Nephrotic Syndrome Pathology Video
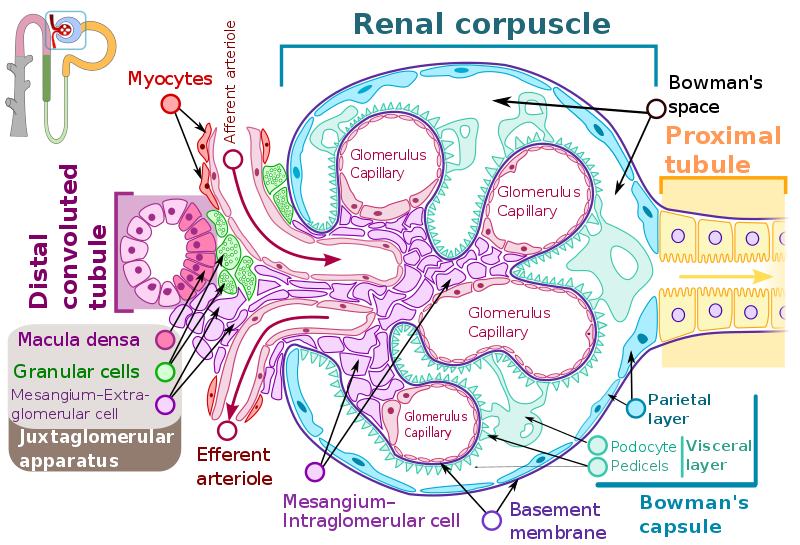
Nephrotic Syndrome
Nephrotic syndrome is characterized by proteinuria and glomerular disorders leading to hypoalbuminemia-pitting edema.
Nephrotic syndromes include:
- Minimal change disease
- Focal segmental glomerulosclerosis (FSGS)
- Membranous nephropathy
- Membranoproliferative glomerulonephritis (MPGN)
- Diabetes mellitus
- Systemic amyloidosis
Complications of nephrotic syndrome includes:
- Hypogammaglobulinemia increases the risk of infection
- Hypercoagulable state because of loss of antithrombin I (fibrin)
- Hyperlipidemia
- Hypercholesterolemia
Minimal Change Disease
Minimal change disease is the most prevalent cause of nephrotic syndrome in children.
Minimal change disease is typically idiopathic.
Minimal change disease can be linked to Hodgkin lymphoma.
The kidney histology looks normal in minimal change disease (“minimal change” disease).
Electron microscopy is needed to see the pathology of minimal change disease.
Electron microscopy of minimal change disease shows podocyte foot effacement.
Selective proteinuria may be present because loss of albumin, but not immunoglobulin.
Minimal change disease is treated with steroids.
Focal Segmental Glomerulosclerosis (FSGS)
Focal segmental glomerulosclerosis (FSGS) is the most common cause of nephrotic syndrome.
Ethnicities at risk of focal segmental glomerulosclerosis (FSGS) include:
- Hispanics
- Americans of African descent
Focal segmental glomerulosclerosis (FSGS) can be linked to HIV infection, heroin use, and sickle cell disease.
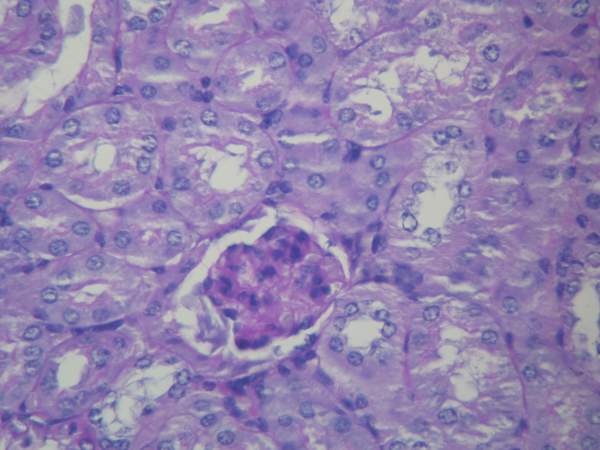
Histology of focal segmental glomerulosclerosis (FSGS) shows segmental (some glomeruli) and focal (part of effected glomeruli) fibrosis and sclerosis.
There are no immune complex deposits associated with focal segmental glomerulosclerosis (FSGS).
