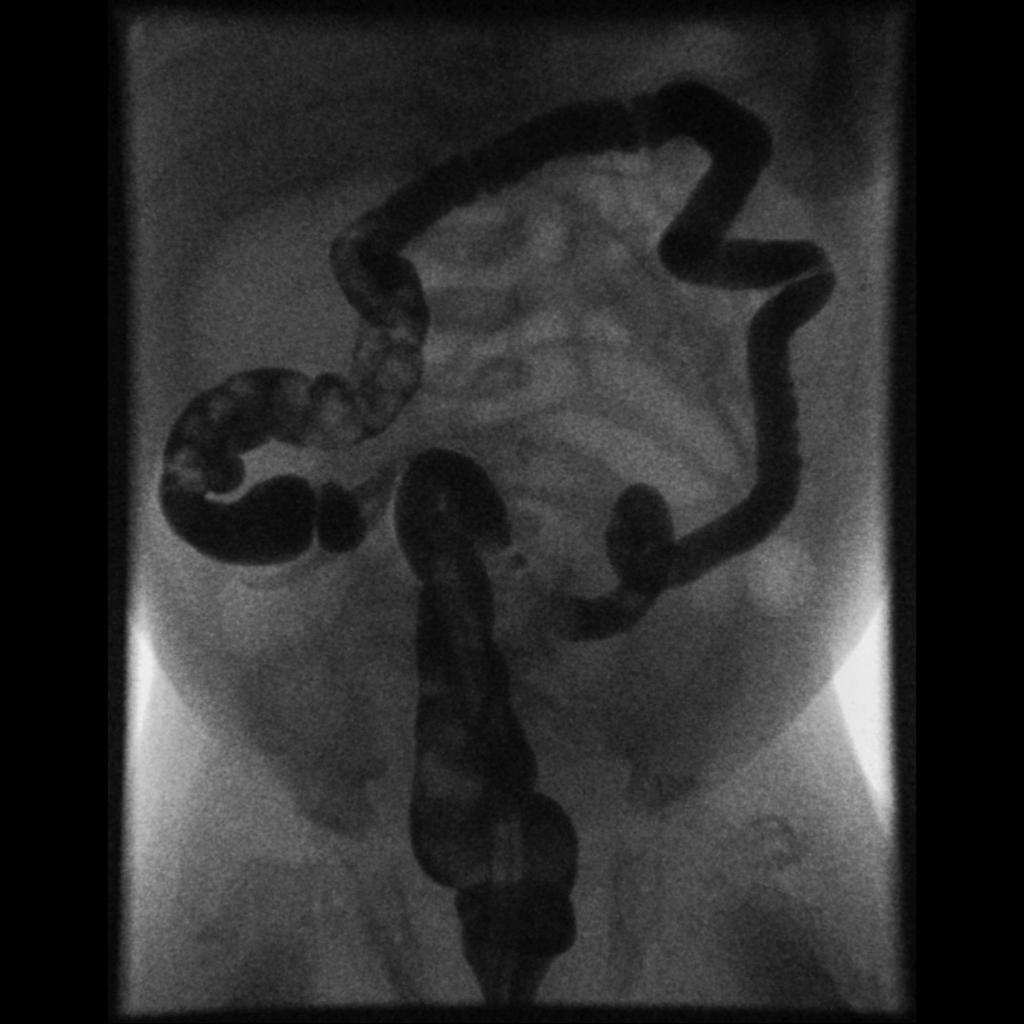
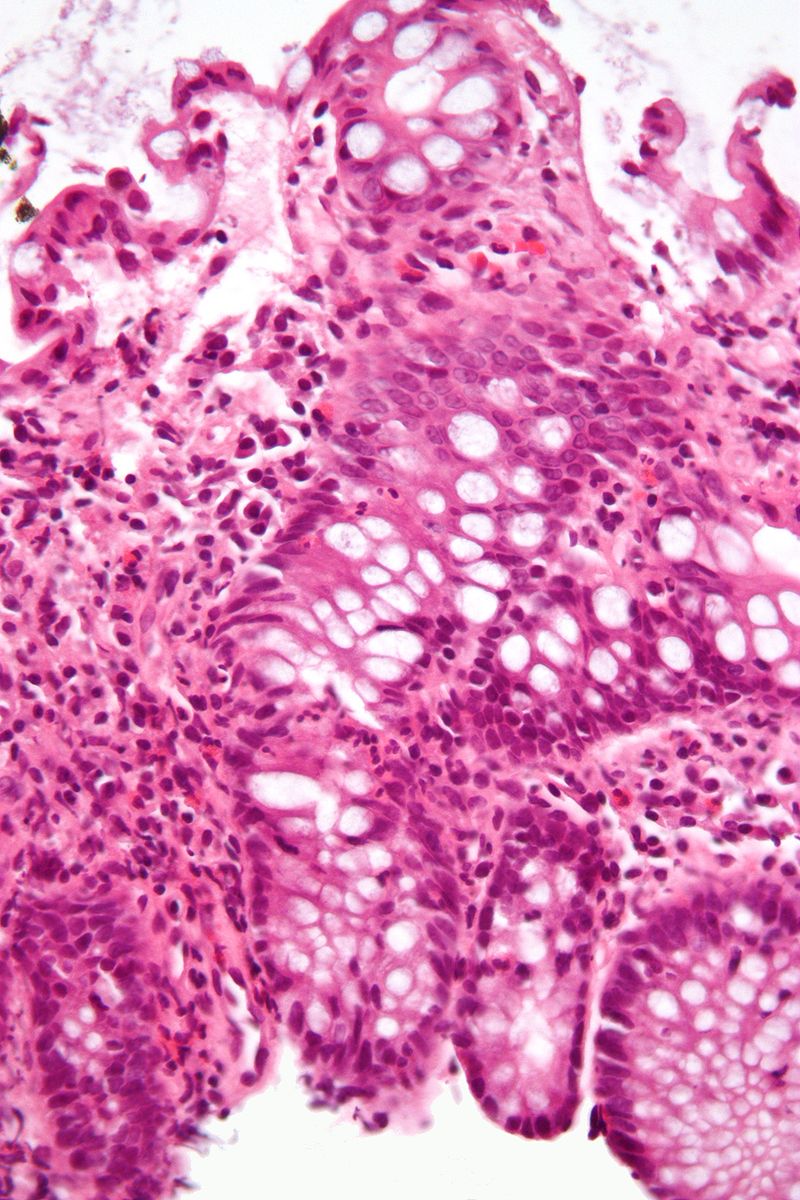
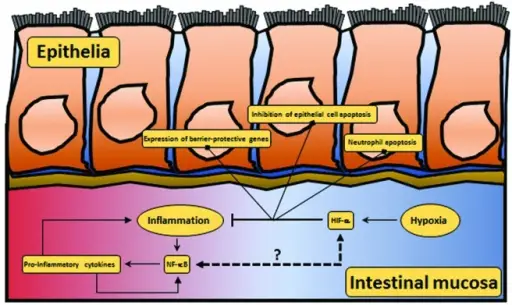
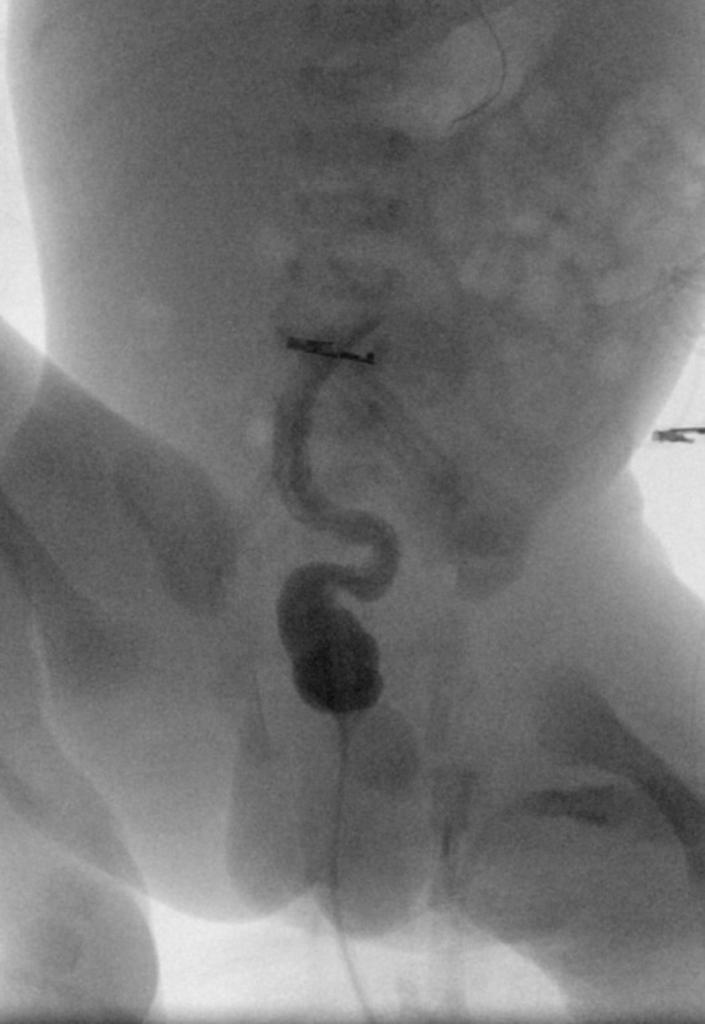
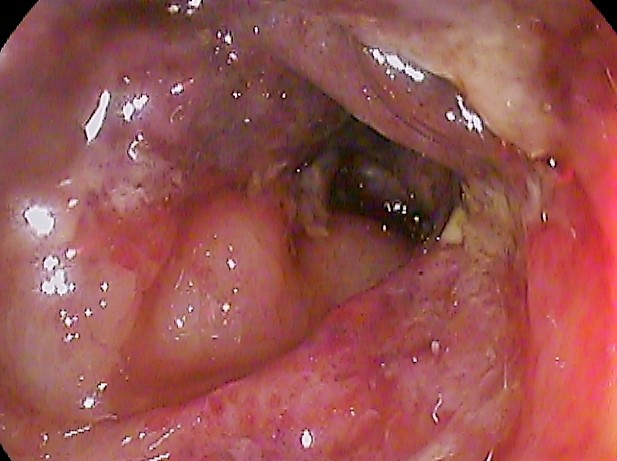
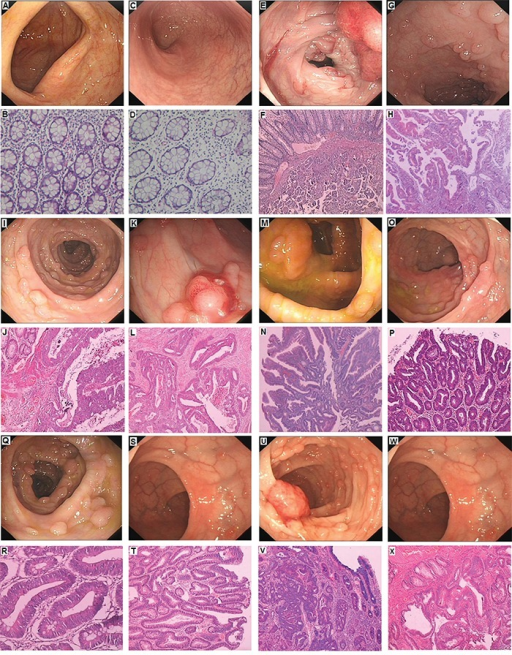
Inflammatory Bowel Disease (IBD)
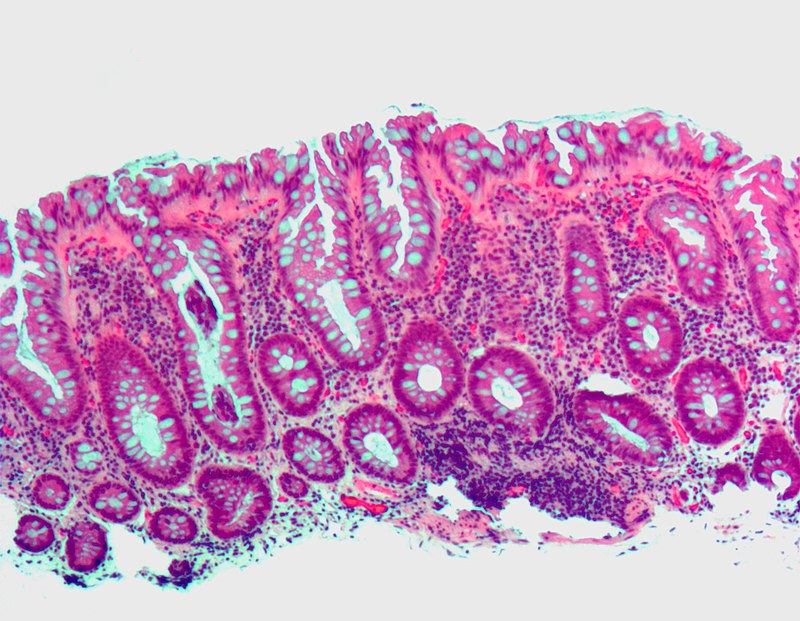
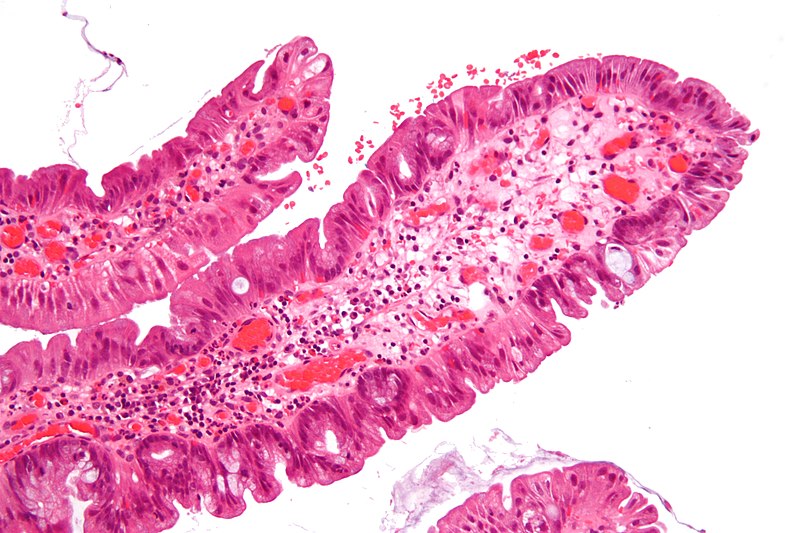
Inflammatory bowel disease (IBD) is chronic, recurrent inflammation of bowel.
