Cerebrovascular Disease Pathology Video
Cerebrovascular Disease
Cerebrovascular disease is a significant source of morbidity and mortality due to cerebrovascular impairment and neurologic dysfunction.
Cerebrovascular disease is typically the result of:
- Ischemia (85% of cases)
- Hemorrhage (15% of cases)
Since serum glucose serves as their primary energy source, neurons are especially vulnerable to ischemia, and may undergo necrosis within 3-5 minutes.
Global Cerebral Ischemia
Global cerebral ischemia is ischemia that effects the entire cerebral tissue.
Important causes of global cerebral ischemia include:
- Minimal perfusion (e.g. atherosclerosis)
- Abrupt reduction in blood flow (e.g. cardiogenic shock)
- Persistent hypoxia (e.g. anemia)
- Hypoglycemia episodes (e.g. insulinoma)
Clinical findings of global cerebral ischemia depend on the length and severity of the trauma.
- Mild global ischemia causes momentary confusion that quickly goes away
- Severe global ischemia causes diffuse necrosis and may result in a vegetative state condition
- Infarcts in watershed regions which may effect memory, sensory, and motor functions
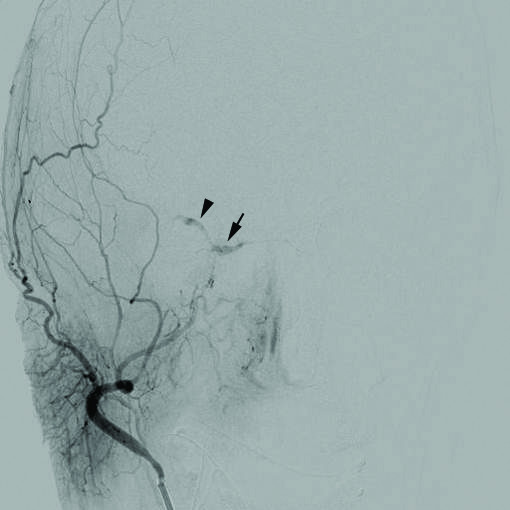
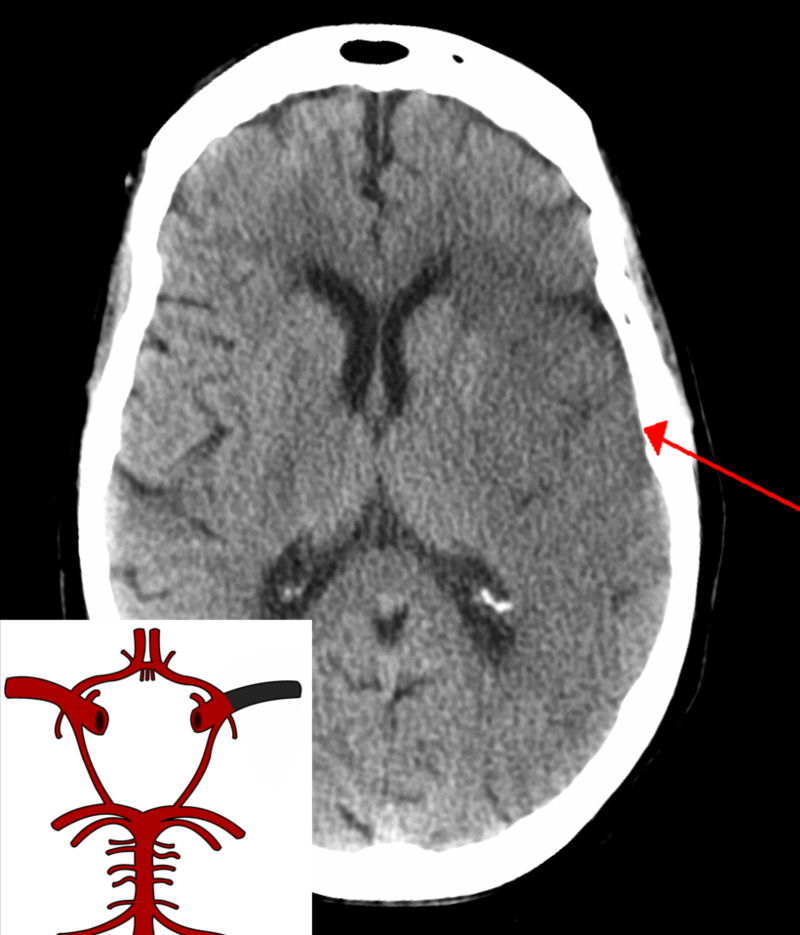
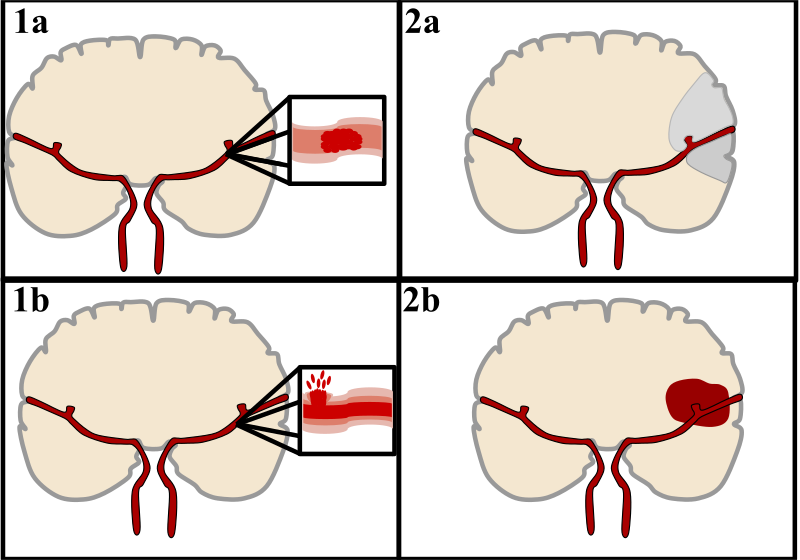
Ischemic Stroke
An ischemic stroke can cause regional ischemia that causes focal neurologic impairments that continue longer than 24 hours.
Transient ischemic attack (TIA) is the name given to an incident if the symptoms last less than 24 hours.
Subtypes of ischemic strokes include:
- Thrombotic (e.g. atherosclerotic plaque rupture)
- Embolic (e.g. from thromboemboli from the heart in atrial fibrillation)
- Lacunar (e.g. from hyaline arteriolosclerosis, an adverse effect of hypertension)