Treatment of focal segmental glomerulosclerosis (FSGS) is steroids.
If focal segmental glomerulosclerosis (FSGS) does not respond to steroid treatment that portends to a worse diagnosis.
Chronic renal failure is a complication of focal segmental glomerulosclerosis (FSGS).
Membranous Nephropathy
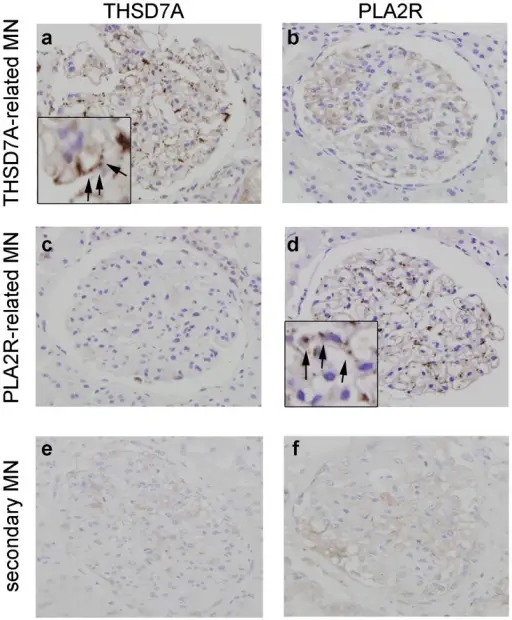
Membranous nephropathy is the most common cause of nephrotic syndrome in Caucasian adults.
Membranous nephropathy is normally idiopathic.
Known causes of membranous nephropathy include:
- Hepatitis B
- Hepatitis C
- Cancer
- Systemic lupus erythematous (SLE)
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Penicillamine
