Uterus
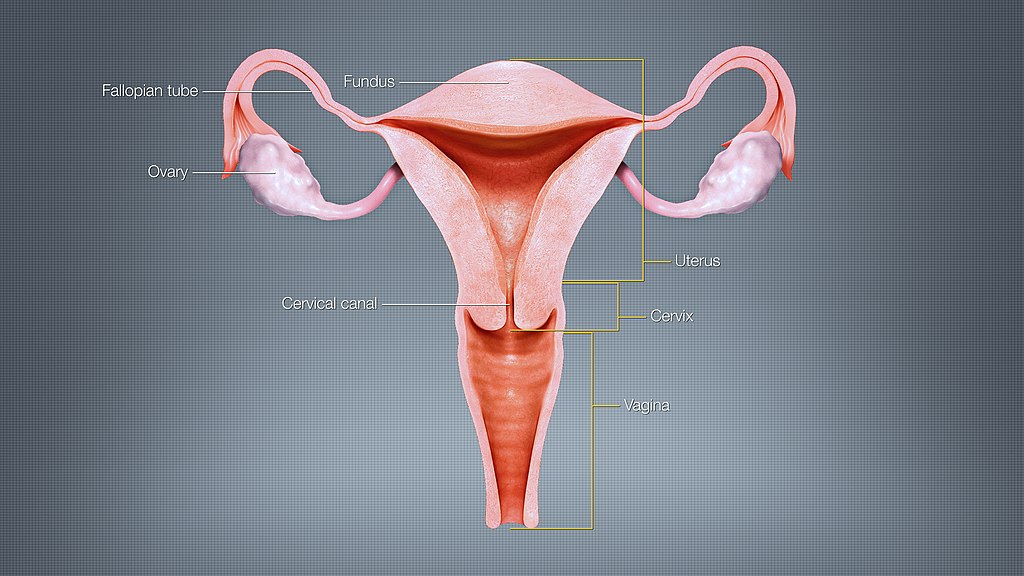
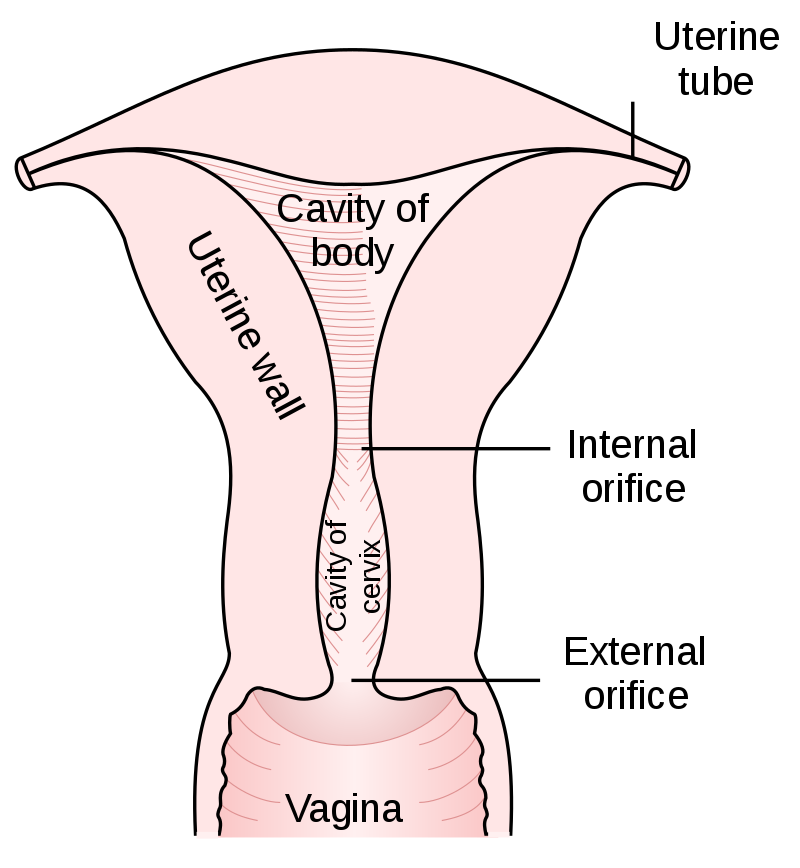
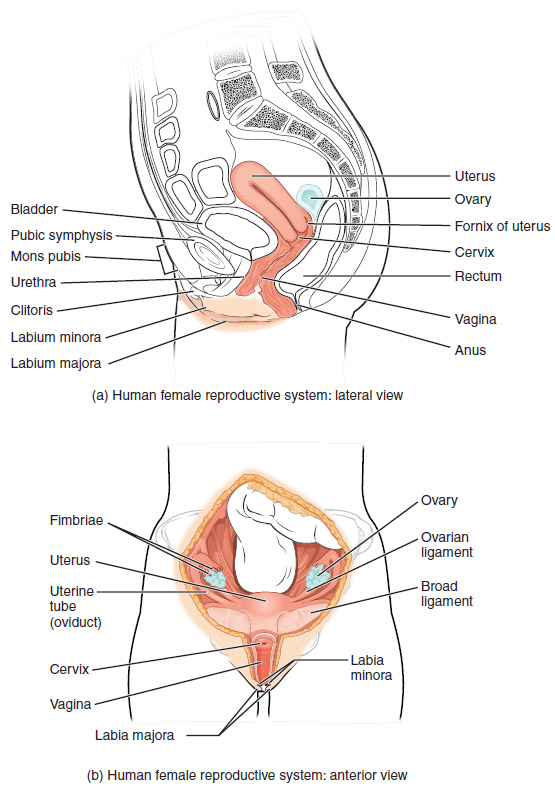
The uterus is responsible for incubating human life.
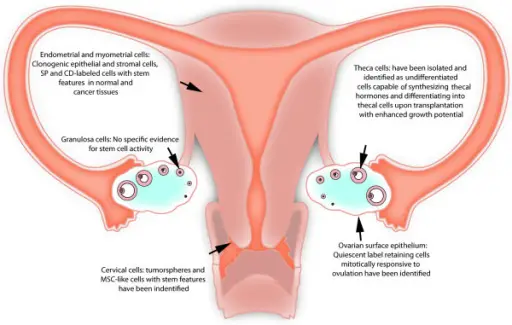
The mucosal lining of the uterus is called endometrium.
The endometrium is supported by a smooth muscular wall called the myometrium.
Hormonal sensitivity exists in the endometrium.
Estrogen drives the endometrium’s growth (proliferative phase).
Progesterone is responsible for preparing the endometrium for implantation (secretory phase).
Shedding happens when progesterone support is lost (menstrual phase).