Symptoms of ischemic stroke depend on the region of brain involvement.
- A pure motor stroke results from the interior capsule being involved
- Thalamus causes a pure sensory stroke
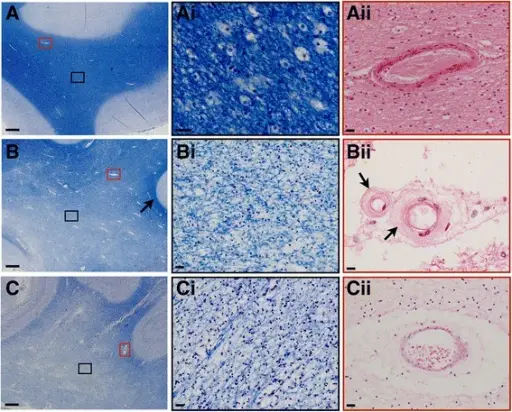
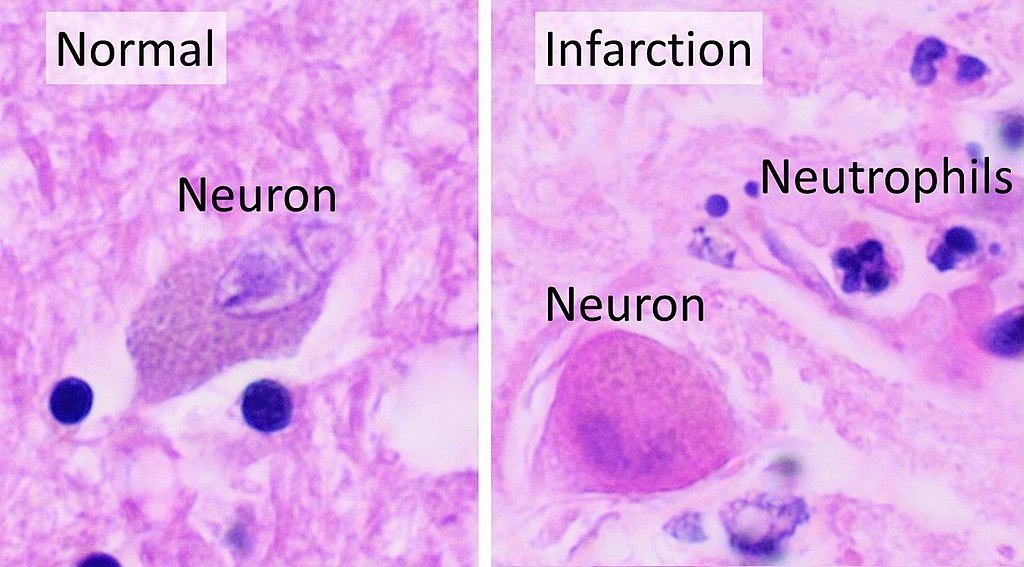
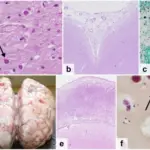
Histologic findings (if obtained) for strokes show:
- An early microscopic observation is an eosinophilic alteration in the cytoplasm of neurons (red neurons) (12 hours after infarction)
- Coagulative necrosis (24 hours)
- Neutrophil infiltration (days 1-3)
- Microglial cell infiltration (days 4-7)
- Granulation tissue (weeks 2-3)
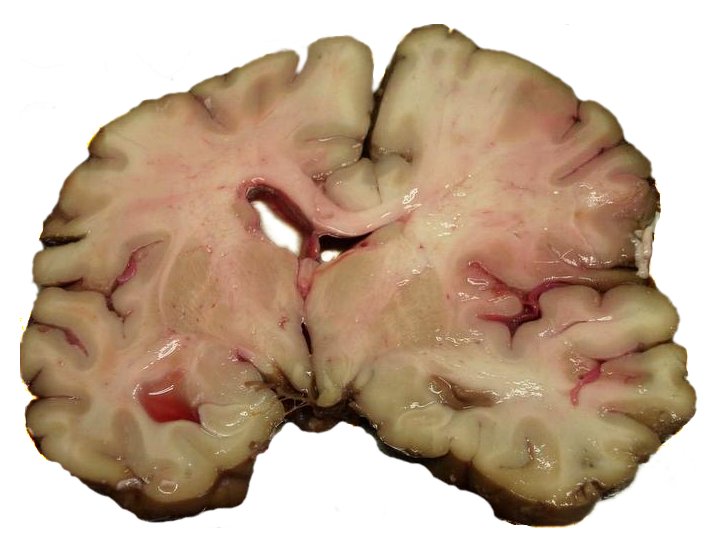
Liquefactive necrosis is the outcome of ischemic stroke.
Liquefactive necrosis results in the development of a cystic area filled with fluid that is encircled by gliosis.