- Systemic lupus erythematous
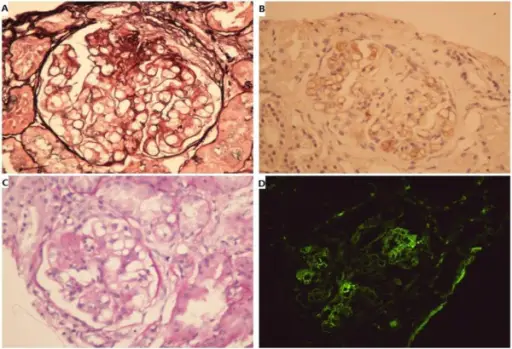
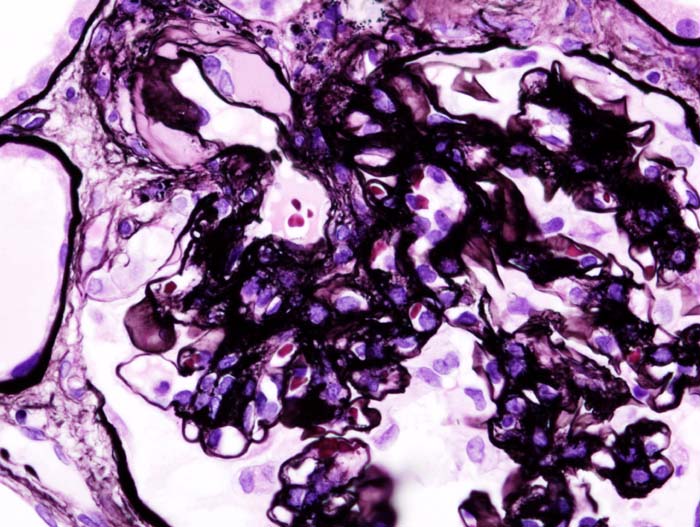
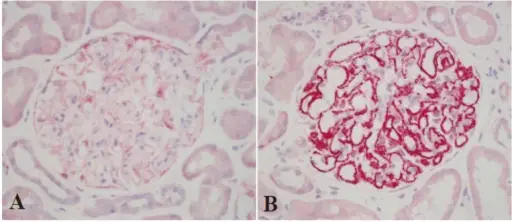
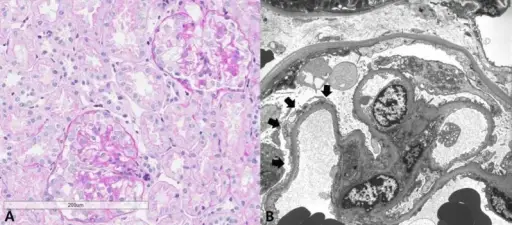
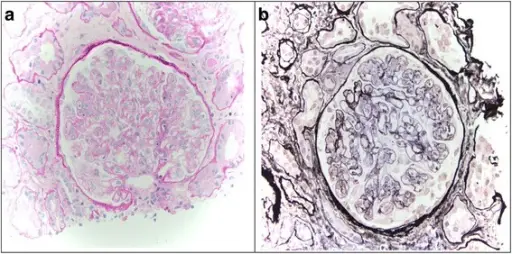
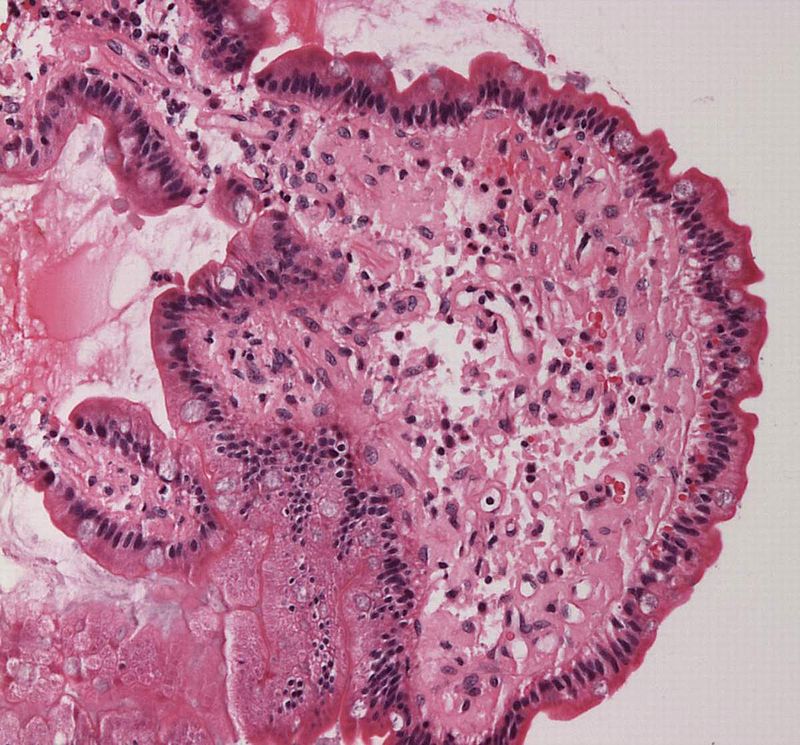
Histology of membranous nephropathy shows glomerular basement membrane thickening.
A periodic acid Schiff (PAS) stain may highlight the thickened basement membrane dark pink.
Electron microscopy of membranous nephropathy shows subepithelial deposits with spike and dome appearance due to immune complex deposition.