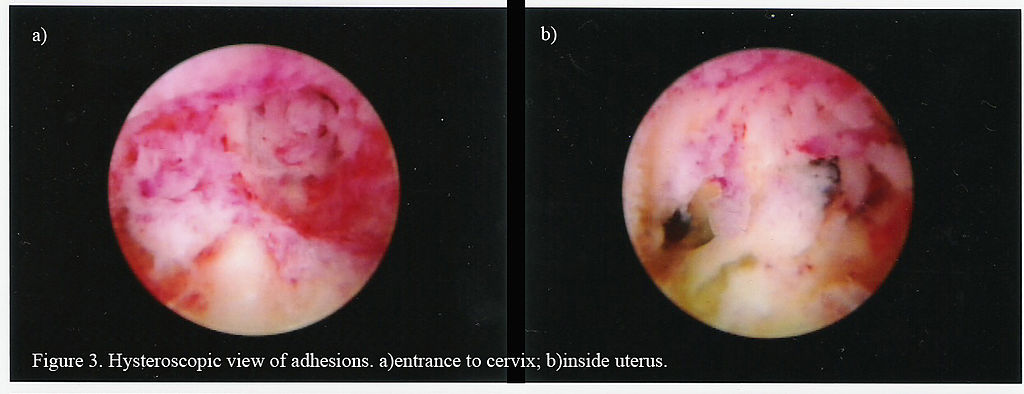
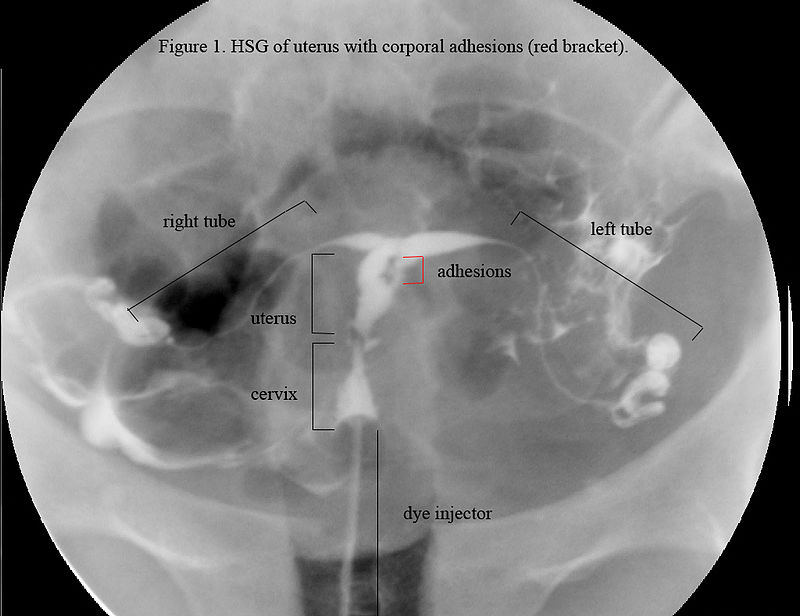
Asherman Syndrome
Asherman syndrome is secondary amenorrhea caused by the loss of the basal layer of the endometrium and scarring.
Asherman syndrome can be a complication of overaggressive dilation and curettage (D&C).
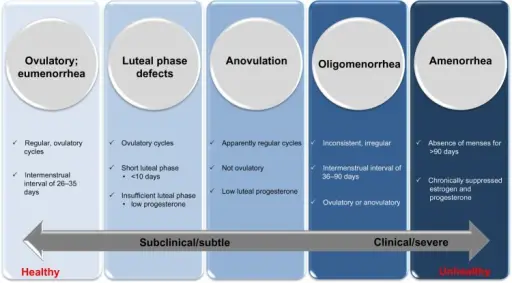
Anovulatory Cycle
An anovulatory cycle is a lack of ovulation.
An anovulatory cycle results in a proliferative phase driven by estrogen without a following secretory phase driven by progesterone.
Uterine bleeding results from the breakdown and shedding of proliferative glands.
Anovulatory cycle is a frequent reason for abnormal uterine bleeding, particularly around menarche and menopause.
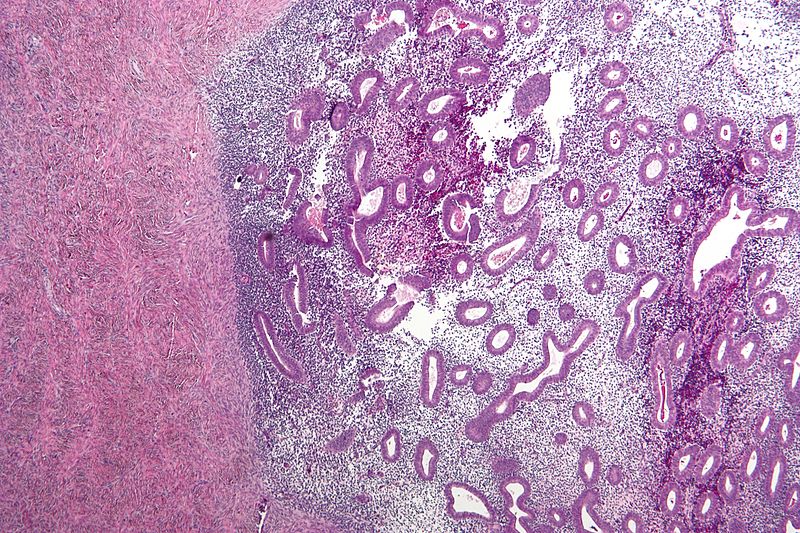
Acute Endometritis
Acute endometritis is typically secondary to bacterial infection of the endometrium.
After baby delivery or miscarriage there may be retained fetal products.
Retained fetal products serve as an infection nidus.
Symptoms of acute endometritis include:
- Fever
- Abnormal uterine bleeding (AUB)
- Pelvic pain
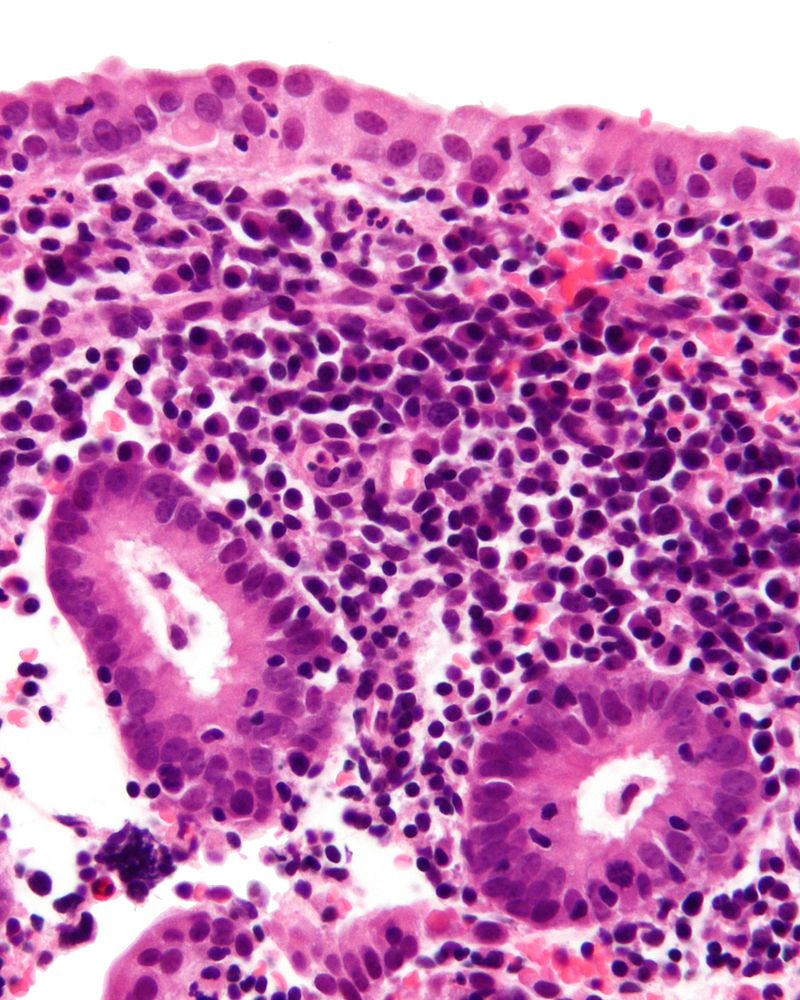
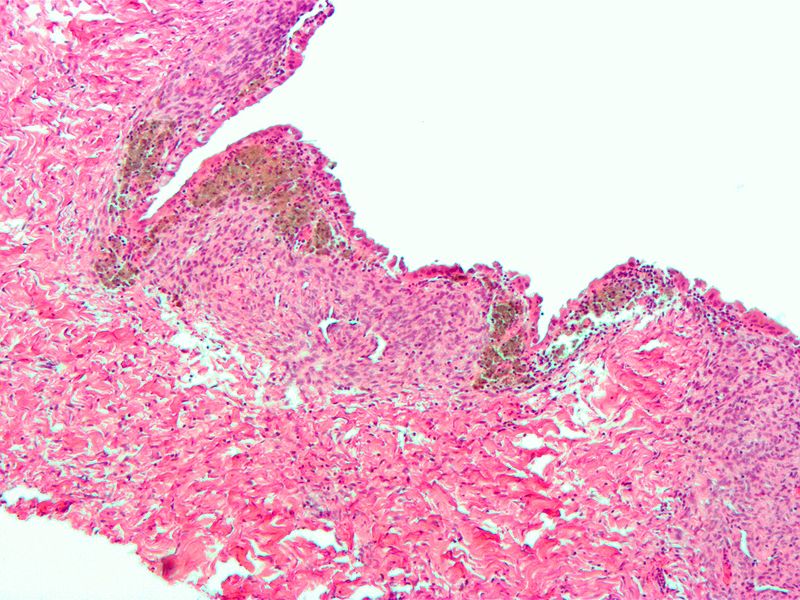
Chronic Endometritis
Chronic endometritis is inflammation of the endometrium.
