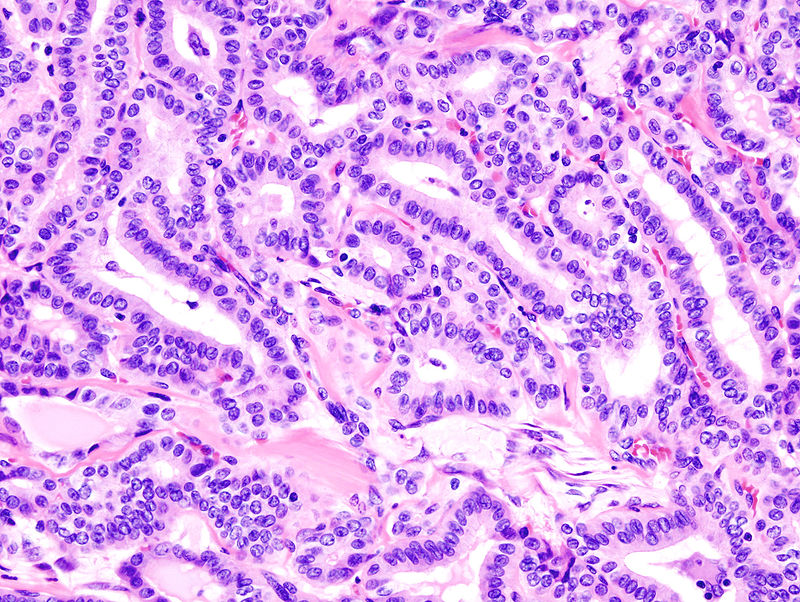
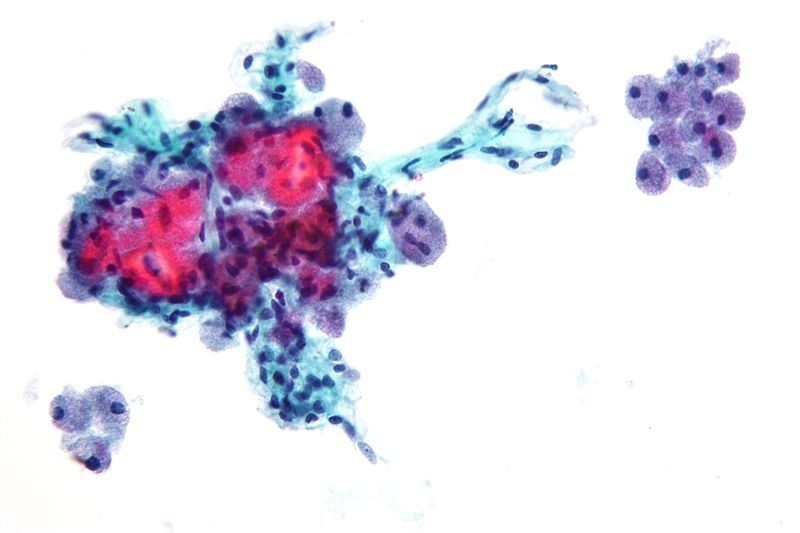
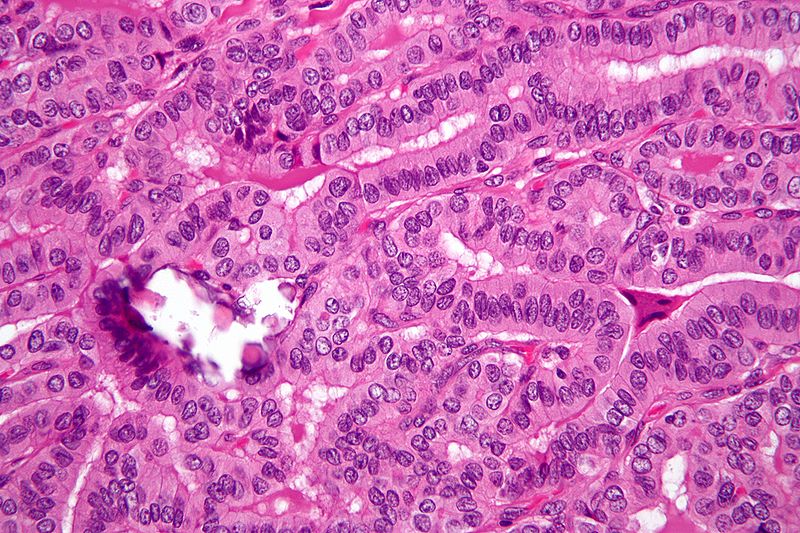
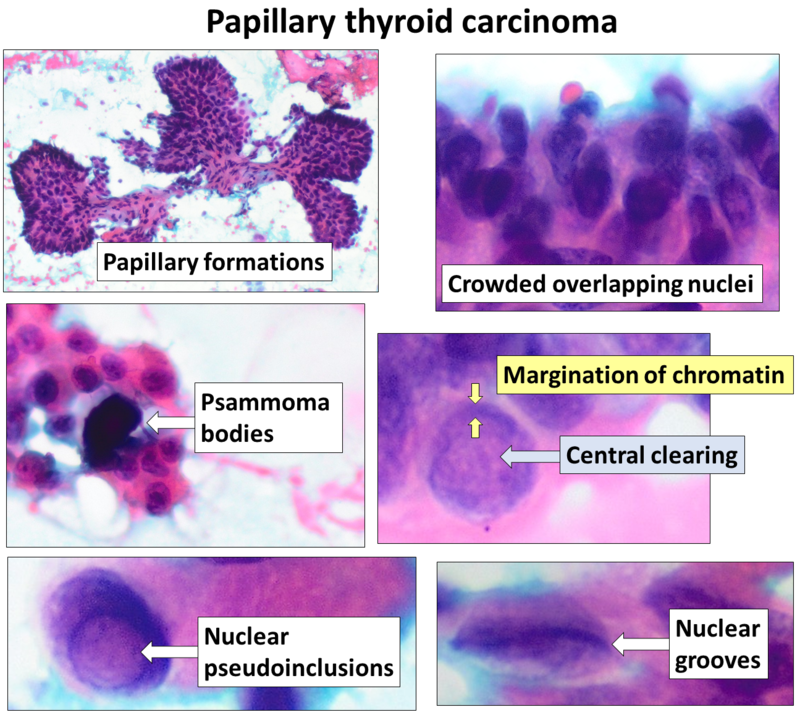
Papillary Thyroid Carcinoma
Papillary thyroid carcinoma (PTC) is the most common kind of thyroid cancer.
A significant risk factor for papillary thyroid carcinoma (PTC) is early ionizing radiation exposure.
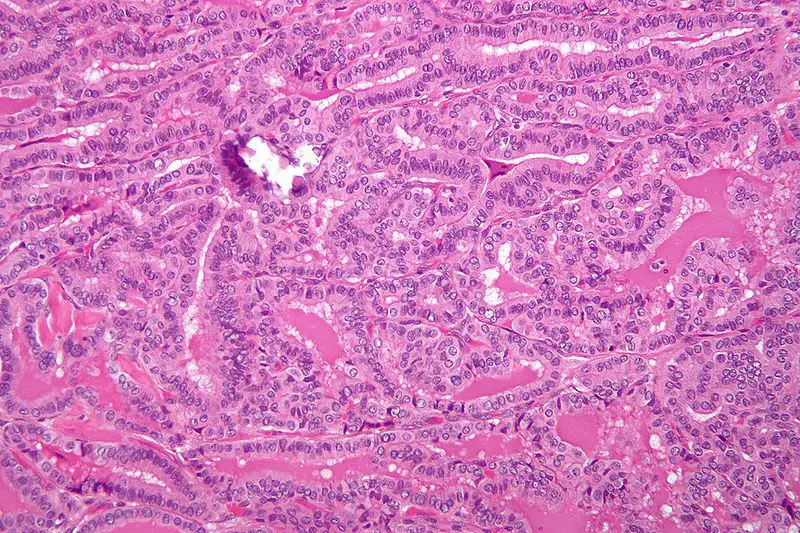
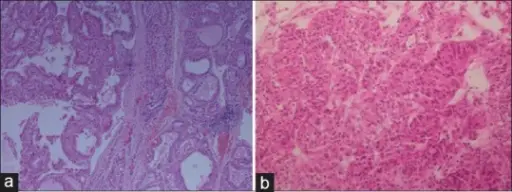
