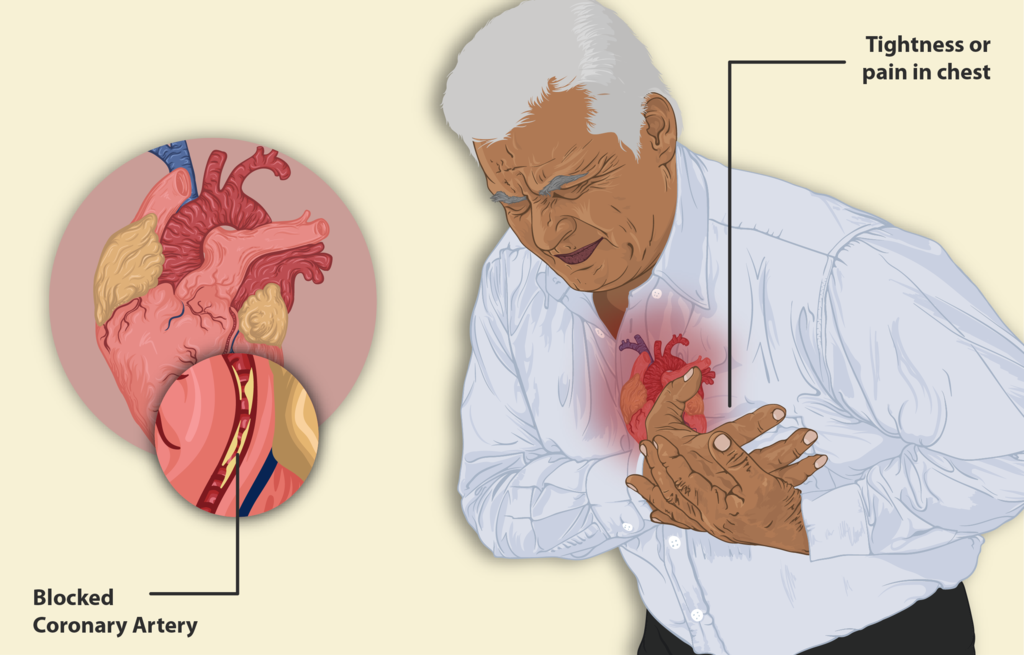
Ischemic Heart Disease
Ischemic Heart Disease Pathology Video
Ischemic heart disease is a group of syndromes associated with myocardial ischemia.
Ischemic heart disease is the major cause of death in the United States of America (USA).
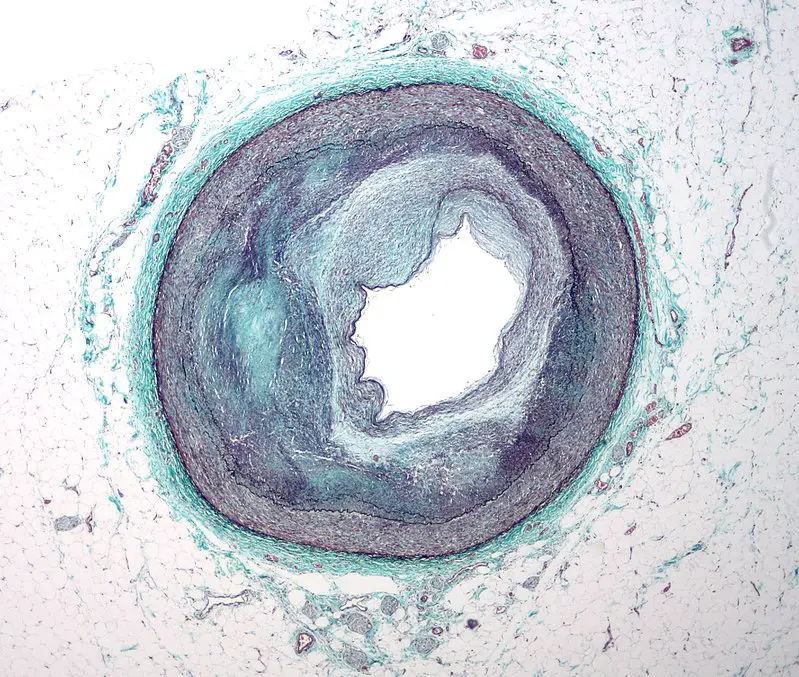
Ischemic heart disease is typically brought on by coronary artery atherosclerosis, which reduces blood flow to the myocardium.
Risk factors for ischemic heart disease include:
- Diet
- Cholesterol
- Smoking
- Age
Stable Angina
As a result of physical activity or emotional stress, chest pain may occur due to stable angina.