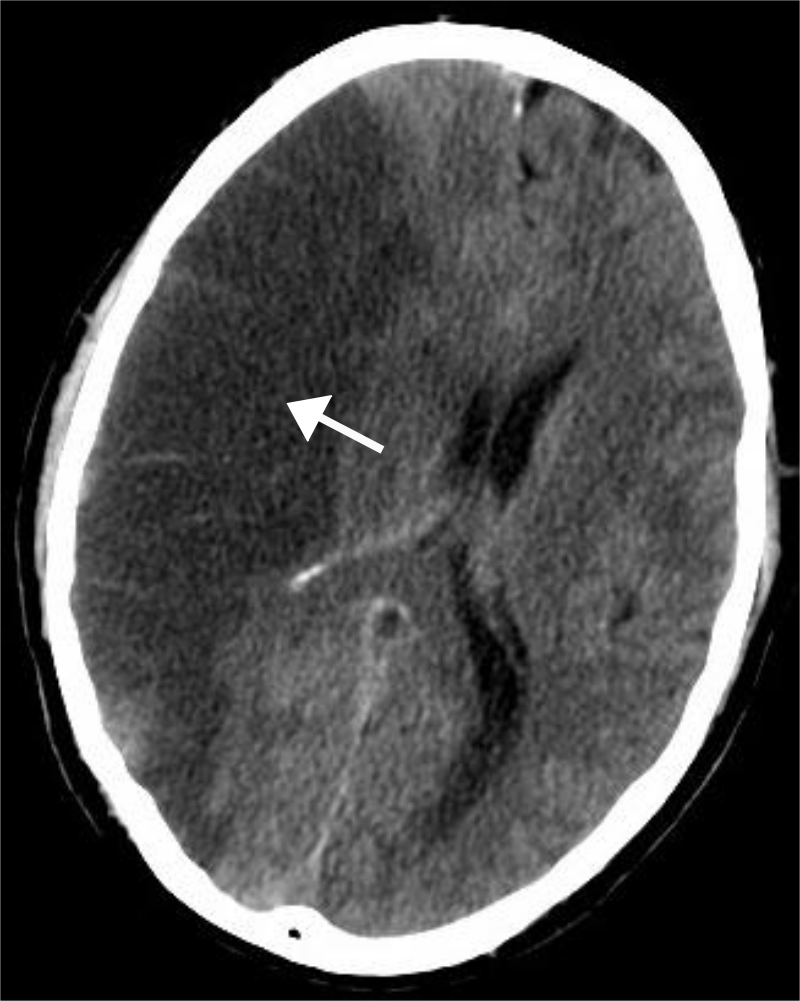
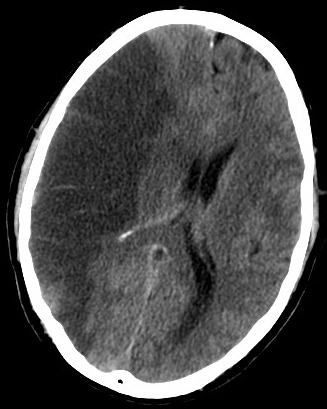
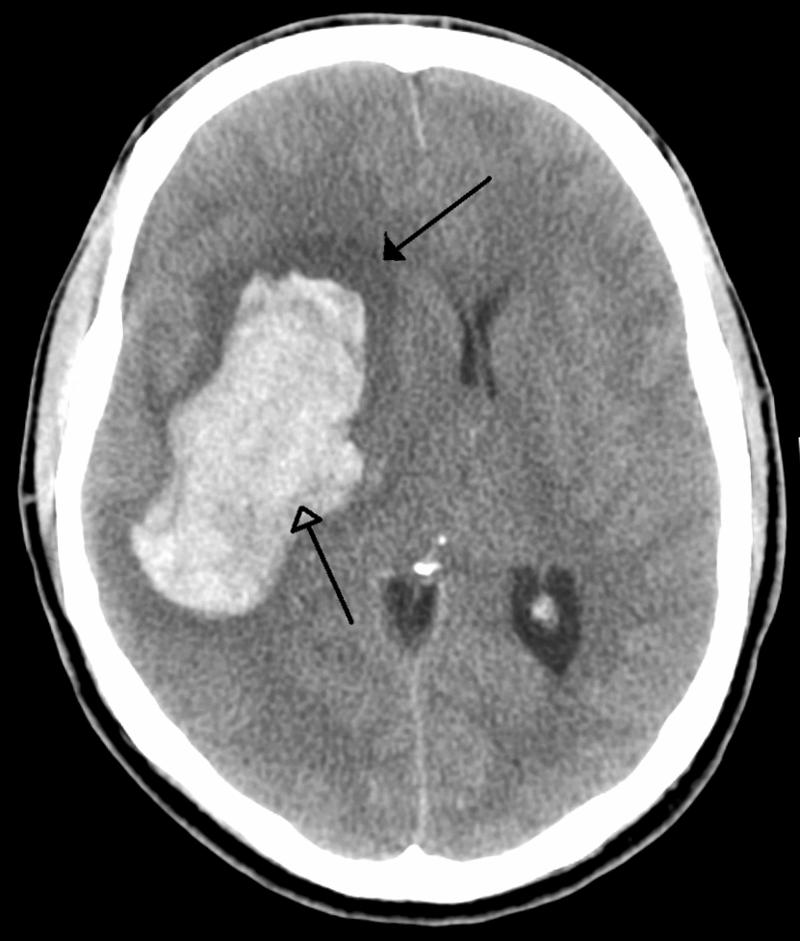
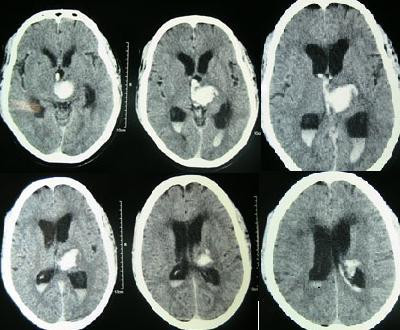
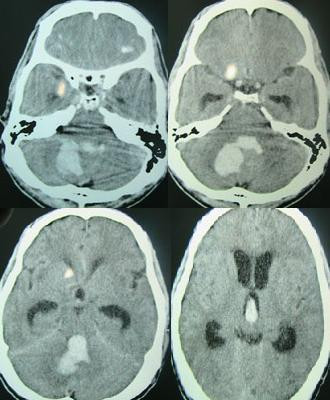