Chronic endometritis is characterized by the presence of lymphocytes and plasma cells.
Given that lymphocytes are typically detected in the endometrium, plasma cells are required for the diagnosis of chronic endometritis.
Cause of chronic endometritis include:
- Retained fetal products of conception
- Chronic pelvic inflammatory illness
- Intrauterine device presence
Chronic endometritis presents as:
- Unusual uterine bleeding
- Pain
- Infertility
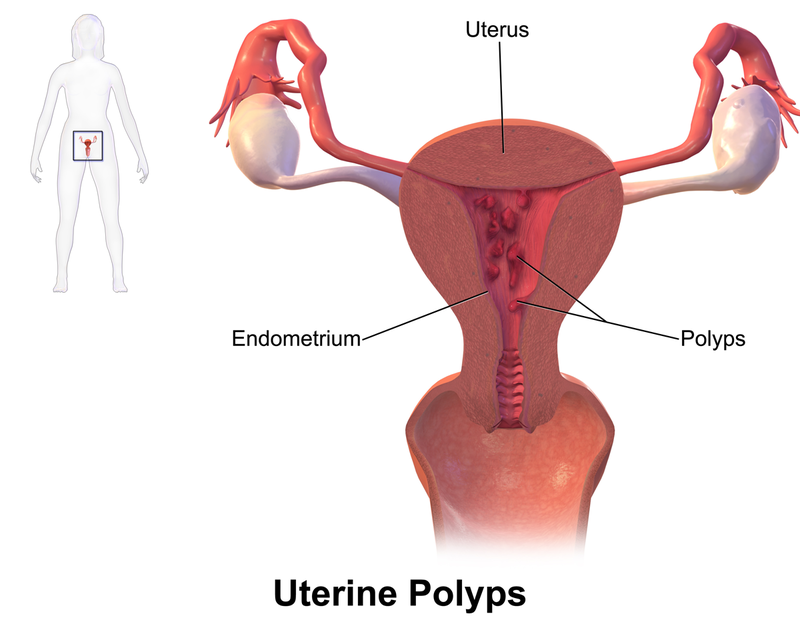
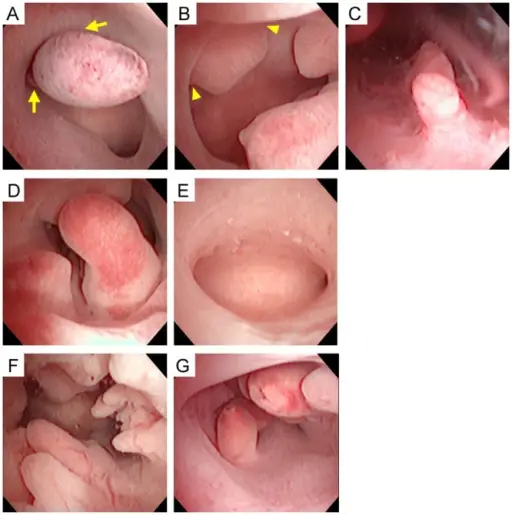
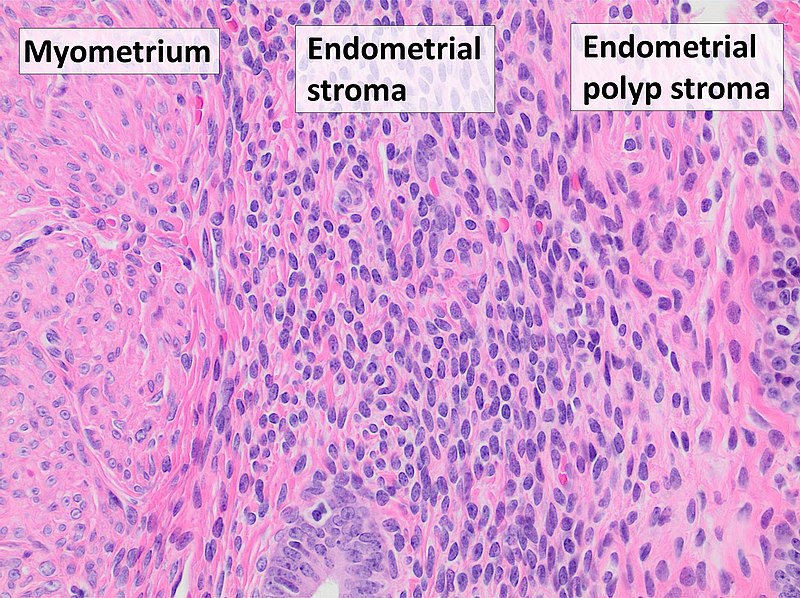
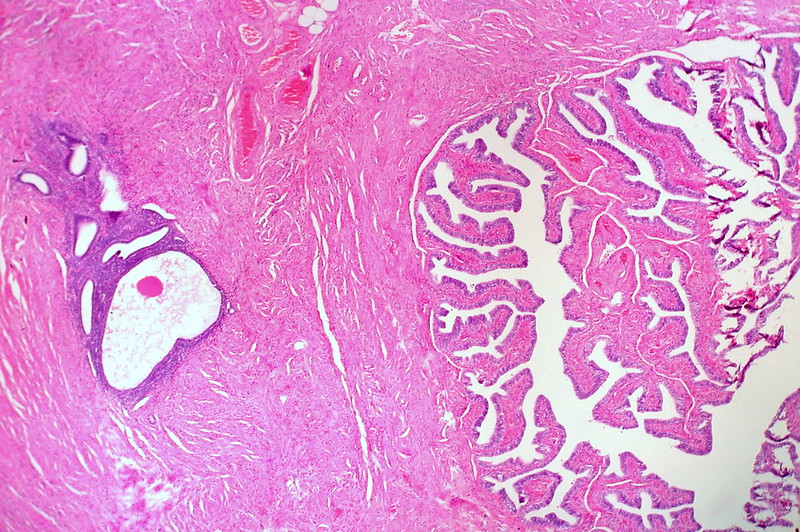
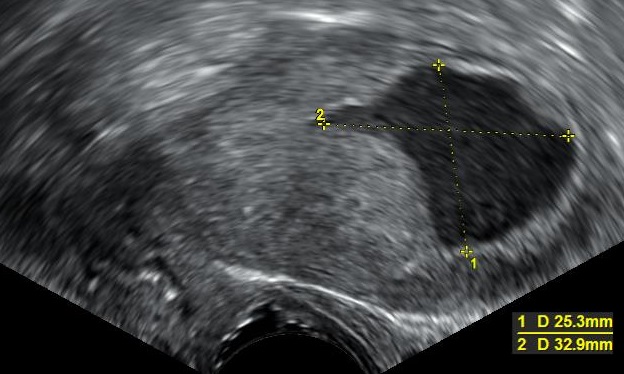
Endometrial Polyp
An endometrial polyp is a hyperplastic protrusion of endometrium.