Inflammatory bowel disease (IBD) likely as a result of an unusual immunological reaction to intestinal flora.
Inflammatory bowel disease (IBD) usually presents as stomach pain and recurrent episodes of bloody diarrhea are the typical symptoms in young women (teens to 30s).
Inflammatory bowel disease (IBD) is more common in Western societies, especially among Caucasians and Jewish people.
Inflammatory bowel disease (IBD) is sub-classified as Crohn’s disease or ulcerative colitis.
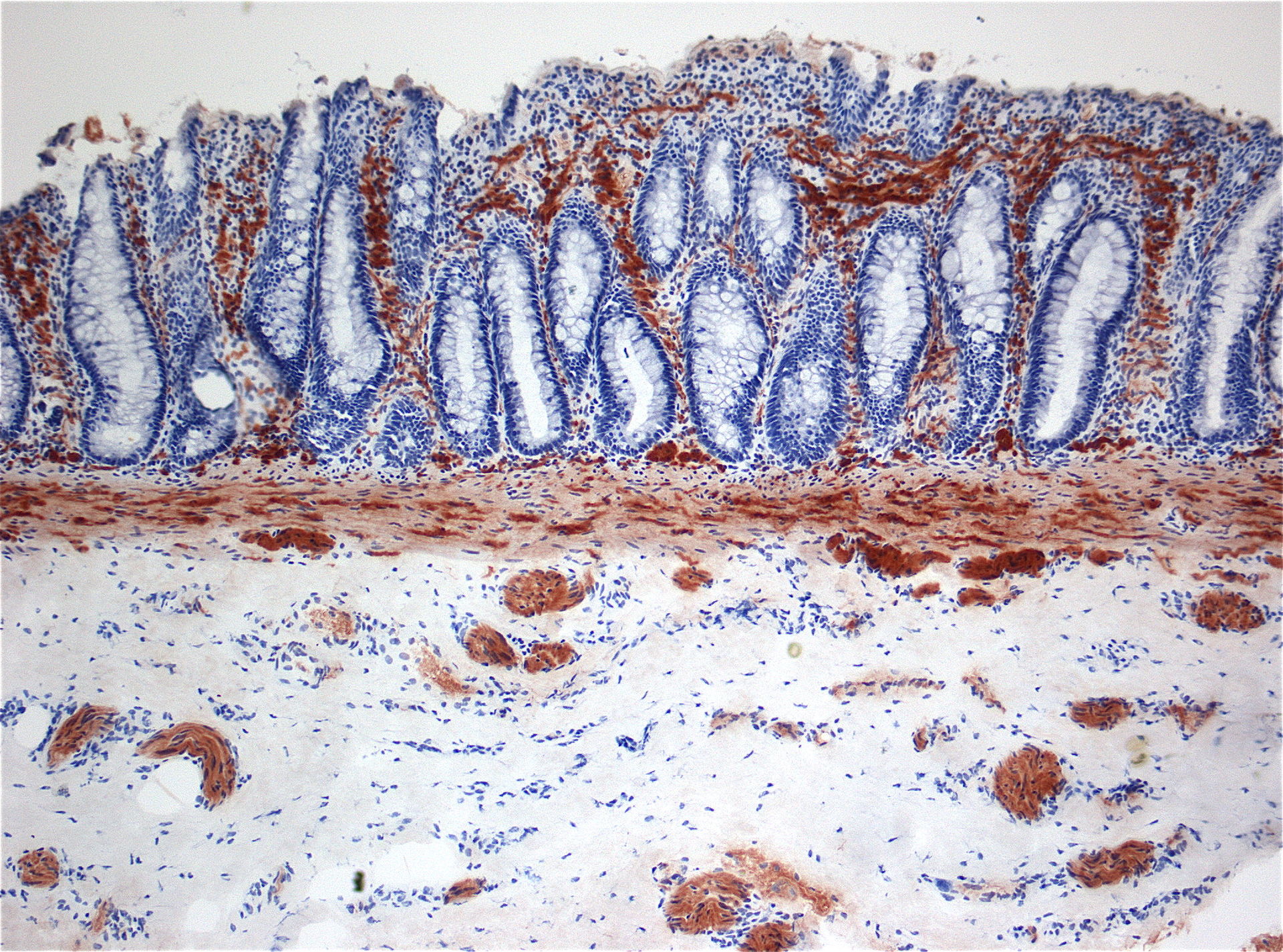
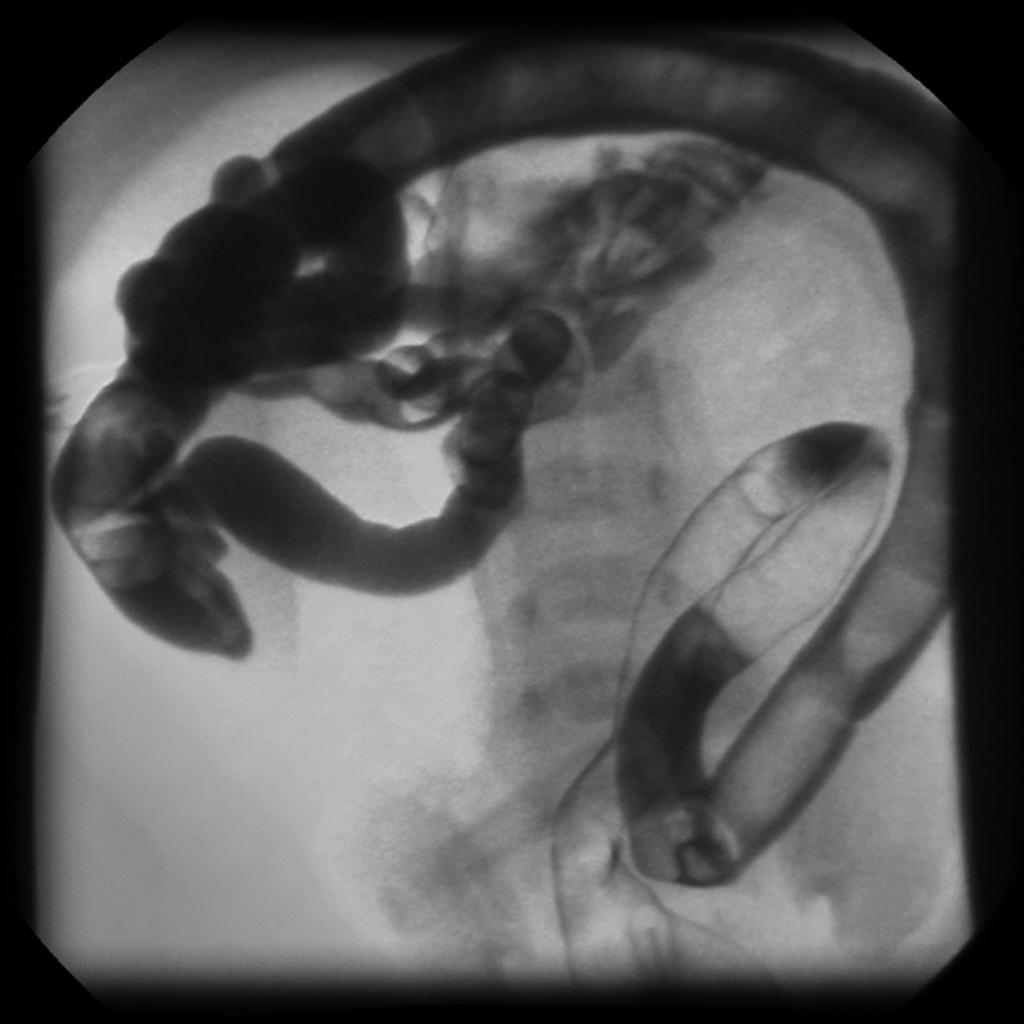
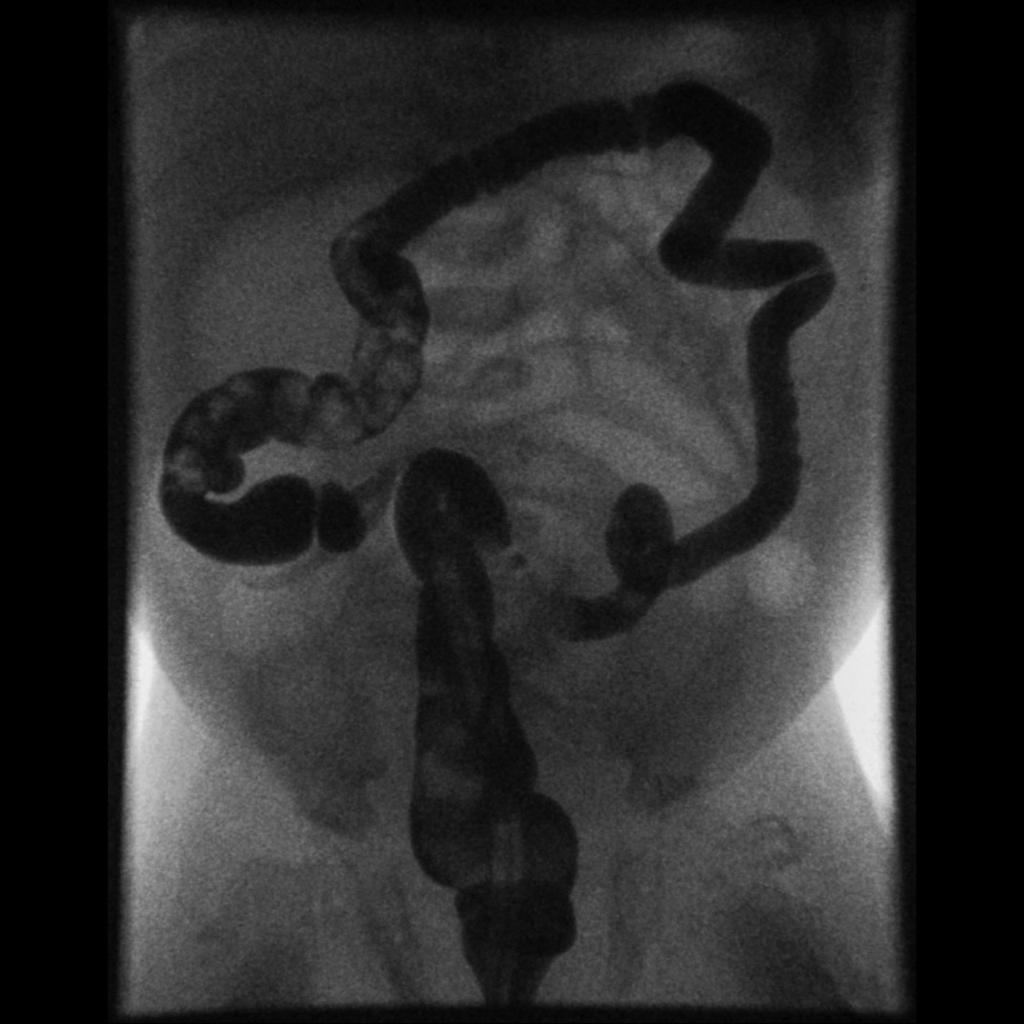
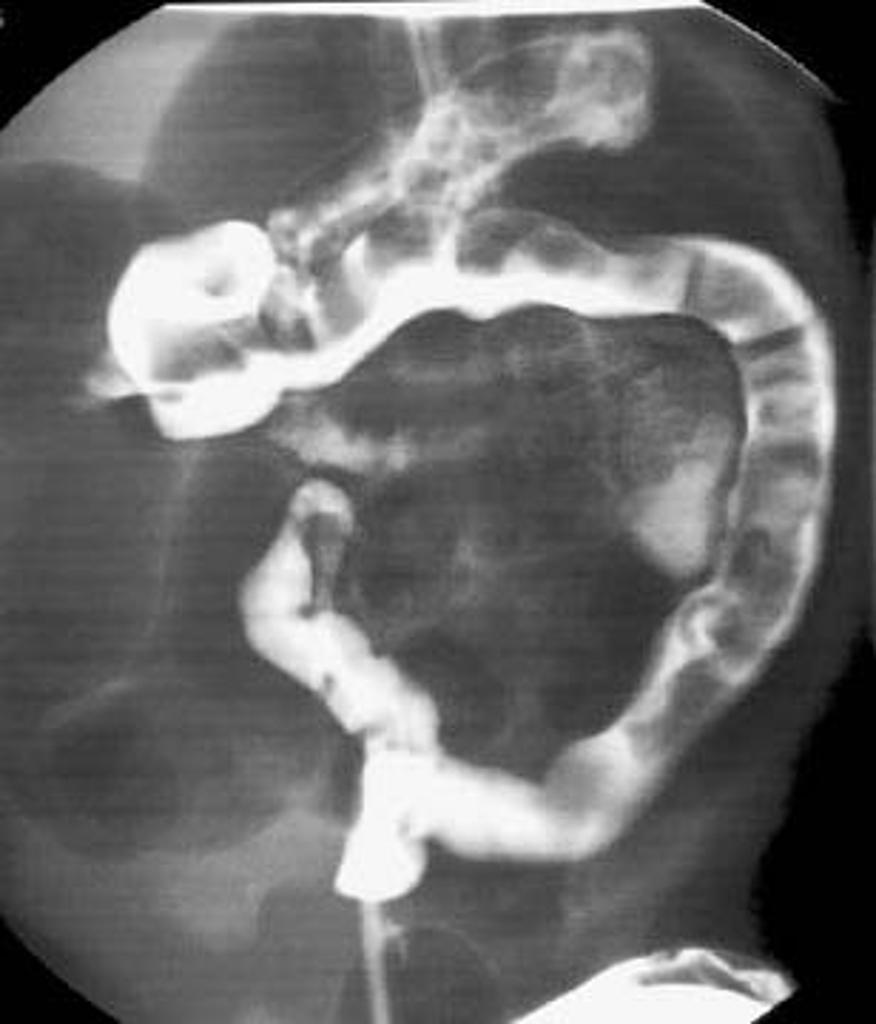
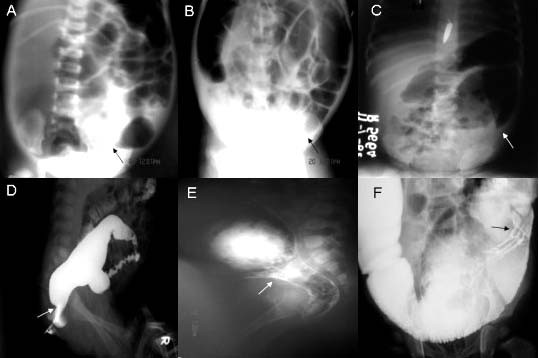
Hirschsprung Disease
Hirschsprung disease results in improper rectus relaxation and distal sigmoid colon peristalsis.