Chronic renal failure may develop as a complication of membranous nephropathy.
Membranoproliferative Glomerulonephritis (MPGN)
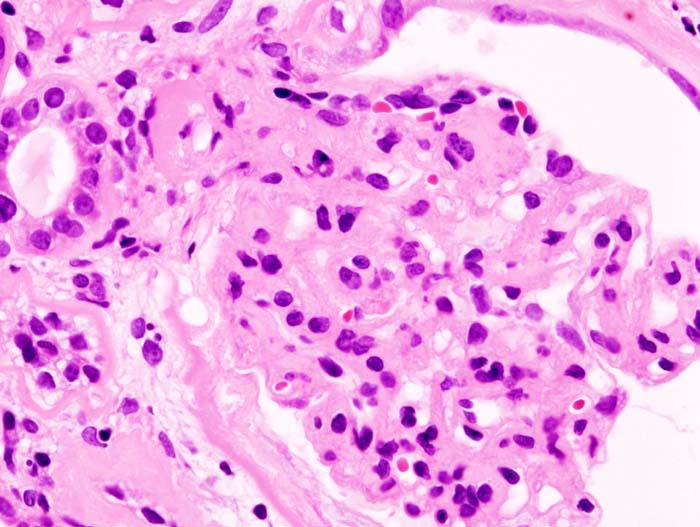
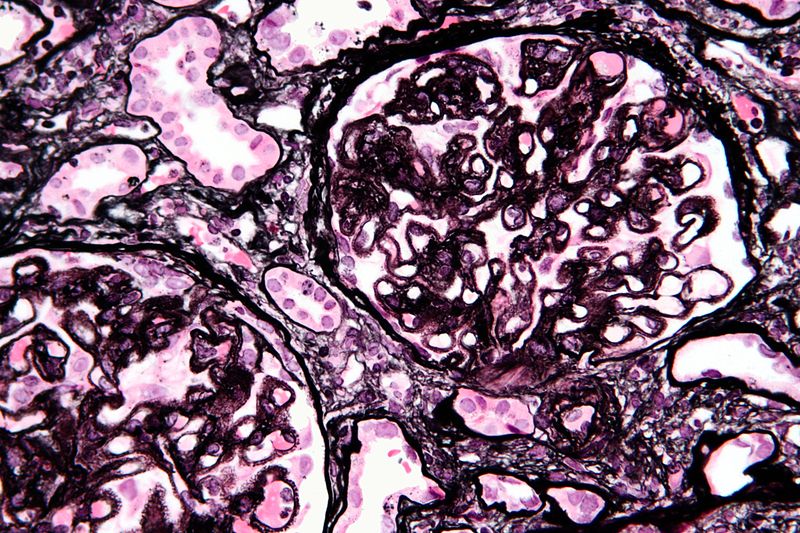
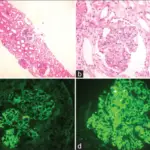
Membranoproliferative glomerulonephritis (MPGN) classically shows a thick glomerular basement membrane on H&E that looks like a “tram-track.”
The tram track appearance of membranoproliferative glomerulonephritis (MPGN) is present because immune complex deposition.
Immunofluorescence of membranoproliferative glomerulonephritis (MPGN) shows immune complex deposition.