Stable angina is usually the result of atherosclerosis of coronary arteries with less than 70 percent stenosis.
In stable angina, reduced blood flow is not able to meet the metabolic demands of the myocardium during cardiac exertion.
Stable angina represents damage that myocytes can recover from (no necrosis).
Symptoms of stable angina include:
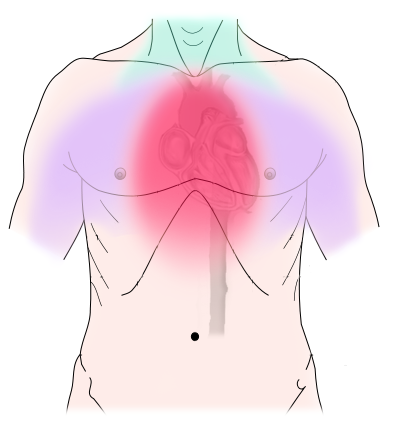
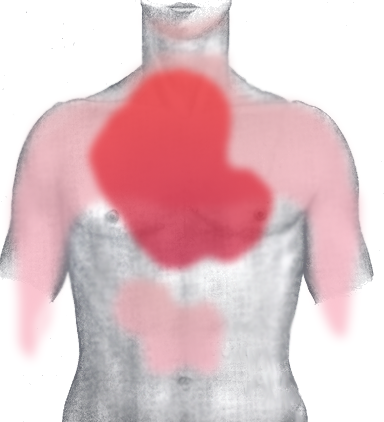
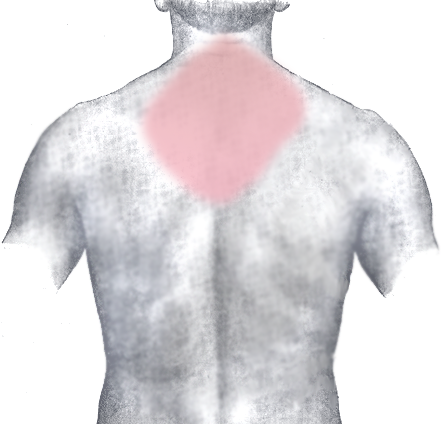
- Chest pain with exertion that lasts about 15 minutes
- Pain that radiates from the chest to the left arm associated with exertion
- Diaphoresis (sweating)
- Shortness of breath
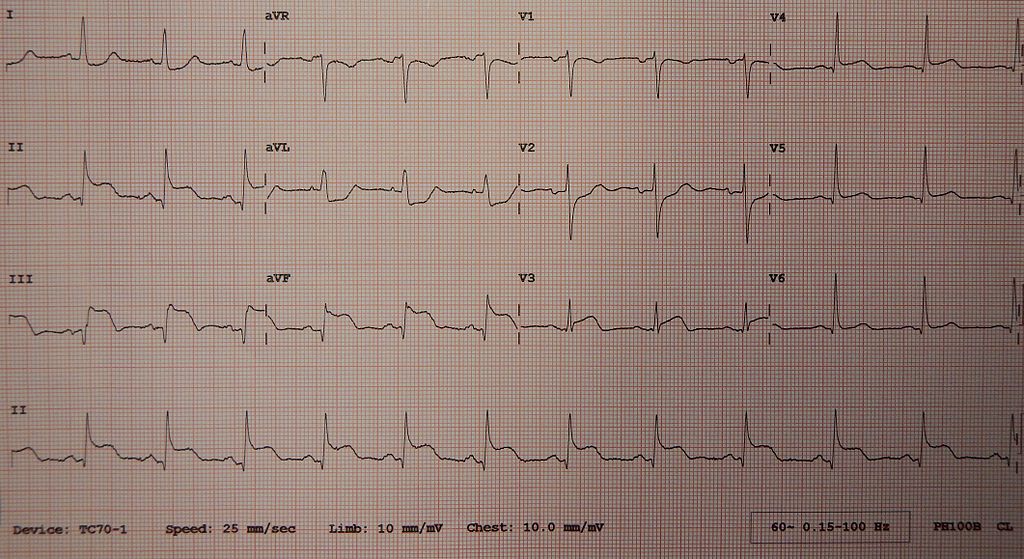
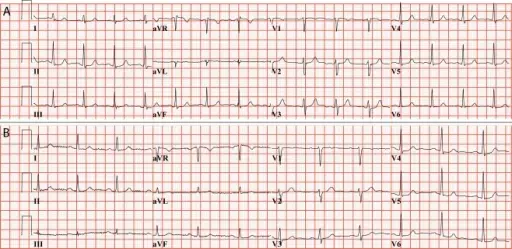
Classical electrocardiogram findings of stable angina show ST-segment depression.
