Hypertension
A blood pressure of 140/90 mmHg or greater indicates high blood pressure, aka hypertension.
Hypertension can involve the pulmonary circulation, systemic circulation, or both.
Pulmonary hypertension refers to hypertension in the arteries that deliver blood from the heart to the lungs.
Systemic hypertension refers to hypertension in the arteries that deliver blood from the heart to the tissues of your body (except the lungs).
Normal blood pressure is less than 120 mmHg systolic and 80 mmHg diastolic.
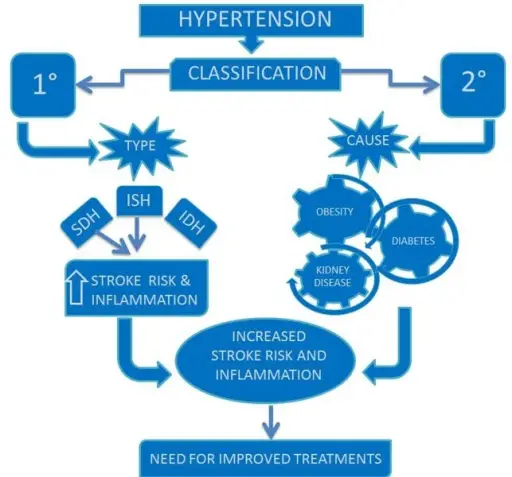
Based on the etiology, hypertension can be classified as primary or secondary.
Primary Hypertension
An unusually high blood pressure that is not brought on by a medical disease is referred to as primary hypertension.
95% of cases of hypertension are due to unknown causes, primary hypertension.
Risk factors for primary hypertension include:
- Age
- Obesity
- Stress
- Lack of exercise
- High salt diet
- Race (Americans of African descent > Caucasians > Asians)
Secondary Hypertension
Secondary hypertension is high blood pressure brought on by a specific illness or disorder.
Five percent of cases of hypertension are due to known causes, secondary hypertension.
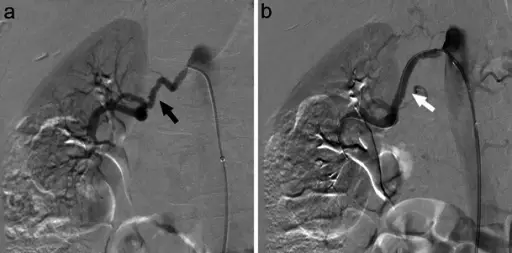
Renovascular hypertension, also known as renal artery stenosis, is a prevalent cause of secondary hypertension.
- In renovascular stenosis, stenotic vessels decreases blood flow to the glomeruli
- In response, the juxtaglomerular apparatus (JGA) secretes renin
- Renin secretion causes angiotensinogen to be converted to angiotensin
- Angiotensin converting enzyme (ACE) transforms angiotensin I into angiotensin (AT)
- Angiotensin causes the smooth muscle in the arteries to contract, which the total peripheral resistance, and in turn the blood pressure
- Additionally, it stimulates the secretion of aldosterone from the adrenal glands, which boosts sodium absorption in the distal convoluted tubule and raises plasma volume
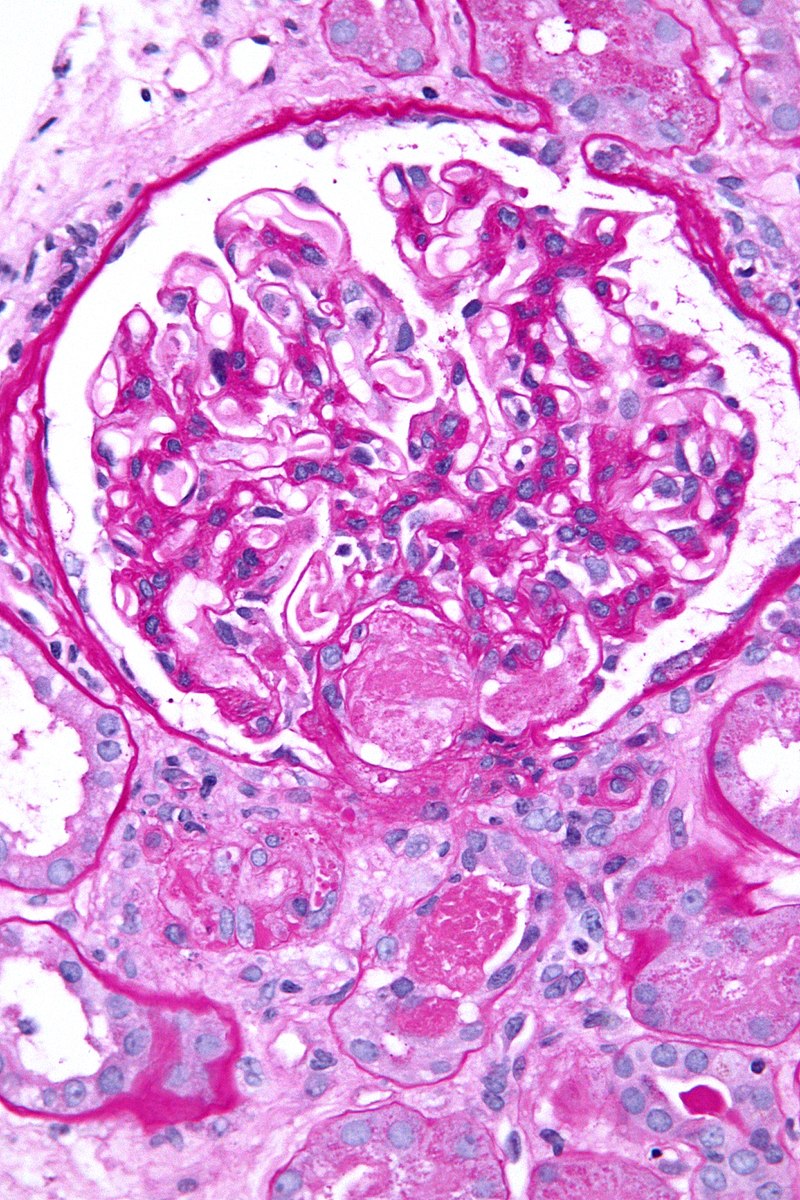
Renovascular hypertension causes unilateral renal atrophy (due to inadequate blood supply) and hypertension with elevated plasma renin levels.
Causes of renovascular stenosis include:
- Atherosclerosis
- Fibromuscular dysplasia
Atherosclerosis typically affects older men.
Fibromuscular dysplasia (FMD) characteristically affects younger women.
Fibromuscular dysplasia (FMD) is a developmental defect in the blood vessel wall that causes an irregularly thickened renal artery.
Benign Hypertension
Hypertension can be categorized as benign or malignant.
A mild to moderate increase in blood pressure is referred to as benign hypertension.
Most hypertension cases are benign.
Clinically speaking, benign hypertension is silent, causing organs and arteries to fail gradually over time.
Malignant Hypertension
Malignant hypertension is characterized by a blood pressure that is greater than 200/120 mmHg.
Less than 5% of cases of hypertension involve malignant hypertension.
Malignant hypertension may arise de novo or from preexisting benign hypertension.
Malignant hypertension is a medical emergency.
Malignant hypertension can cause severe end-organ damage such as:
- Acute renal failure
- Papilledema
- Stroke
- Hemorrhage