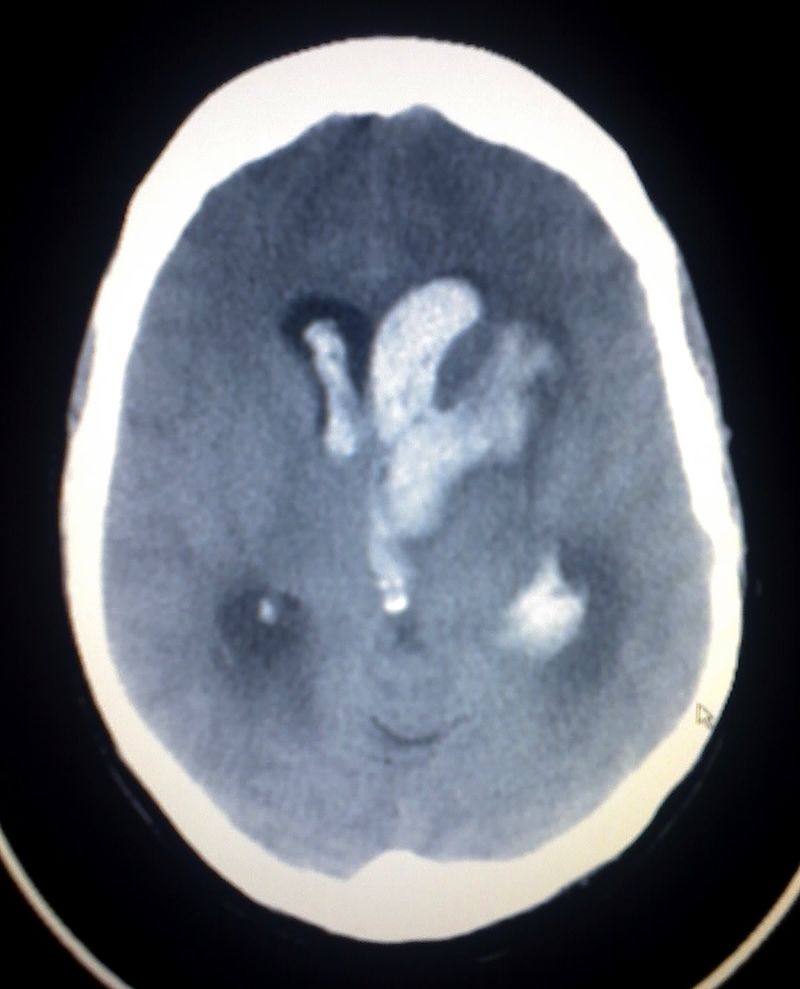
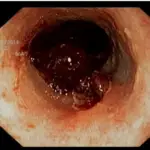
Intracerebral Hemorrhage
An intracerebral hemorrhage is due to brain parenchyma bleeding.