Endometrium polyps presents as unusual uterine bleeding.
Endometrial polyps may develop from adverse side effects of medications such as tamoxifen, which has mild pro-estrogenic effects on the endometrium but anti-estrogenic effects on the breast.
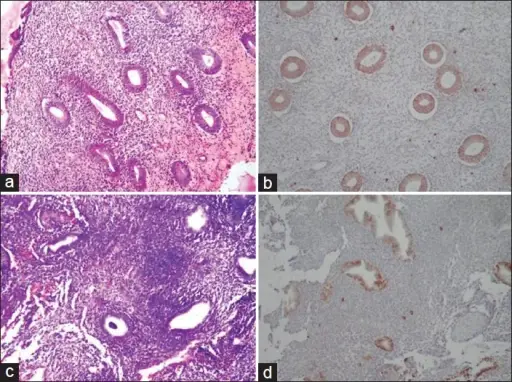
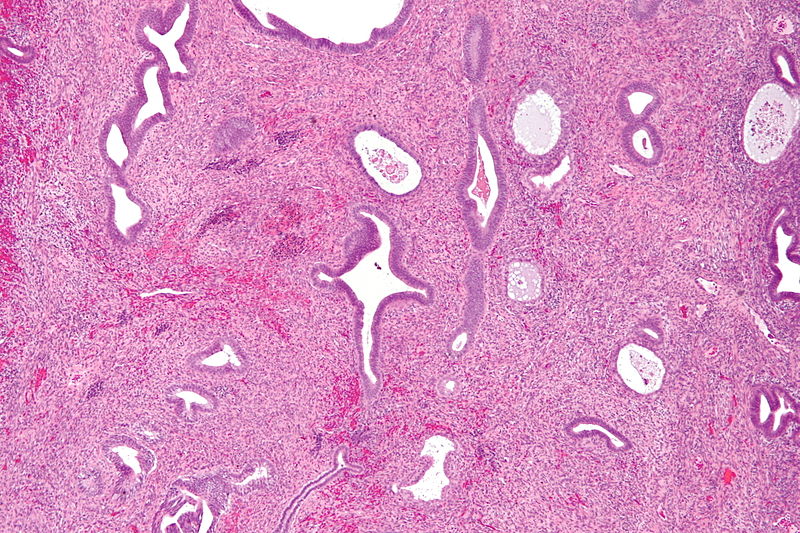
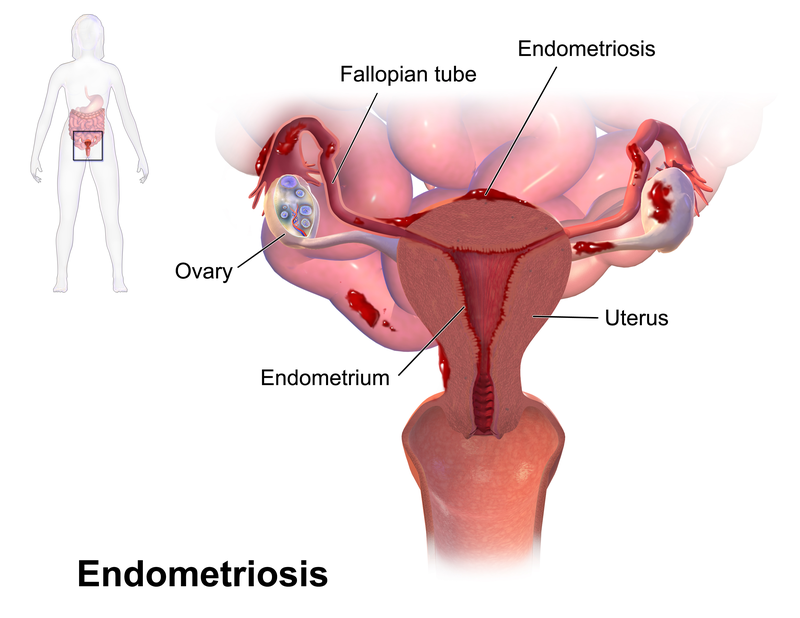
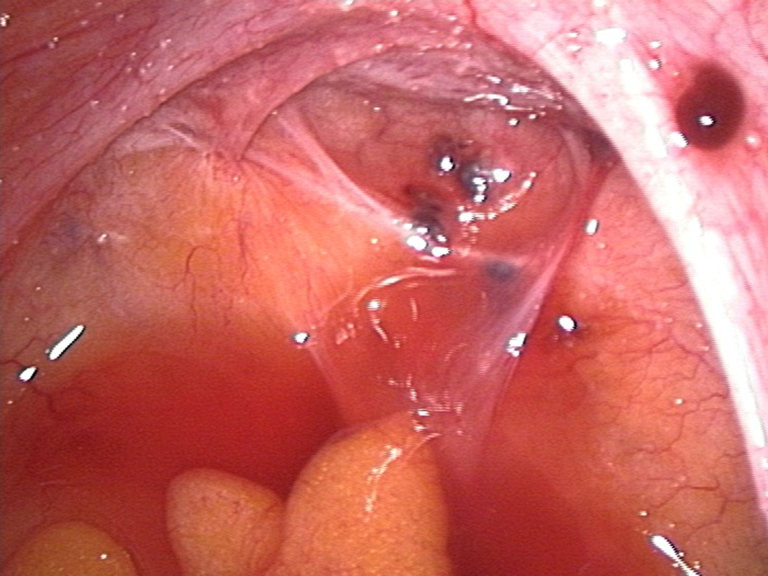
Endometriosis
Endometriosis occurs outside of the uterine cavity endometrial lining.
Endometriosis mostly occurs due to retrograde menstruation with implantation at an ectopic site.
Symptoms of endometriosis include:
- Pelvic discomfort
- Dysmenorrhea
Complications of endometriosis include:
- Infertility
- Pain while urinating
- Pain while defecating
- Scarring increases the risk for ectopic tubal pregnancy
Endometriosis cycles (the same way as normal endometrium).