The ST-segment depression is due to subendocardial ischemia.
Stable angina is treated by:
- Rest
- Nitroglycerin
Unstable Angina
Chest pain that occurs with rest is known as unstable angina.
Unstable angina is usually due to rupture of atherosclerotic plaque with thrombosis and incomplete occlusion of a coronary artery.
Unstable angina represents damage that myocytes can recover from (no necrosis).
Electrocardiogram (ECG) of unstable angina shows ST-segment depression because of subendocardial ischemia.
Unstable angina is relieved by nitroglycerin.
Patients with unstable angina are at increased risk of progression to myocardial infarction.
Prinzmetal Angina
Prinzmetal angina is episodic chest pain that is not related to exertion.
Prinzmetal angina is due to coronary artery vasospasm.
Prinzmetal angina represents damage that myocytes can recover from (no necrosis).
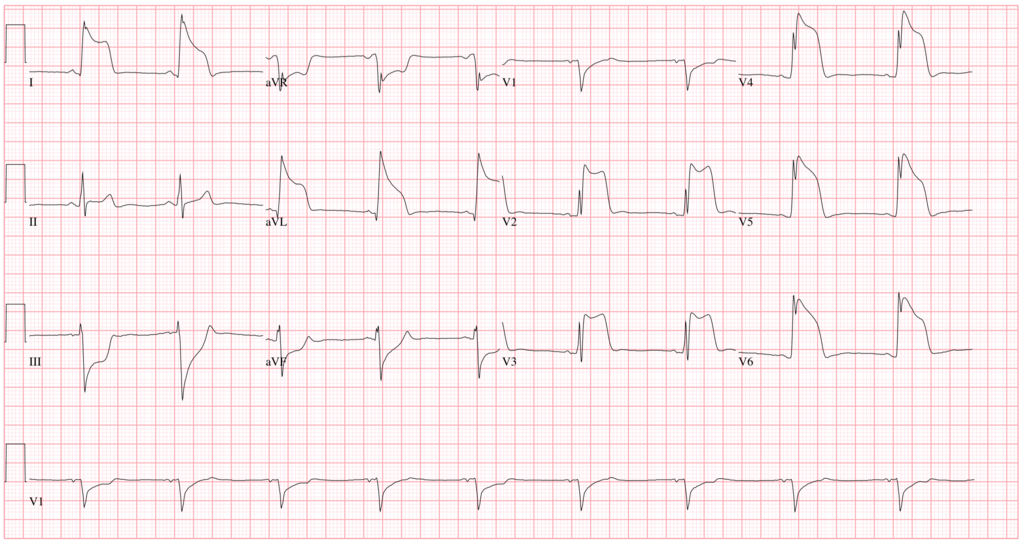
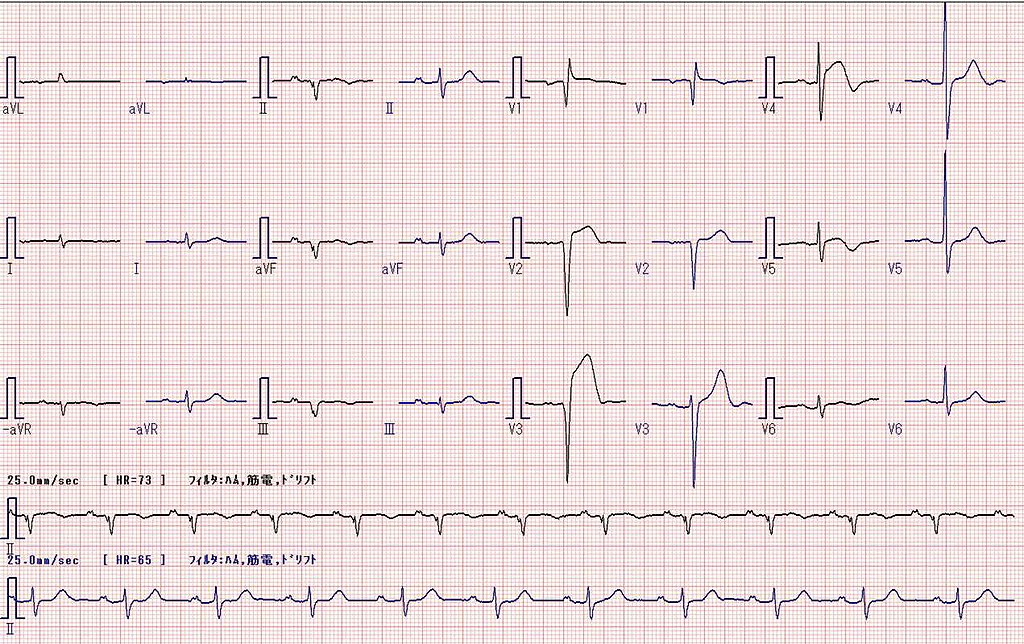
Electrocardiogram (ECG) of Prinzmetal angina shows ST-segment elevation due to transmural ischemia.