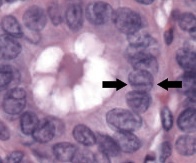
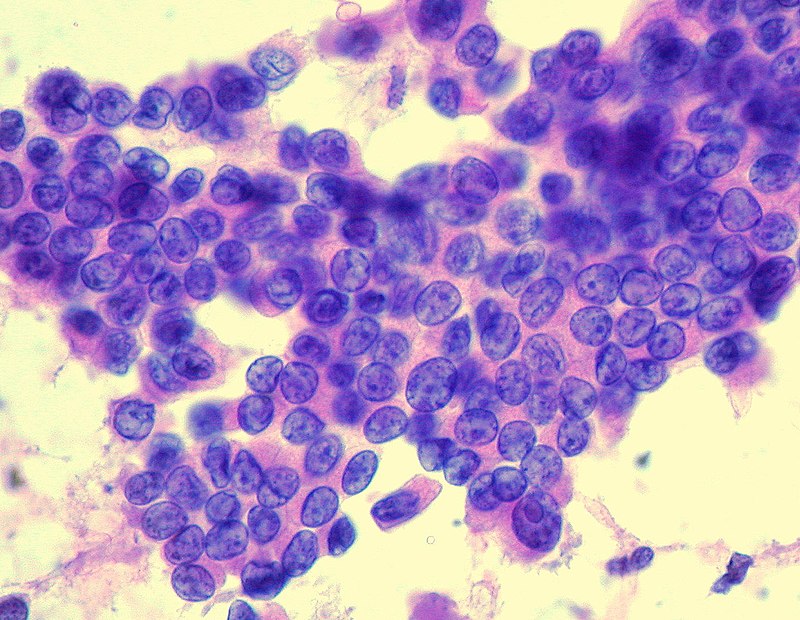
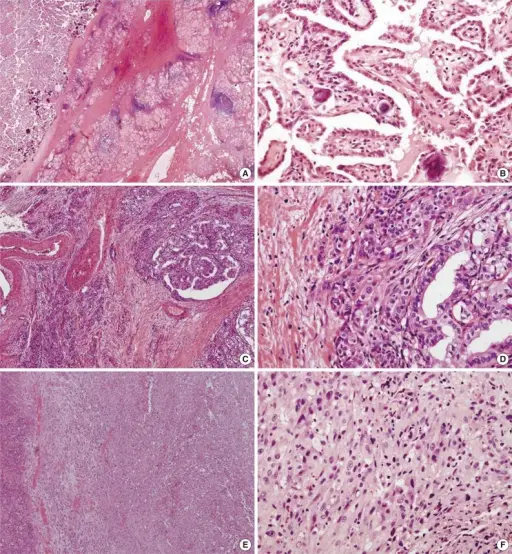
Histology of papillary thyroid carcinoma (PTC) shows papillae that are lined by cells with Orphan Annie eye nuclei that are clear and nuclear grooves that are frequently found around psammoma bodies.
The prognosis of papillary thyroid carcinoma (PTC) is excellent.
The 10-year survival rate of papillary thyroid carcinoma (PTC) is greater than 95% despite the fact that this frequently spreads to cervical or neck lymph nodes.
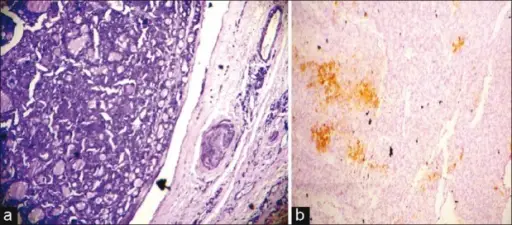
Medullary Thyroid Carcinoma
The malignant proliferation of parafollicular C cells, which makes up 5% of thyroid carcinomas, is known as medullary thyroid carcinoma.
Medullary thyroid carcinoma may result in high quantities of calcitonin and cause hypocalcemia.