Hirschsprung disease is connected to Down syndrome.
Hirschsprung disease is due to the ganglion cells’ (derived from the neural crest) congenital inability to penetrate the myenteric and submucosal plexus.
Between the inner circular and outer longitudinal muscle layers of the muscularis propria, there is a structure called the myenteric (Auerbach) plexus, which controls motility.
Submucosal (Meissner) plexus controls blood flow, secretions, and absorption from the submucosa.
The clinical characteristics of Hirschsprung disease is based on blockage of the gastrointestinal tract:
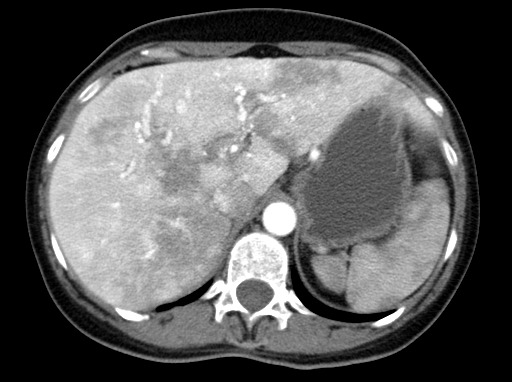
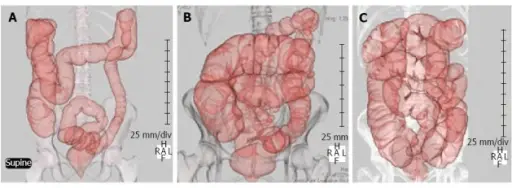
- Massive intestinal dilatation (megacolon) next to a blockage that could rupture
- Meconium not passing
- Rectal vault empty during a digital rectal exam
Hirschsprung disease concern requires a rectal suction biopsy.
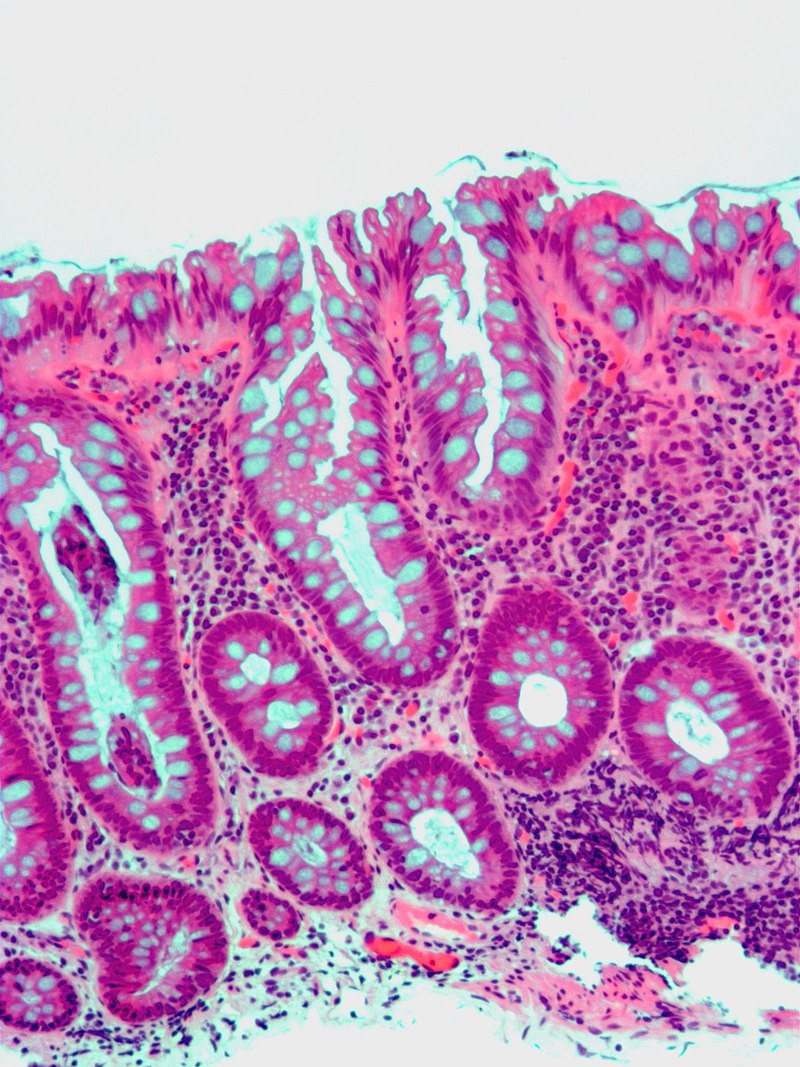
Histology of Hirschsprung disease shows lack of ganglion cells.
Treatment of Hirschsprung disease requires the affected bowel be removed.
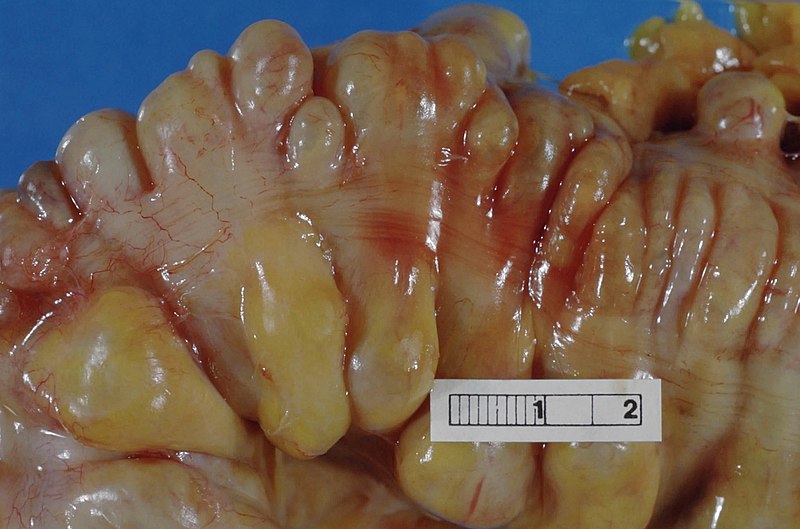
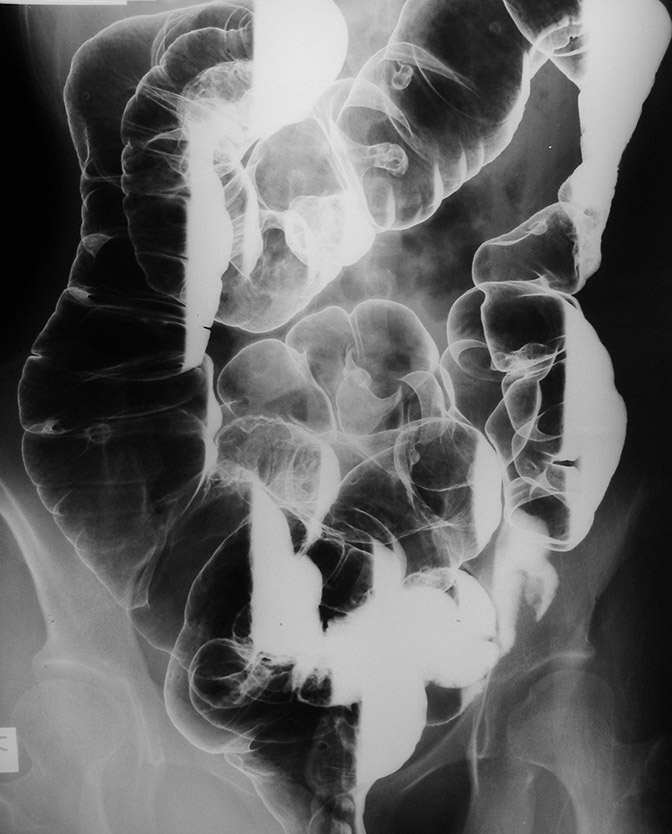
Colonic Diverticula
Colonic diverticula are mucosal and submucosal outpouching through the muscularis propria (false diverticulum).