The immune complex deposition of membranoproliferative glomerulonephritis (MPGN) is classified into two types based on the location of deposits:
- Type 1 subendothelial (associated with HBV and HCV)
- Type 2 dense deposit disease (which is intramembranous associated with C3 nephritic factor)
Membranoproliferative glomerulonephritis (MPGN) may progress to chronic renal failure.
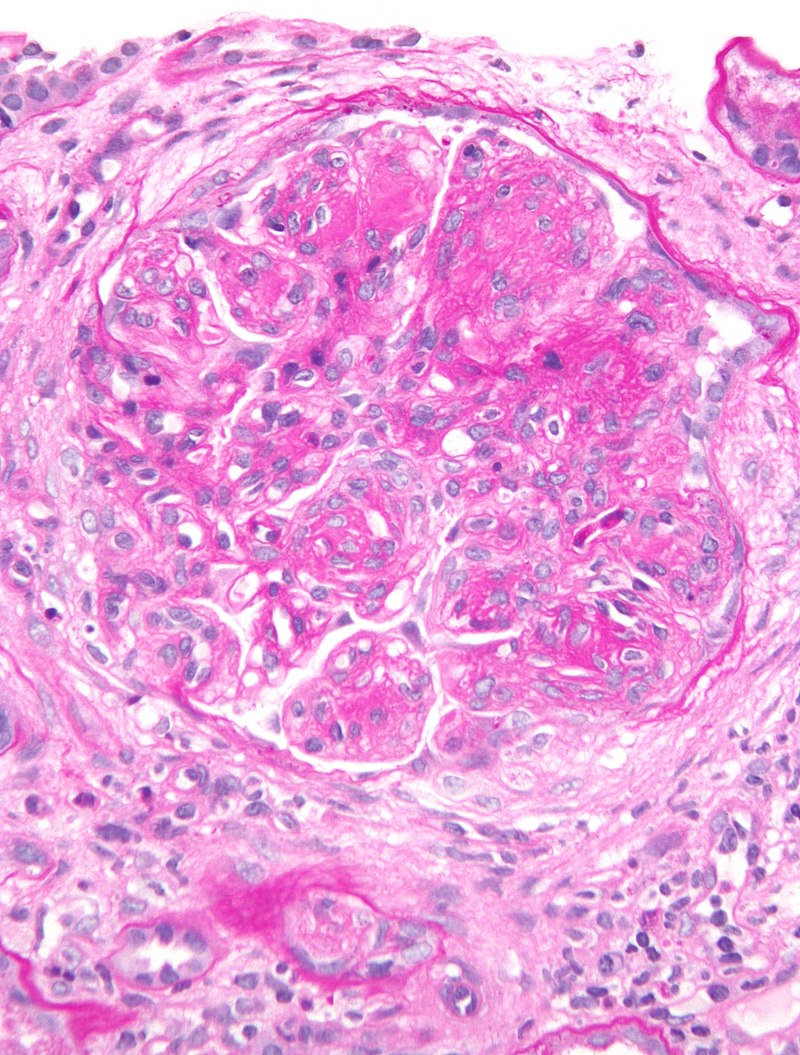
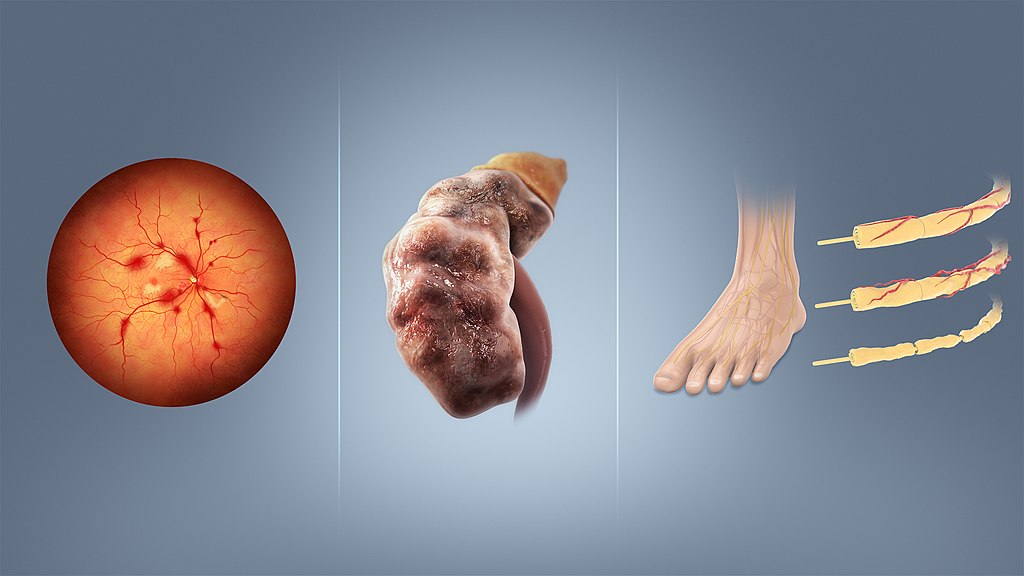
Diabetes Mellitus
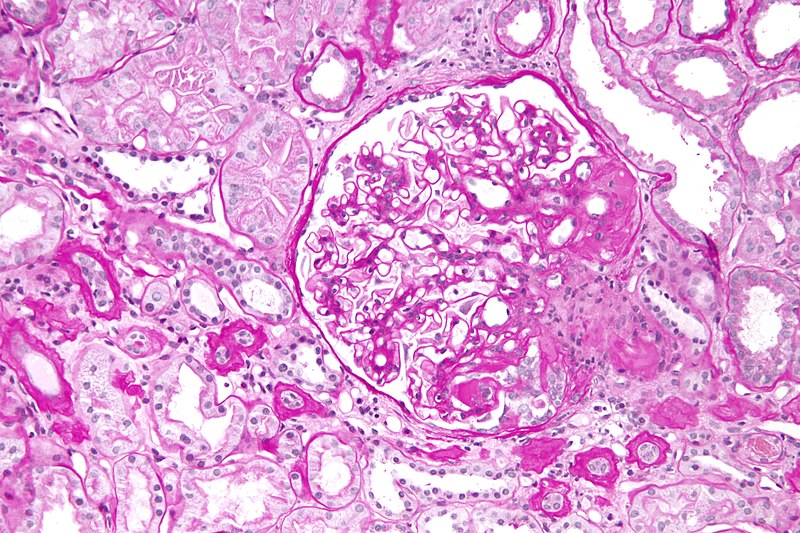
High serum glucose levels in patients with diabetes mellitus causes the vascular basement membrane to be glycosylated non-enzymatically, which results in hyaline arteriolosclerosis.