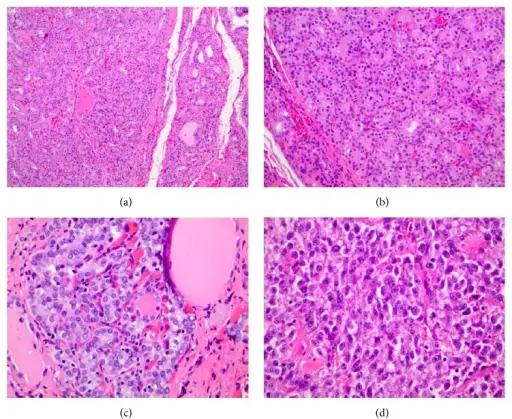
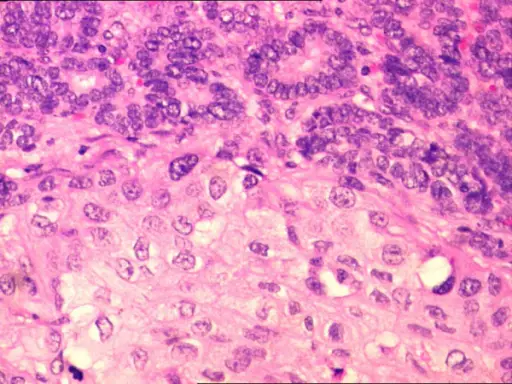
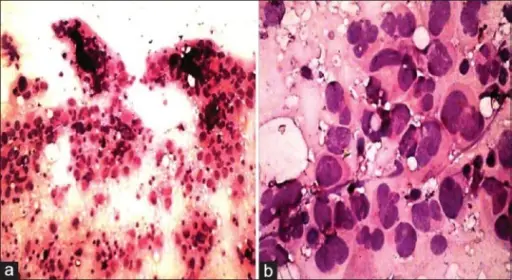
Histology of medullary thyroid carcinoma reveals sheets of malignant cells in a calcitonin derived amyloid stroma.
Multiple endocrine neoplasia (MEN) 2A and 2B, which are linked to mutations in the RET oncogene, are often the cause of familial cases of medullary thyroid carcinoma.
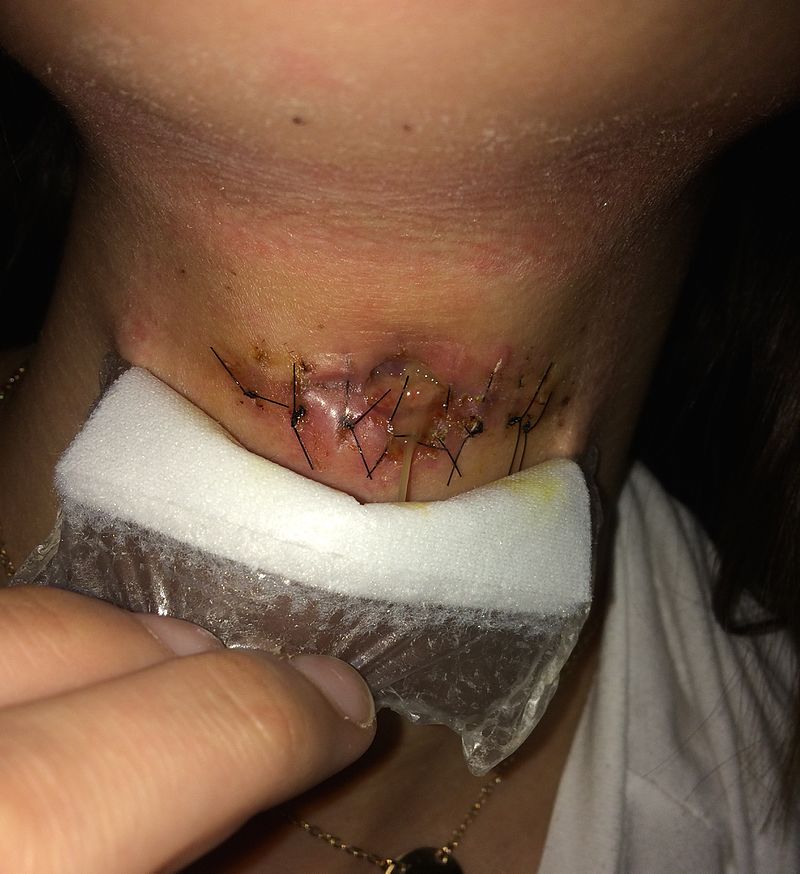
When the RET mutation is found, a prophylactic thyroidectomy is necessary.
Anaplastic Thyroid Carcinoma
An undifferentiated malignant thyroid tumor called anaplastic carcinoma is typically detected in older people.
Anaplastic carcinoma frequently infiltrates nearby structures, causing dysphagia or respiratory problems.
Anaplastic carcinoma has a poor prognosis.