Colonic diverticula are associated with colonic wall stress.
Risk factors of colonic diverticula include:
- Constipation
- Straining with bowel movements
- Low-fiber diet
- Older age
Colonic diverticula most often effects the sigmoid colon is the most typical place.
Colonic diverticula usually develop where the vasa recta crosses the muscularis propria (weak area in the intestinal wall).
Colonic diverticula are usually asymptomatic.
Complications of colonic diverticula include:
- Rectal bleeding (hematochezia)
- Diverticulitis (caused by obstruction from feces) that has symptoms resembling appendicitis in the left lower quadrant
- Diverticulum with a fistula inflamed ruptures and adheres to a nearby structure
- Colovesicular fistula
Urine with air (or stool) in it is a sign of a colovesicular fistula.
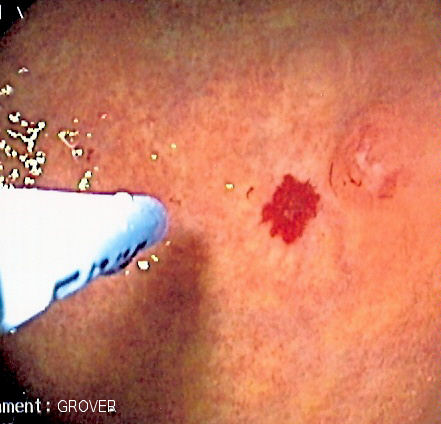
Angiodysplasia
Angiodysplasia is mucosal and submucosal capillary beds anomaly.
Angiodysplasia typically develops in the right colon and cecum as a result of strong wall strain.
Hematochezia is a typical sign of angiodysplasia rupture in an older adult.
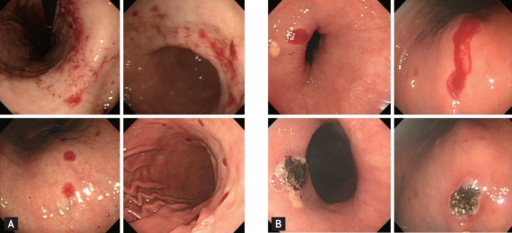
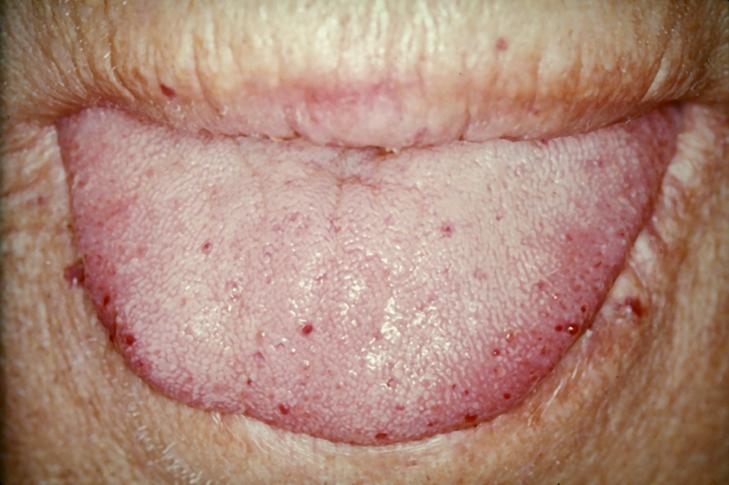
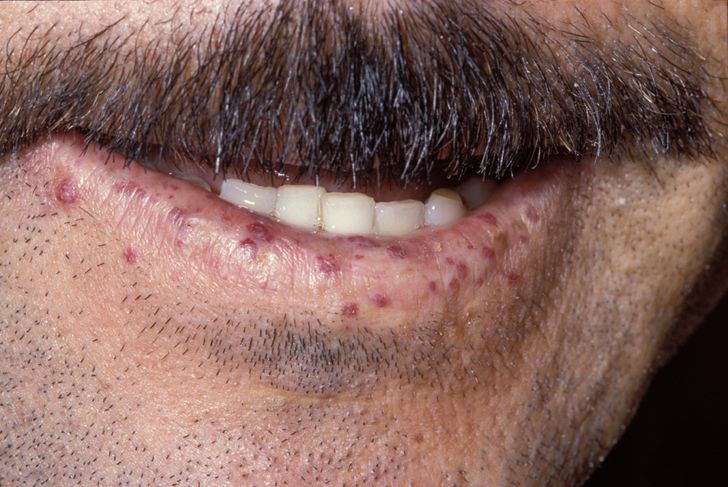
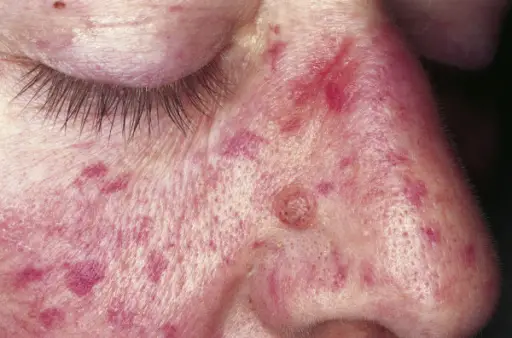
Hereditary Hemorrhagic Telangiectasia
Hereditary hemorrhagic telangiectasia is a thin-walled blood vessels as a result of an autosomal dominant disease are particularly prevalent in the mouth and gastrointestinal tract.
Ischemic Colitis
Ischemic colitis is inflammation of the colon due to ischemia.
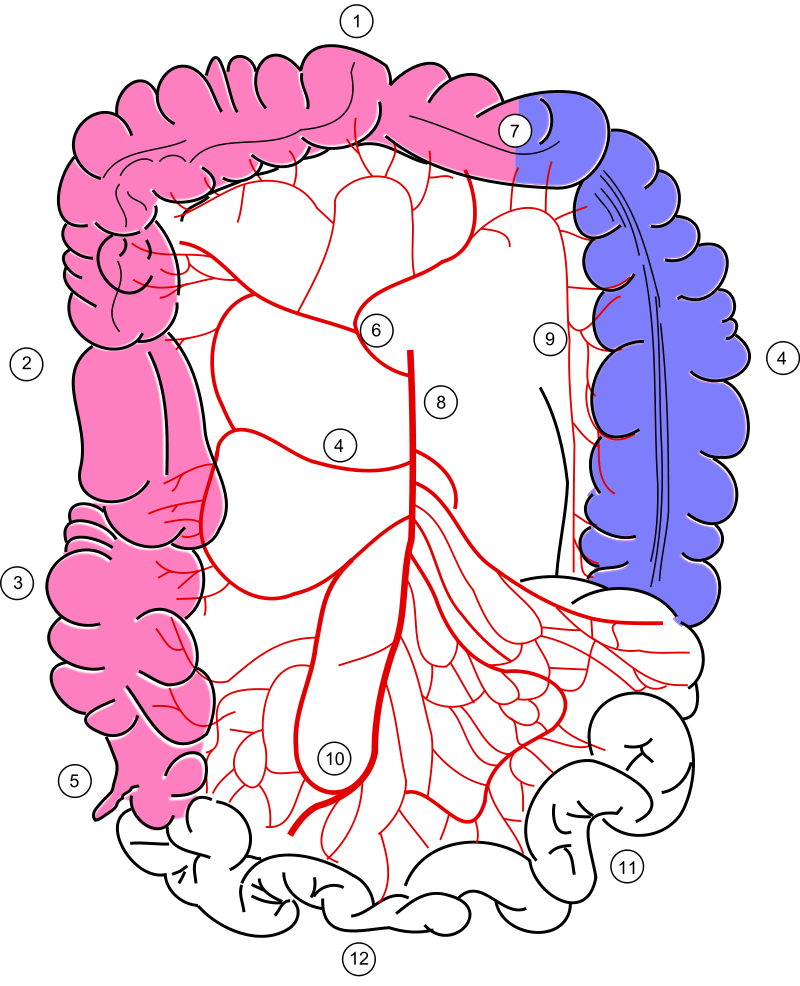
Ischemic colitis is more apt to happen near the splenic flexure (watershed area of superior mesenteric artery (SMA)).
The most frequent cause of ischemic colitis is superior mesenteric artery (SMA) atherosclerosis.
Ischemic colitis symptoms include:
- Postprandial pain
- Weight loss
- Pain
- Bloody diarrhea
Irritable Bowel Syndrome (IBS)
Irritable bowel syndrome (IBS) symptoms include:
- Recurrent stomach pain
- Bloating
- Flatulence
- Diarrhea
- Constipation
Irritable bowel syndrome (IBS) is typically experienced by middle-aged women.
Irritable bowel syndrome (IBS) is typically connected to abnormal intestinal motility.
No obvious pathogenic alterations are noted in irritable bowel syndrome (IBS).
Dietary fiber intake may help symptoms irritable bowel syndrome (IBS).