The glomerular efferent arteriole is more impacted than afferent arteriole, resulting in increased glomerular filtration pressure.
Hyperfiltration injury may result in microalbuminuria and nephrotic syndrome.
Diabetes mellitus causes cirrhosis of the mesangium with formation of Kimmelstiel-Wilson nodules.
Diabetes mellitus induced hyaline arteriolosclerosis is treated with angiotensin converting enzyme (ACE) inhibitors.
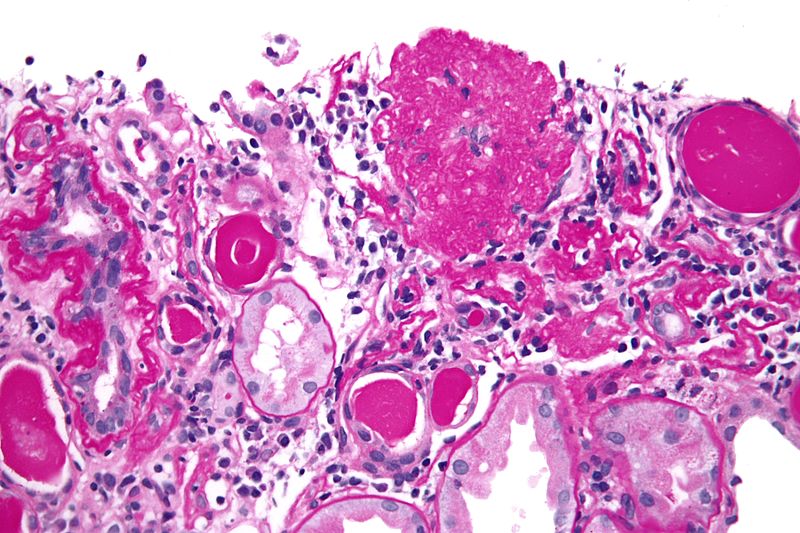
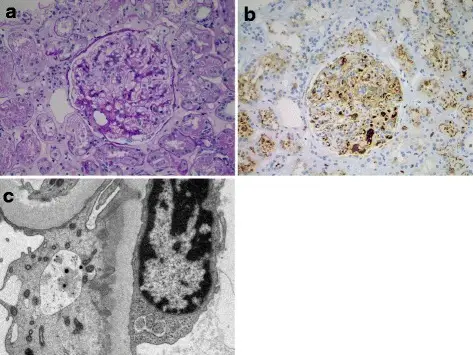
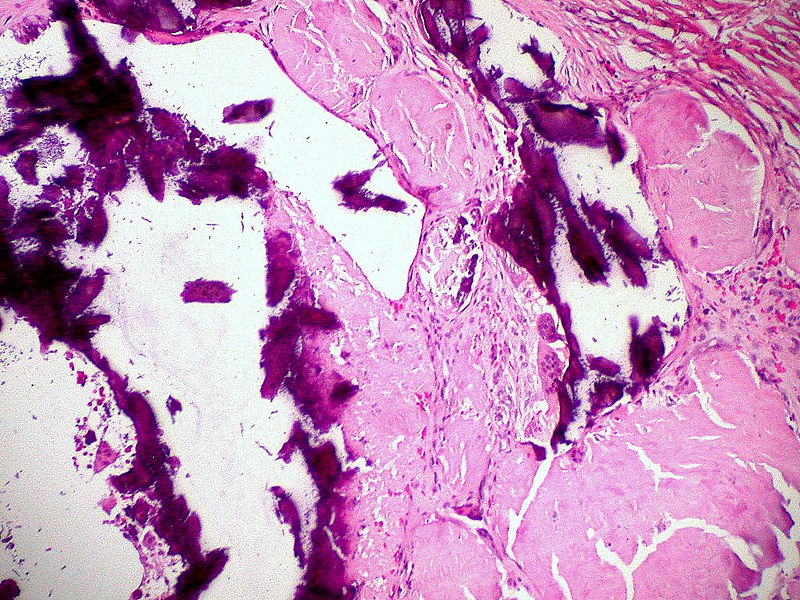
Systemic Amyloidosis
The kidney is the organ that is most often involved by systemic amyloidosis.
Systemic amyloidosis is characterized by deposits in the mesangium which can cause nephrotic syndrome.