Cell Injury
When stress exceeds a cell’s ability to adapt, cell injury may occur.
The likelihood of cellular injury occurring depends on:
- The type(s) of cells involved
- The type(s) of stress
- The severity of stress(ors)
- The duration of the stress(ors)
Please note that neurons are extremely sensitive to ischemia.
Please note that compared to neurons, skeletal muscle cells are less sensitive to ischemia.
Acute injury can result from acute ischemia such as a stroke.
Atrophy can result from slowly developing ischemia such as renal artery atherosclerosis leading to atrophic kidney.
Common causes of cellular injury include:
- Inflammation
- Nutritional deficiency
- Nutritional excess
- Hypoxia
- Trauma
- Genetic issues
Hypoxia
Hypo- means low.
-oxia means oxygen.
Hypoxia means low oxygen.
Tissues are dependent on oxygen for the generation of ATP.
Hypoxia may result in low oxygen delivery to tissue.
Hypoxia is an important cause of cellular injury.
Oxygen is the final electron acceptor in the electron transport chain.
Decreased oxygen impairs oxidative phosphorylation.
Decreased oxygen results in decreased ATP production.
Lack of ATP leads to cellular injury.
Causes of hypoxia include:
- Ischemia
- Hypoxemia
- Decreased oxygen carrying capacity
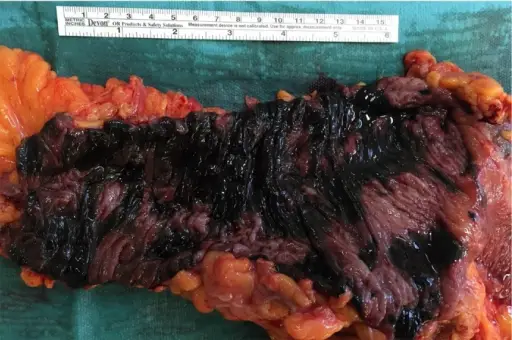
Ischemia
Ischemia is decreased blood flow through an organ.
Ischemia can be due to decreased arterial perfusion (e.g. atherosclerosis).
Ischemia can be due to decreased venous drainage (e.g. Budd-Chiari syndrome).
Ischemia can be due to shock (generalized decrease perfusion of organs).
Types of shock include:
- Hypovolemic shock
- Neurogenic shock
- Septic shock
- Cardiogenic shock
- Anaphylactic shock
Hypoxemia
Hypoxemia is technically a lower partial pressure of oxygen in the blood.
Remember from lung physiology that FiO2 -> PAO2 -> PaO2 -> SaO2.
The specific partial pressure that defines hypoxemia is:
- PaO2 < 60 mm Hg
- SaO2 < 90%
Hypoxemia can be caused by:
- Hypoventilation (e.g. carbon dioxide build-up in lung -> increased PACO2)
- V/Q mismatch
- High altitude (e.g. FiO2 decreased)
- Diffusion defect (e.g. thickened alveolar air sacks in interstitial fibrosis of the lung)
- Decreased oxygen carrying capacity (e.g. anemia PaO2 & SaO2 both are normal or carbon monoxide (CO) poisoning PaO2 normal & SaO2 decreased, methemoglobinemia PaO2 normal & SaO2 decreased)
Carbon Monoxide Poisoning
Carbon monoxide (CO) binds hemoglobin stronger than oxygen binds hemoglobin.
PaO2 normal & SaO2 decreased
Carbon monoxide poisoning can be due to:
- Engine exhaust inhalation (e.g. suicide attempt in car)
- Smoke inhalation from fire
Classic symptoms of carbon monoxide poisoning include:
- Headache early on in exposure
- Cherry red skin
Prolonged carbon monoxide exposure can lead to coma, and even death.
Methemoglobinemia
Heme contains iron.
The iron in heme can be oxidized to Fe3+.
Fe3+ cannot bind oxygen.
Patients with methemoglobinemia will have:
- Normal PaO2
- Decreased SaO2
Drugs that may cause methemoglobinemia are classically oxidant stresses which include:
- Sulfa drugs
- Nitrite drugs (e.g. “poppers”)
Newborns are at increased risk of methemoglobinemia.
Clinical signs of methemoglobin include:
- Chocolate colored blood
- Cyanosis
Methemoglobinemia is treated with methylene blue which is administered intravenously.
Methylene blue helps reduce Fe3+ back to the Fe2+ state.
Oxygen can bind easier to Fe2+.
Reversible Cell Injury
Hypoxia results in decreased ATP due to the oxidative phosphorylation chain being negatively impacted.
Low ATP negatively effects:
- Na+-K+ pump
- Ca2+ pump
- Aerobic glycolysis
Decreased ATP results in issues with cellular function which include:
- Cell swelling
- Calcinosis
- Lactic acid buildup
Cell swelling occurs due to the sodium potassium pump not having the ATP needed to function, which results in sodium accumulating in the cell.
Calcinosis occurs due to the Ca2+ pump not having the ATP needed to function.
Hypoxia causes the metabolic machinery of the cell to shift from aerobic glycolysis to anaerobic glycolysis.
Anaerobic glycolysis produces lactic acid.
Lactic acid accumulates in the cell, and lowers the cell pH, which causes denaturation of proteins.
The initial phase of hypoxic injury is reversible.
Key features of reversible cell injury includes:
- Cellular swelling
- Loss of microvilli
- Membrane blebbing
- Decreased protein synthesis
Irreversible Cell Injury
The characteristic feature of irreversible cellular injury is membrane damage, which includes:
- Cellular membrane damage
- Mitochondrial membrane damage
- Lysosome membrane damage
Please note that membrane damage is the key feature of irreversible cell injury.
When the cellular membrane is damaged cytosolic enzymes are capable of leaking out of the cell into the blood and serum.
Please note that troponin testing for myocardial infarction is based on detecting intracellular components of myocardiocytes that have leaked into the blood and serum via cardiac cell membranes that were damaged due to hypoxia or ischemia.
Regarding mitochondrial membrane damage, the electron transport chain would be negatively impacted, and cytochrome C would leak out into the cytosol causing apoptotic activation.
Regarding lysosome and brain damage, hydrolytic enzymes will leak out into the cytosol and wreak havoc.
The final result of irreversible injury is cell death.