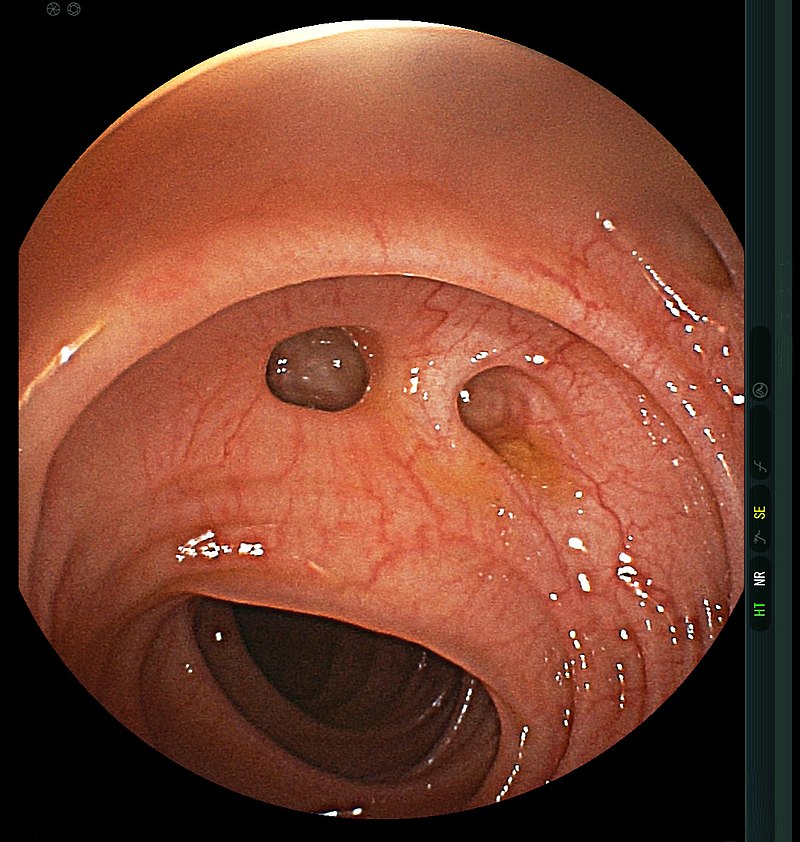
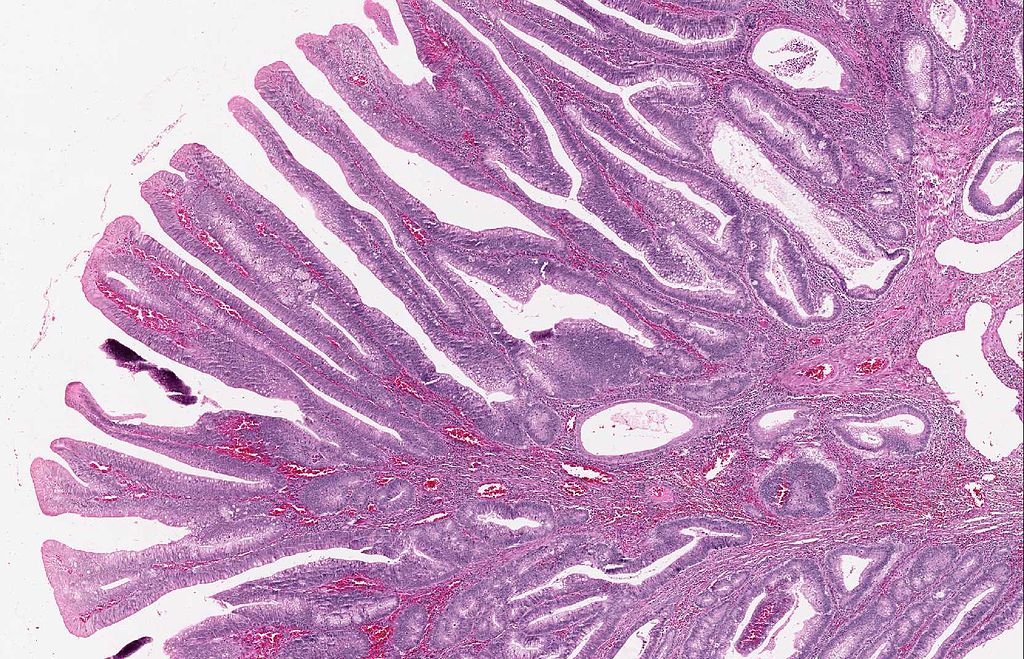
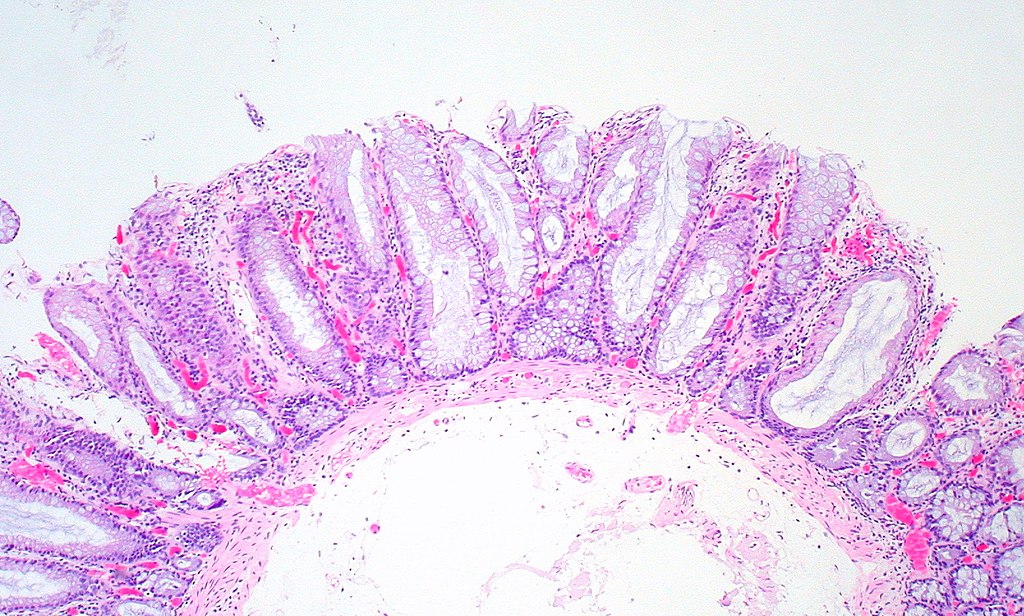
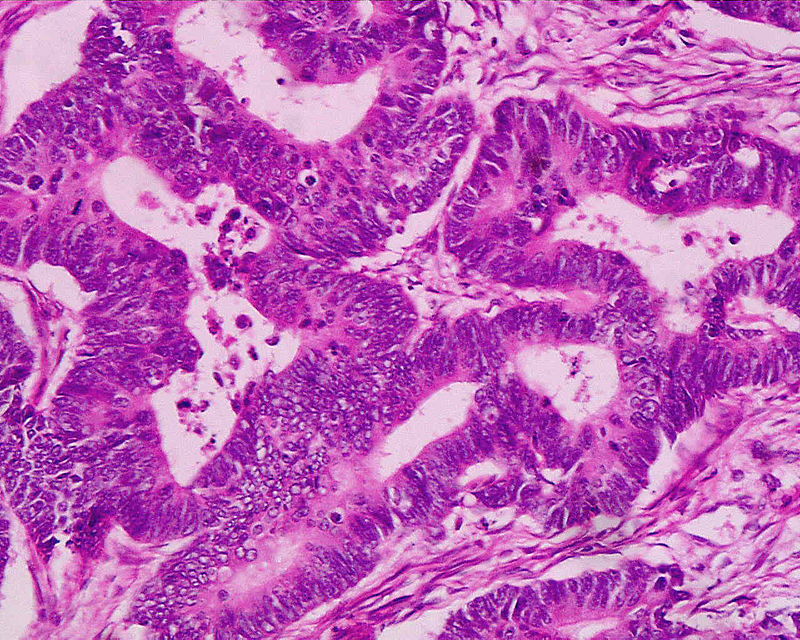
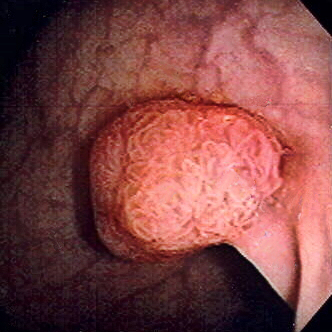
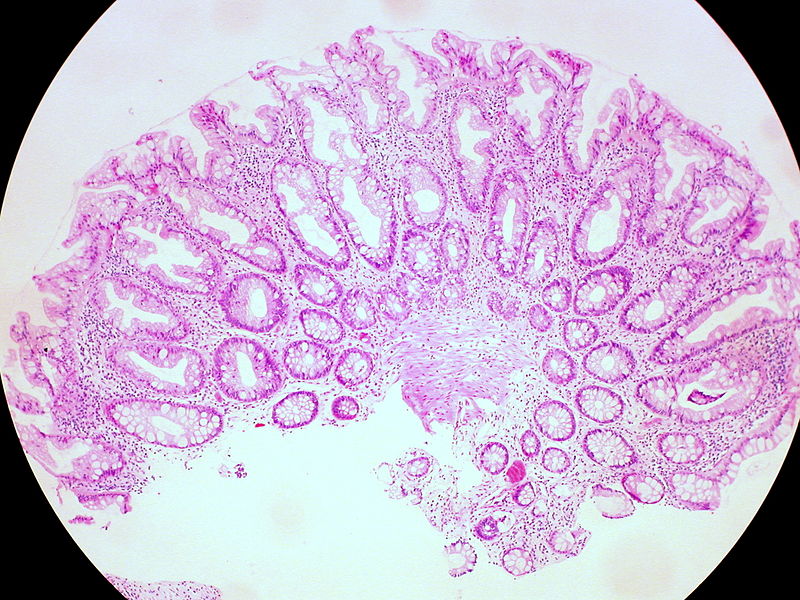
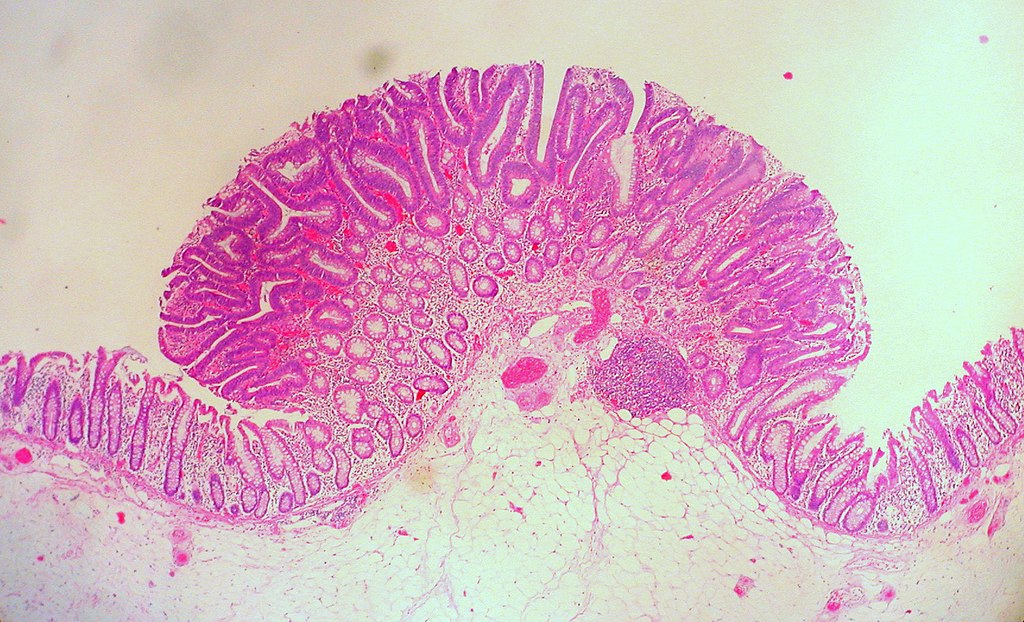
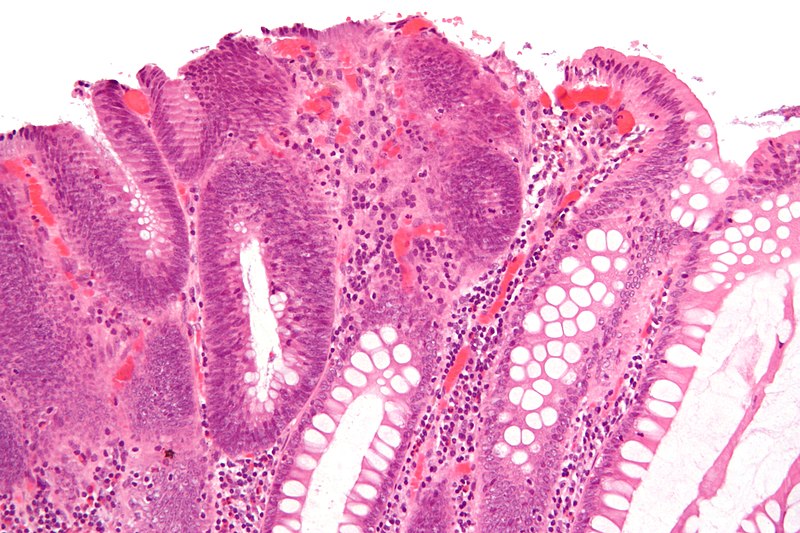
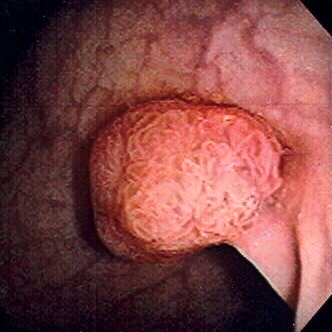
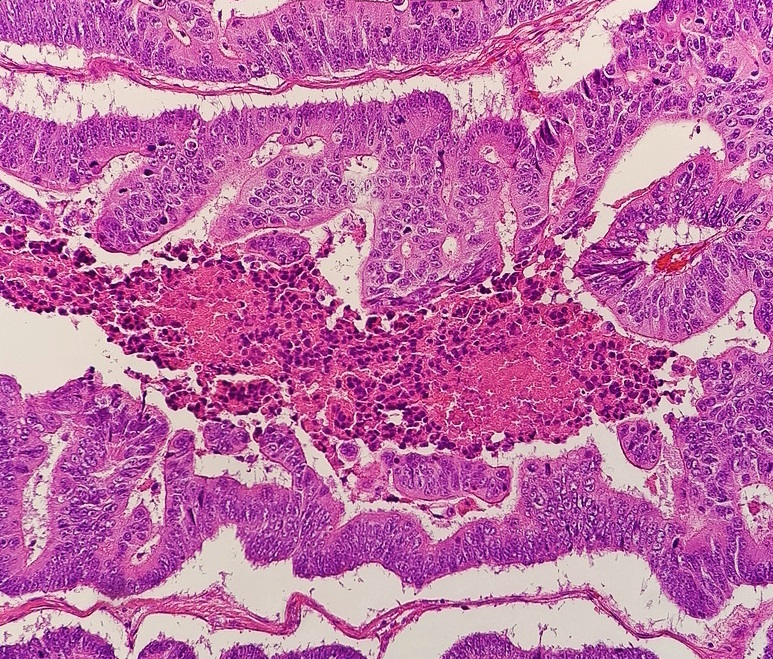
Colonic Polyps
Colonic polyps are colonic mucosal protrusions that are raised.
Adenomatous and hyperplastic polyps are the most prevalent forms of colonic polyps.
The overgrowth of glands results in hyperplastic polyps.