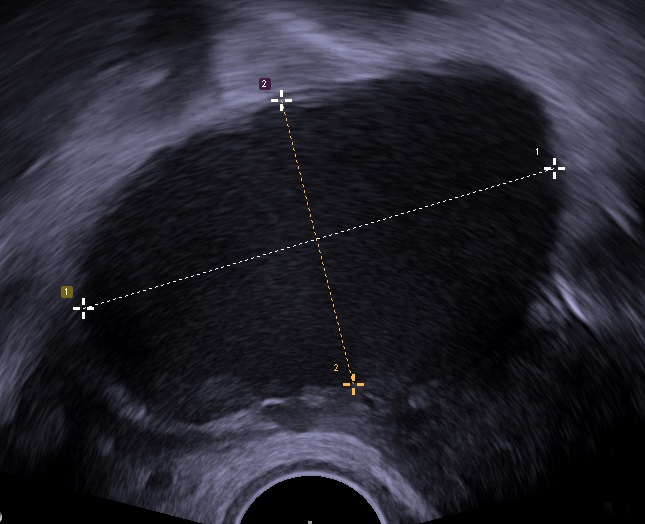
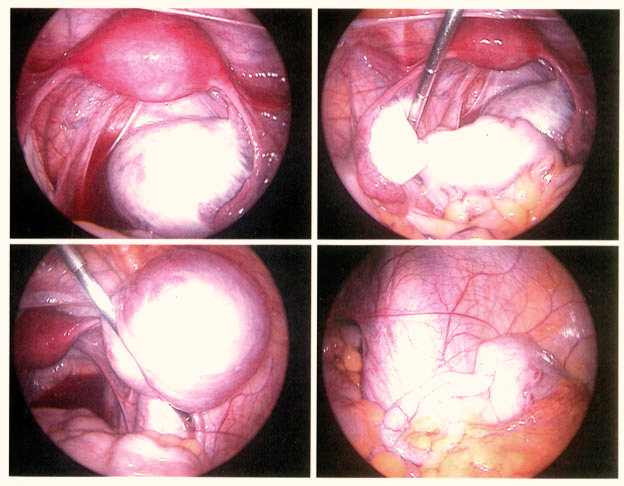
The ovary is the most frequently affected region by endometriosis, and this typically causes the development of a “chocolate” cyst.
Other sites of endometriosis involvement include:
- Fallopian tube mucosa
- Bladder wall
- Intestine serosa
- Pouch of Douglas
- Uterine ligaments
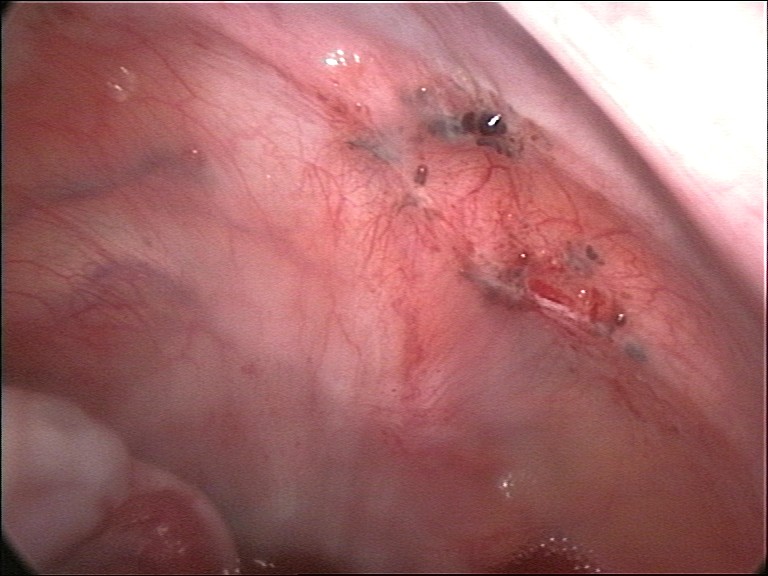
Traditionally, endometriosis implants look like yellow-brown “gun-powder” nodules.
Adenomyosis is the medical term for endometriosis involvement of the uterine myometrium.
At the site of endometriosis, particularly in the ovary, there is an elevated chance of developing endometrial adenocarcinoma.
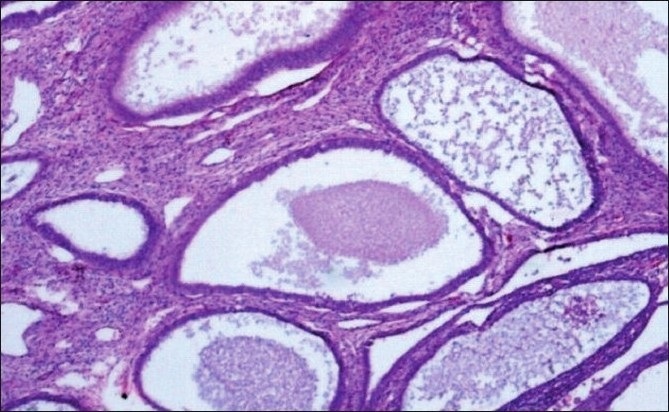
Endometrial Hyperplasia
Endometrial gland hyperplasia is excessive growth of the endometrium.
Endometrial hyperplasia occurs due to increased amounts of estrogen.
Increased estrogen may be present from:
- Obesity
- Polycystic ovary syndrome (PCOS)
- Estrogen replacement therapy