Symptoms of intracerebral hemorrhage include:
- Headache
- Nausea
- Vomiting
- Altered mental status (AMS)
- Coma
Intracerebral hemorrhage may result from:
- Lenticulostriate vessel rupture
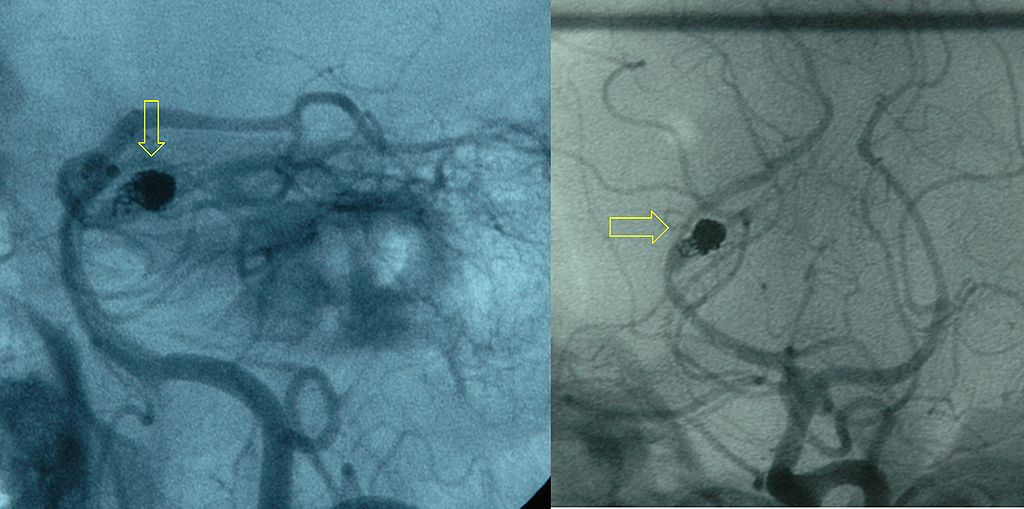
- Aneurysm rupture
The most typical location of the brain involved by intracerebral hemorrhage is the basal ganglia.
Intracerebral hemorrhage hemorrhages may be caused by hypertension.
Hypertension treatment decreases the risk of intracerebral hemorrhage by half.