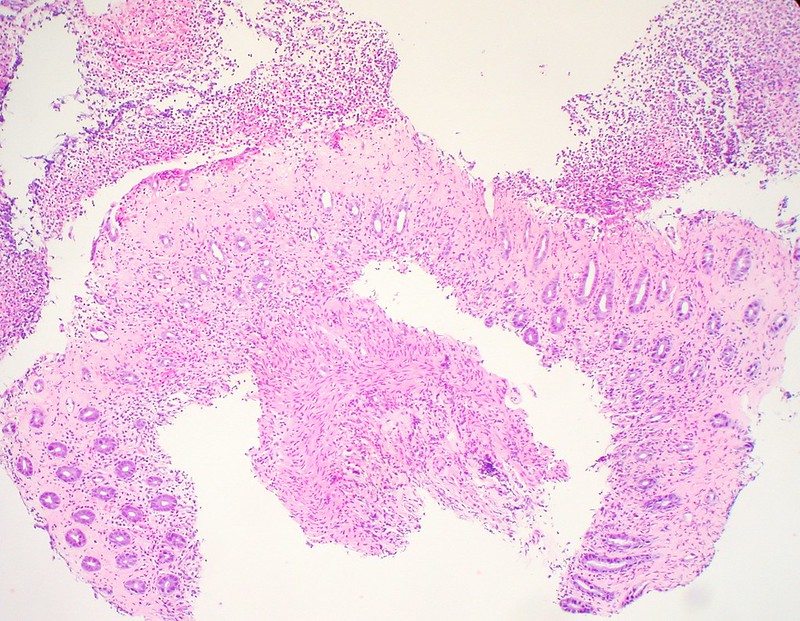
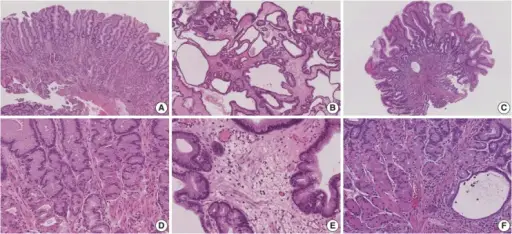
Histologically, colonic polyps typically appear as:
- Polypoid
- Hyperplastic
- Sessile serrated
- Tubular
- Villous
- Tubulovillous
Polyps may proceed through the adenoma-carcinoma sequence to adenocarcinoma.
Benign incapable of becoming cancerous.
Neoplastic gland proliferation results in adenomatous polyps.
Adenomatous polyps are the second most typical kind of colonic polyp.
Adenomatous polyps are benign but premalignant.
Adenomatous polyps may proceed through the adenoma-carcinoma sequence to adenocarcinoma.