Endometrial hyperplasia typically manifests as uterine hemorrhage after menopause.
Histologically endometrial hyperplasia with cellular atypia is the most significant predictor of development to carcinoma.
Atypical simple hyperplasia frequently develops into cancer (30% of cases).
Complex hyperplasia without atypia, on the other hand, seldom develops into carcinoma (5% of cases).
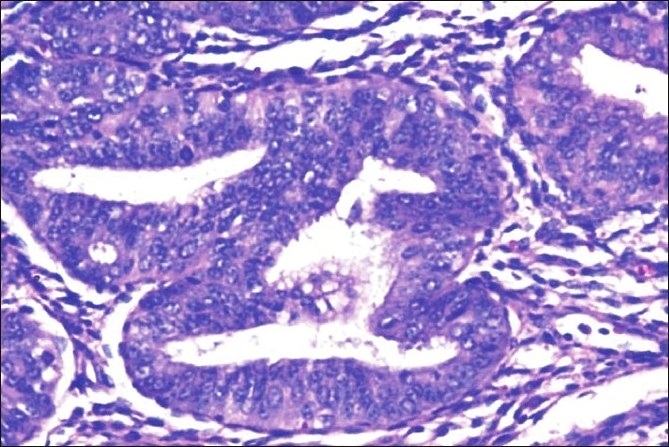
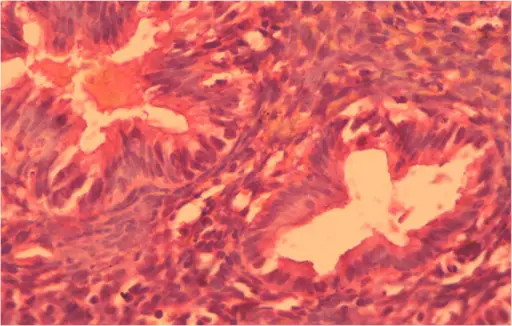
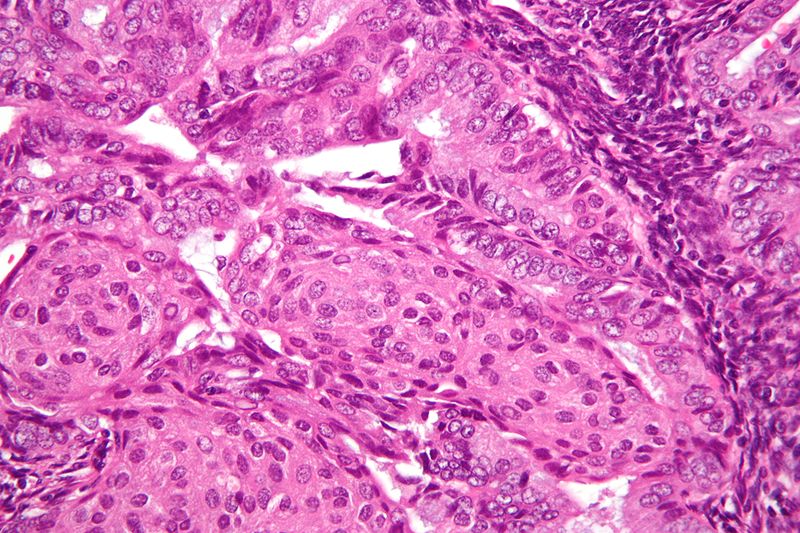
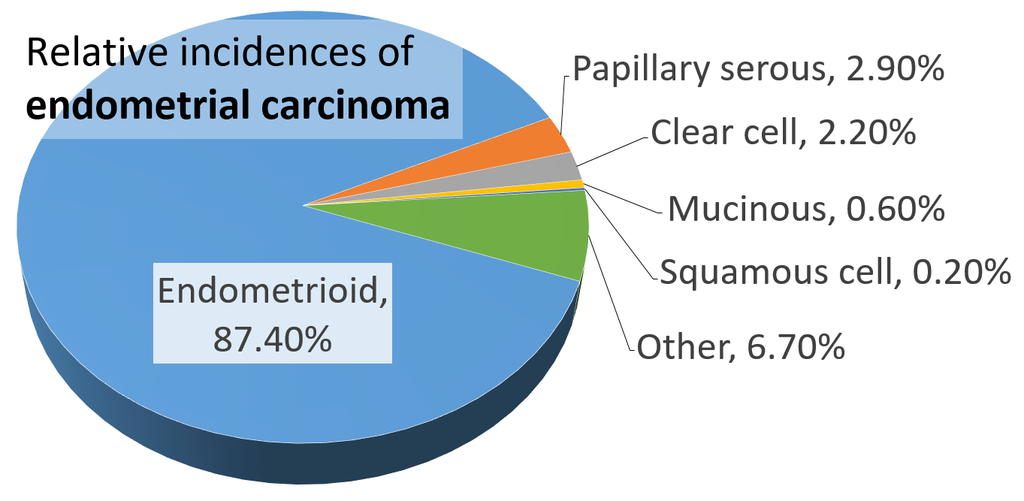
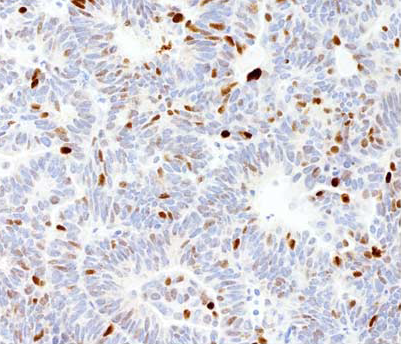
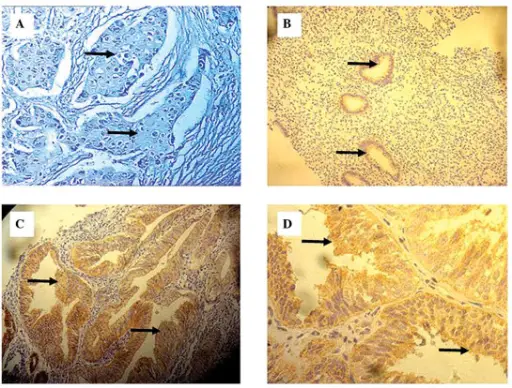
Endometrial Carcinoma
Endometrial carcinoma is the malignant proliferation of endometrial glands.
Endometrial carcinoma is a female vaginal tract invasive cancer, which is most prevalent.
Endometrial carcinoma presents as bleeding after menopause.
Endometrial carcinoma occurs through two different ways:
- Sporadic
- Hyperplastic
Carcinoma may develop from endometrial hyperplasia.
Risk factors for endometrial carcinoma are linked to estrogen exposure such as:
- Early menarche
- Late menopause
- Obesity
- Nulliparity
- Infertility with anovulatory cycles
Endometrial carcinoma typically presents around 60-years-old.
Histology of endometrial carcinoma is usually full of abnormal endometrioid cells.
In 25 percent of cases, the sporadic pathway, cancer develops in an atrophic endometrium without any obvious antecedent lesions.
P53 mutation is frequent, and the tumor behaves aggressively.
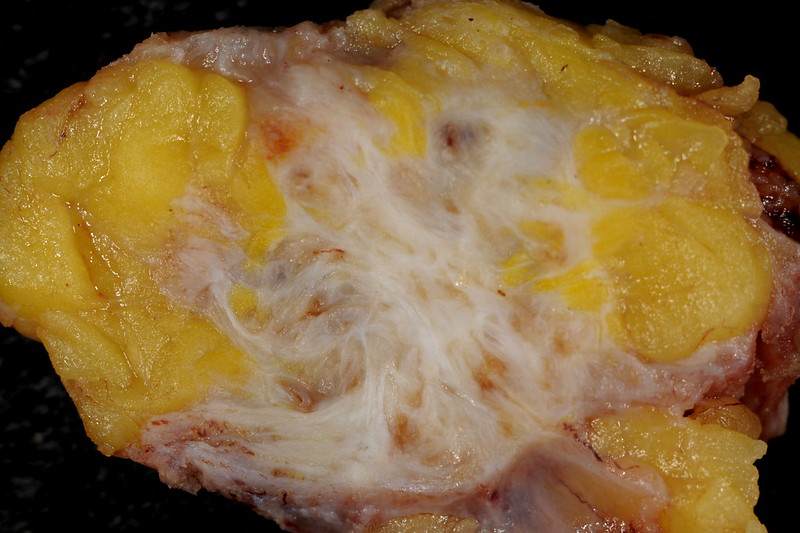
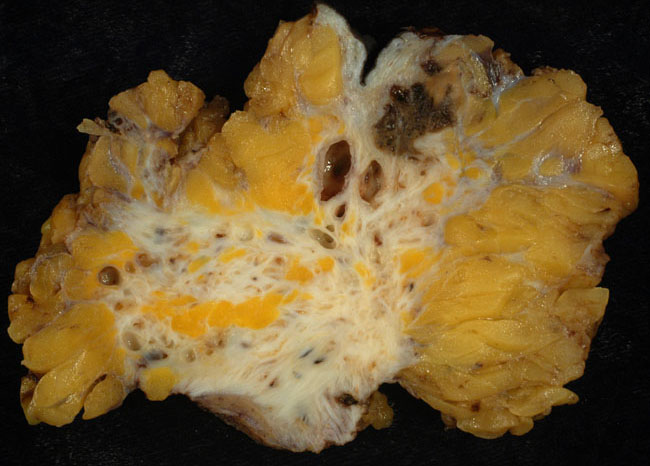
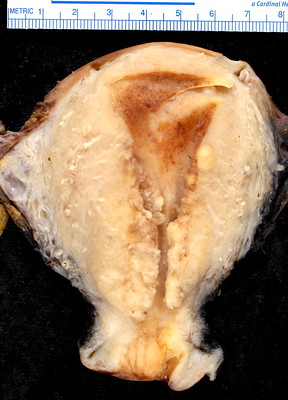
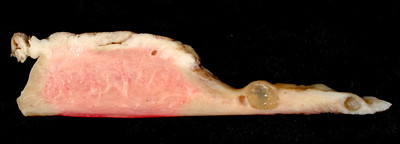
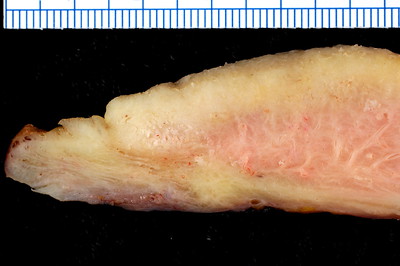
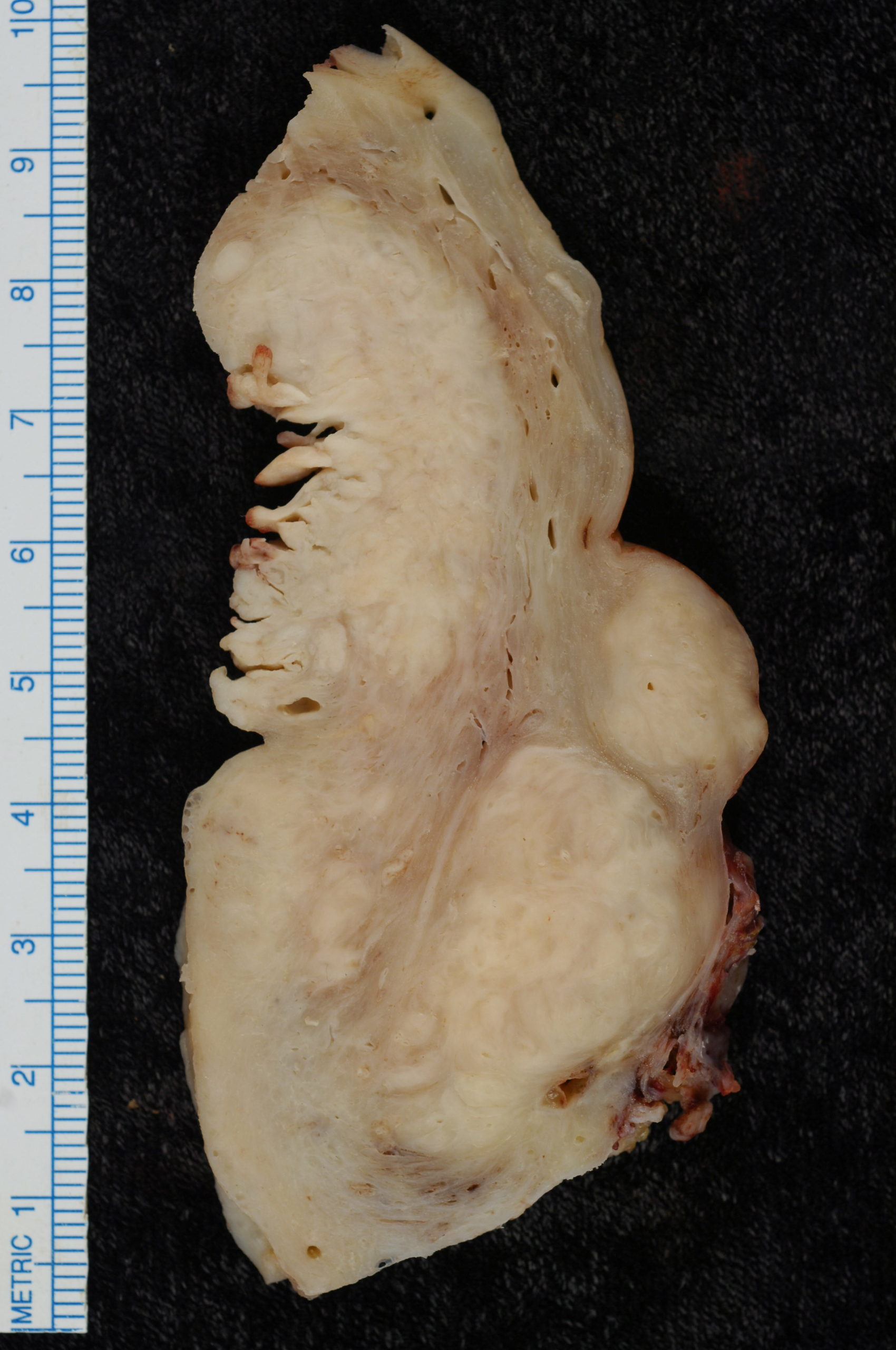
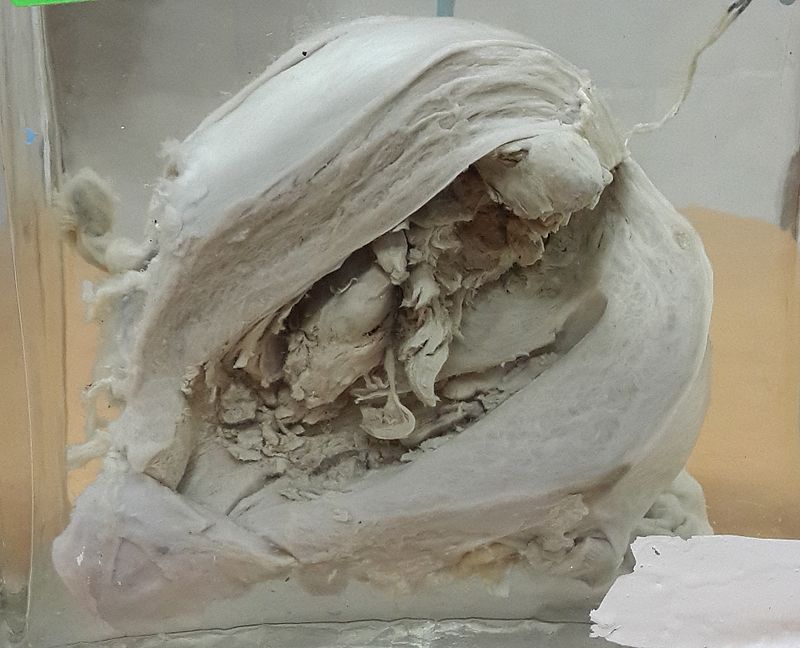
Leiomyoma
Leiomyomas are also called fibroids.
Leiomyomas are the most typical female tumor is a benign neoplastic growth of smooth muscle that arises from the myometrium.
Leiomyomas are associated with estrogen exposure.
Leiomyomas are prevalent in premenopausal females.
Leiomyomas may enlarge during pregnancy.
Leiomyomas shrink after menopause.