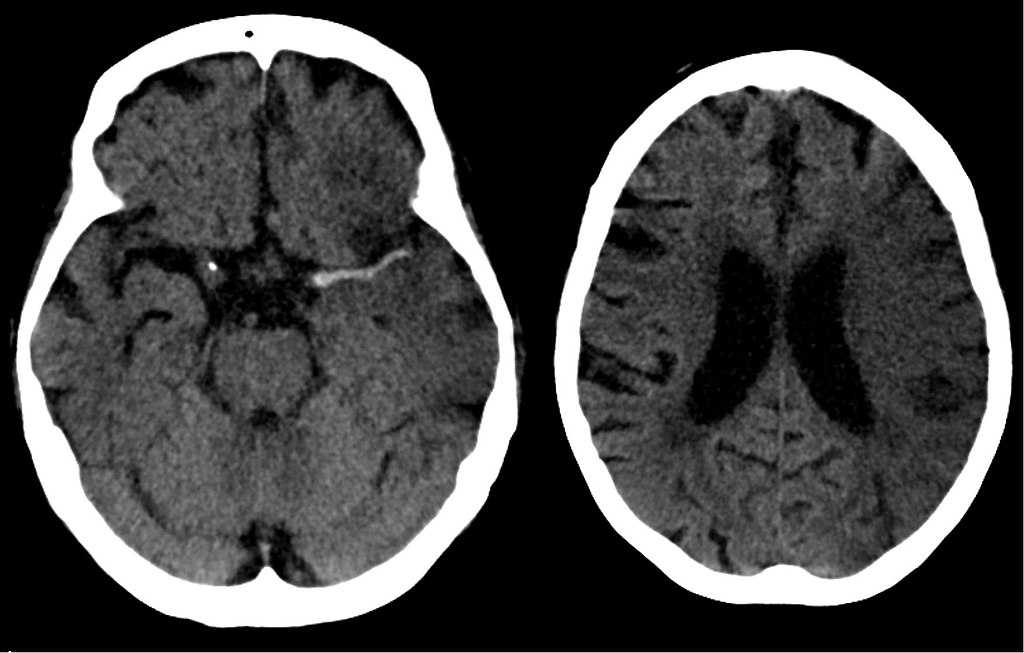
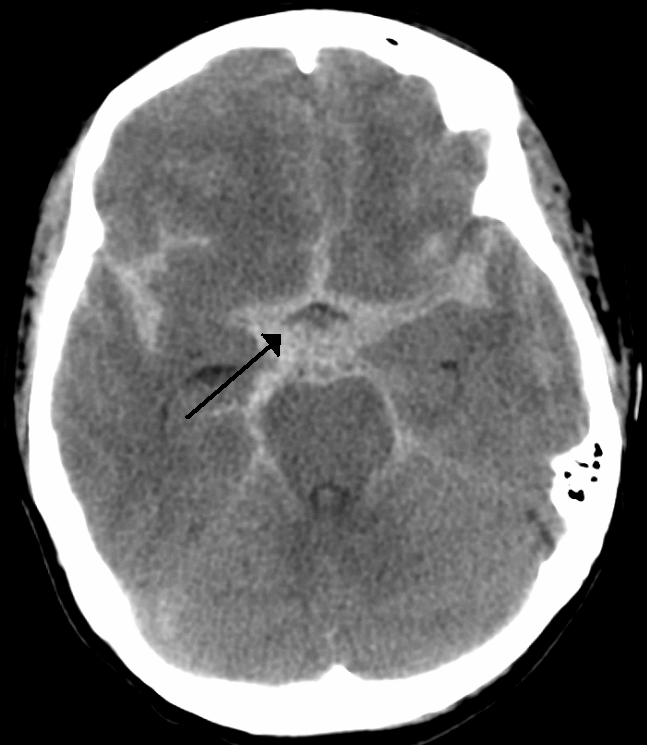
Subarachnoid Hemorrhage
Subarachnoid hemorrhage is hemorrhage that involves the subarachnoid area of the brain.
Subarachnoid hemorrhage symptoms include:
- Sudden “thunder clap” headache
- Worst headache of life
- Suddenly neck stiffness
A spinal tap in a patient with subarachnoid hemorrhage reveals xanthochromia (yellow hue due to bilirubin breakdown).
In subarachnoid hemorrhage, a spinal tap reveals xanthochromia (yellow hue due to bilirubin breakdown).
Causes of subarachnoid hemorrhage include:
- Berry aneurysm rupture (85% of cases)
- Arteriovenous (AV) abnormalities
- Anticoagulation complication