The molecular transition from healthy colonic mucosa to adenomatous polyp to carcinoma is described by the term “adenoma-carcinoma sequence”.
Adenomatous polyposis coli (APC) gene alterations, whether sporadic or germline, enhance the chance of polyp development.
Polyp development is caused by the APC gene mutation.
Aspirin may prevent progression from adenoma to carcinoma.
P53 mutation and increased cyclooxygenase (COX) expression allow for carcinoma to develop.
Colonoscopy and tests for fecal occult blood are used to check for polyps.
Polyps are typically clinically quiet but can bleed.
Prior to adenomatous polyps developing into cancer, removal is the goal.
Adenomatous and hyperplastic polyps have the same appearance during a colonoscopy.
As a result, all polyps are removed and analyzed under a microscope.
The biggest risk factors for turning an adenoma into a carcinoma include:
- Polyp size > 2.0 cm
- Growth rate
- Villous histology
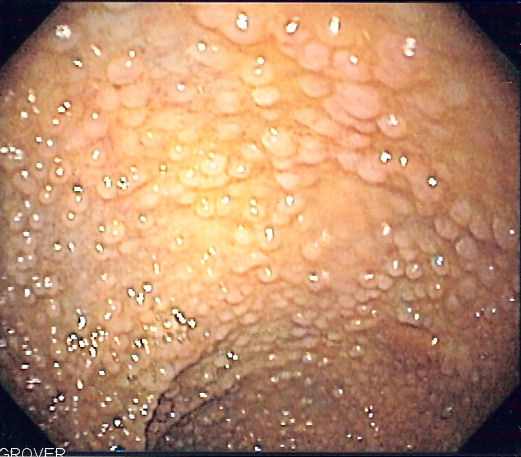
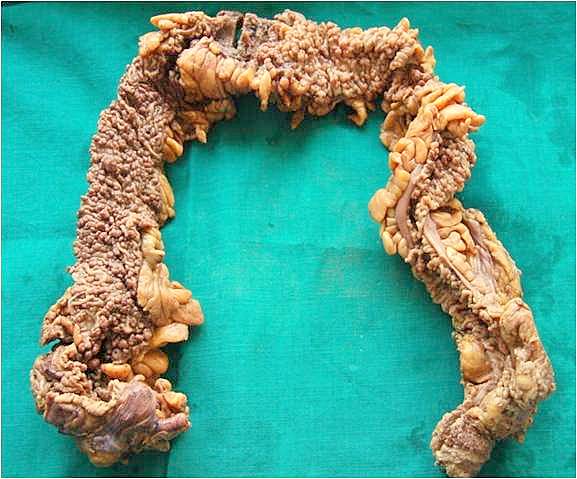
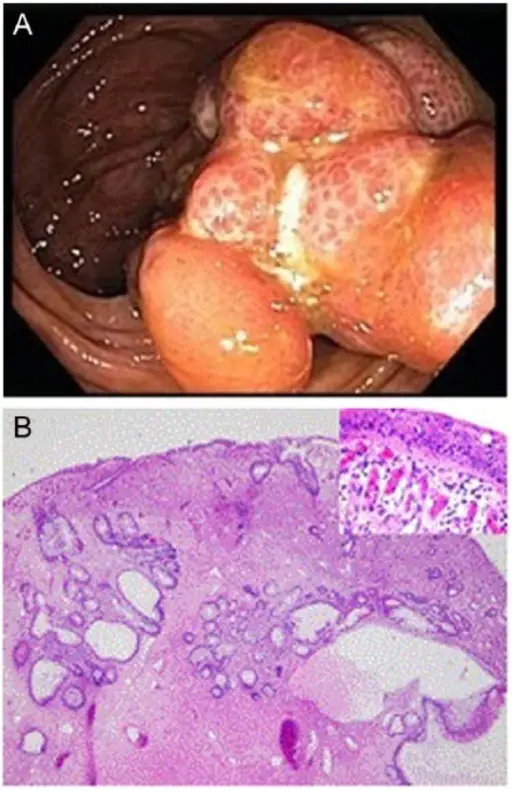
Familial Adenomatous Polyposis (FAP)
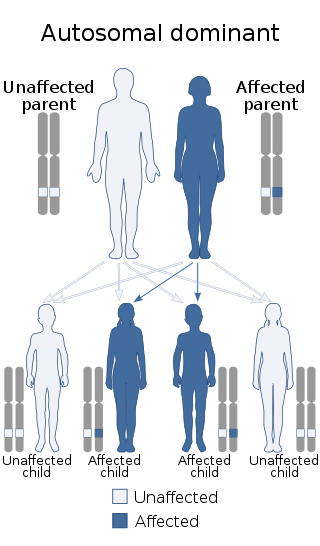
Numerous adenomatous colonic polyps characterize this autosomal dominant disease.
Familial adenomatous polyposis (FAP) occurs due to a hereditary APC gene mutation (on chromosome 5).
APC gene mutation increases the likelihood that adenomatous polyps may form in the colon and rectum.
Familial adenomatous polyposis (FAP) patients may require prophylactic colon and rectum removal.
Almost all patients with familial adenomatous polyposis (FAP) will acquire cancer by the age of 40-years-old.
A non-neoplastic proliferation of fibroblasts is known as fibromatosis.
Develops in the desmoid of the retroperitoneum and kills tissue there.
An osteoma is a benign bone tumor that typically develops in the skull.
Familial adenomatous polyposis (FAP) with fibromatosis and osteomas is Gardner syndrome.
Familial adenomatous polyposis (FAP) with central nervous system (CNS) malignancies is the Turcot syndrome (medulloblastoma and glial tumors).
Juvenile Polyp
Juvenile polyp is a sporadic, benign (hamartomatous) polyp that appears in young children (under 5 years old).
Juvenile polyp commonly manifests as a single rectal polyp that prolapses and bleeds.
Multiple juvenile polyps in the colon and stomach are a defining feature of juvenile polyposis.
The likelihood that juvenile polyps may develop into cancer is increased by their abundance.
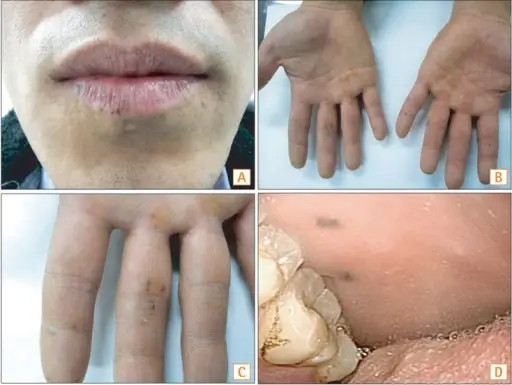
Peutz-Jeghers Syndrome
Peutz-Jeghers syndrome is characterized by:
- Hamartomatous (benign) polyps
- Freckle-like lesions on mucosal surfaces (lips, oral mucosa, vaginal skin)
Peutz-Jeghers syndrome is autosomal dominance.
There is an elevated risk of gynecologic, breast, and colorectal cancer in Peutz-Jeghers syndrome.
Colorectal Carcinoma
Colorectal carcinoma is cancer that develops in the rectal or colon mucosa.
Colorectal carcinoma is the third most frequent place for cancer and third most frequent reason for cancer-related fatalities.
Incidence of colorectal carcinoma peaks between the ages of 60 and 70-years-old.
Colorectal carcinoma most frequently results from the adenoma-carcinoma sequence; microsatellite instability is a second significant molecular route (MSI).
Microsatellites are non-coding DNA repeating sequences whose stability is preserved throughout cell division.
Instability suggests flawed DNA copying processes (e.g. DNA mismatch repair enzymes).
Hereditary mutations in DNA mismatch repair enzymes are the cause of hereditary nonpolyposis colorectal cancer (HNPCC).
In hereditary nonpolyposis colorectal cancer (HNPCC) there is increased risk of ovarian, endometrial, and colorectal cancer.
At a relatively young age, colorectal cancer develops spontaneously (not from adenomatous polyps), and is typically right-sided.
At age 50-years-old, fecal occult blood tests and endoscopy are used for colorectal cancer screening.
The objective is early cancer detection and removal of adenomatous polyps before carcinoma develops (before clinical symptoms arise).
Colorectal carcinoma can occur anywhere along the colon’s length.
Symptoms of left sided colorectal carcinoma include:
- Left-sided carcinoma
- Decreased stool volume
- Pain in the left lower quadrant
- Blood-streaked stool
- Napkin-ring lesion
Symptoms of right side colorectal carcinoma include:
- Iron-deficiency anemia (occult bleeding)
- Abdominal discomfort
Until proven differently, an older adult with iron deficiency anemia has colon cancer.
Streptococcus bovis endocarditis risk is increased in colorectal carcinoma.
Staging describes how far the lesion has gone.
- T for the depth of invasion
- N for the lymph nodes that the cancer has migrated to
- M for metastasis (where the tumor has moved to)
Due to the absence of lymphatics in the mucosa, tumors that are restricted to the mucosa typically do not disseminate.
Metastatic colon cancer commonly involves:
- Liver
- Lungs
A serum tumor marker called carcinoembryonic antigen (CEA) is helpful for evaluating treatment efficacy and spotting recurrence of colorectal carcinoma.
Carcinoembryonic antigen (CEA) is not useful for colorectal carcinoma screening.