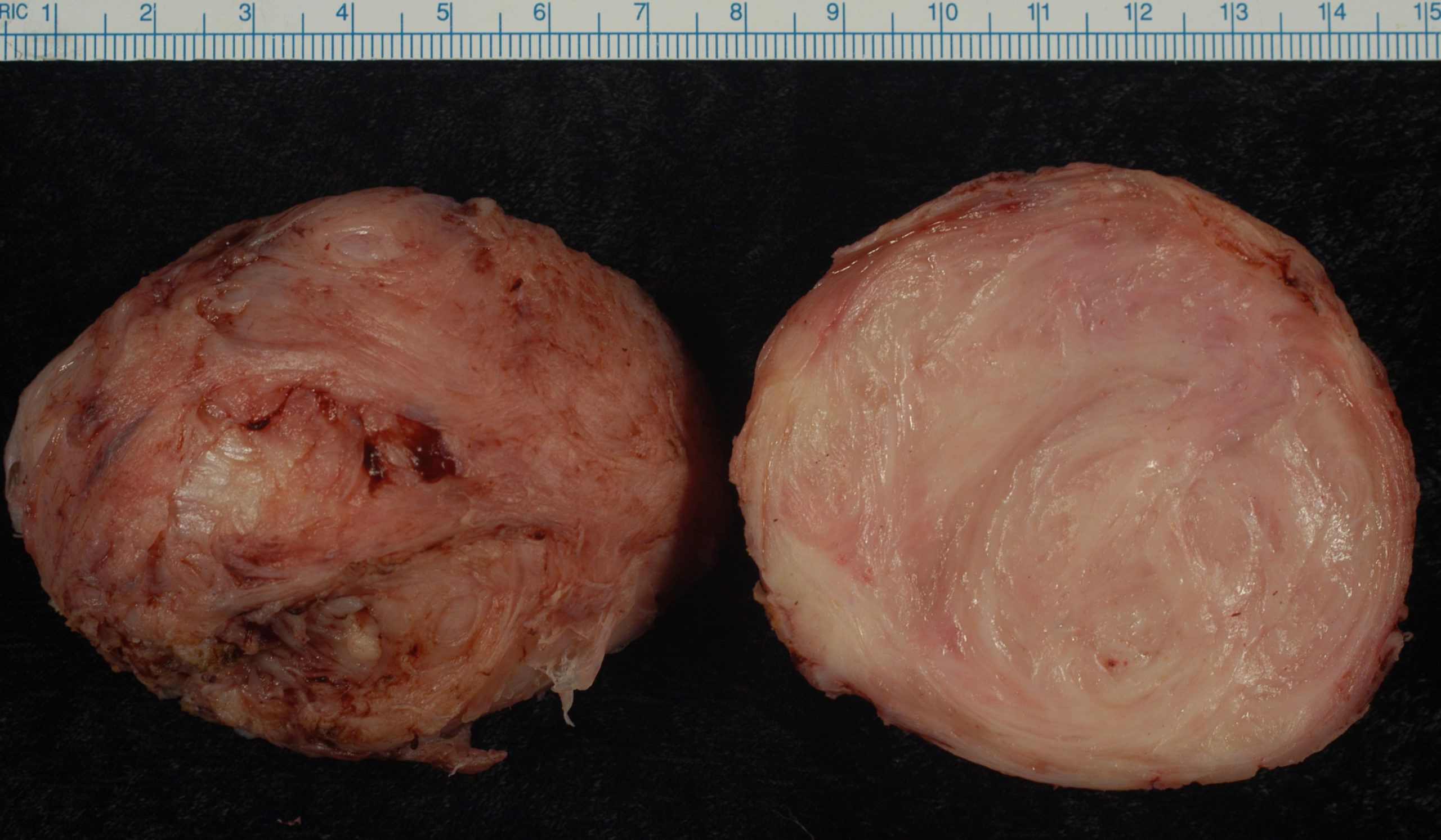
On a gross examination, leiomyomas have, white, whorled, round masses that could encroach on the pelvic tissues and deform the uterus.
Leiomyomas are typically asymptomatic.
When symptoms from leiomyomas exist they typically include:
- Abnormal uterine bleed (AUB)
- Abdominal distension
- Bloating
- Infertility
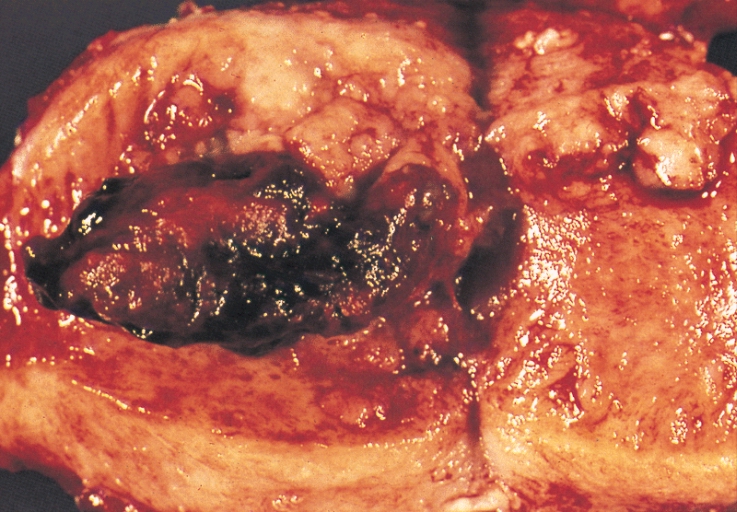
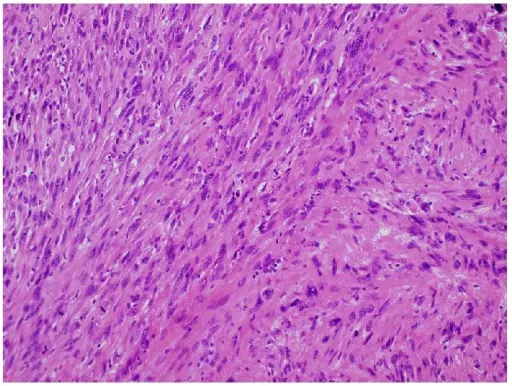
Leiomyosarcoma
Leiomyosarcomas are tumors of myometrial smooth muscle that have become malignant.
Leiomyosarcomas arises de novo.
Leiomyosarcomas do not develop from leiomyomas.
Leiomyosarcomas normally occur in postmenopausal females.
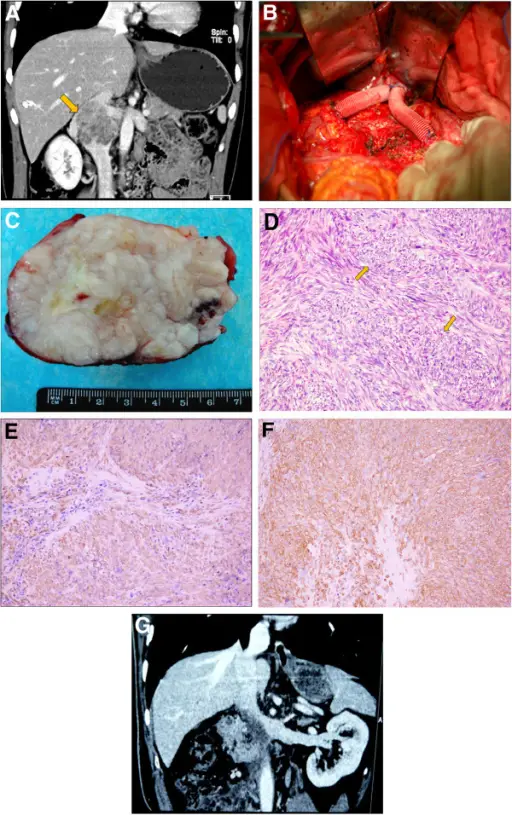
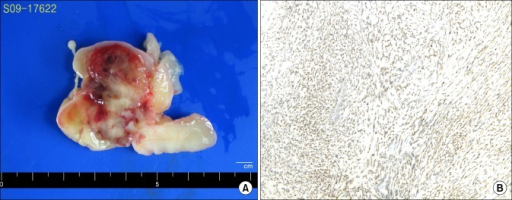
Leiomyosarcomas typically show a single lesion with areas of necrosis and bleeding is frequently visible on a gross exam.
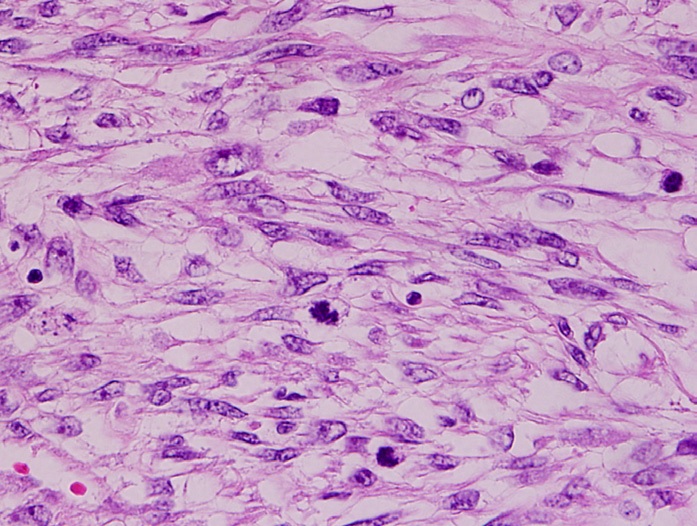
Histologic features of leiomyosarcomas include:
- Necrosis
- Multiple mitoses
- Cellular atypia