Treatment of Prinzmetal angina includes:
- Nitroglycerin
- Calcium channel blockers
Myocardial Infarction (MI)
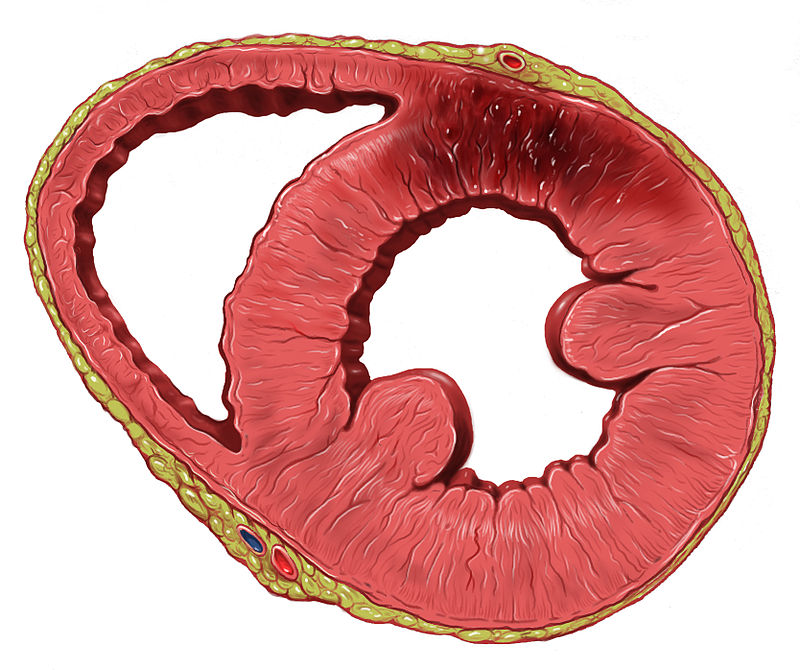
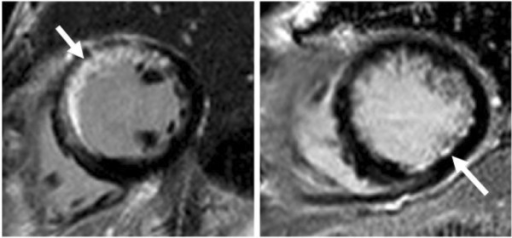
Necrosis of cardiac myocytes occurs in myocardial infarction (MI).
Myocardial infarction (MI) usually occurs due to rupture of an atherosclerotic plaque with thrombosis and complete occlusion coronary artery.
Risk factors of myocardial infarction (MI) include:
- Coronary artery vasospasm (due to Prinzmetal angina or cocaine use)
- Emboli
- Vasculitis (e.g. Kawasaki disease)
Clinical features of myocardial infarction (MI) include:
- Sever chest pain that radiates to the left arm
- Diaphoresis
- Dyspnea
Symptoms of myocardial infarction (MI) are not relieved by nitroglycerin.
The left ventricle (LV) is typically affected by infarction, while the right ventricle (RV) and both atria are typically spared.
The left anterior descending (LAD) artery is the most prevalent involved artery in myocardial infarction (MI) (45 percent of cases).
The right coronary artery (RCA) is the second most prevalent involved artery in myocardial infarction.
Classic cardiac vessel occlusion shows:
- Occlusion of left anterior descending artery (LAD) results in infarction of the anterior wall and anterior septum of the left ventricle
- Occlusion of the right coronary artery (RCA) results in infarction of the posterior wall, posterior septum, and papillary muscles of the left ventricle
- Occlusion of the left circumflex artery results in infarction of the left lateral wall of the left ventricle
The initial phase of myocardial infarction (MI) results in subendocardial necrosis involving less than 50 percent of the myocardial thickness (subendocardial infarction), and the EKG shows ST-segment depression.
Continued or severe ischemia leads to transmural necrosis involving most of the myocardial wall (transmural infarction), and the ECG shows ST-segment elevation.
Laboratory findings of myocardial infarction (MI) show:
- Elevated lactate dehydrogenase (LDH) levels
- Elevated troponin
- Elevated CK-MB
Troponin I is the most sensitive and specific marker (gold standard) for detecting myocardial infarction.
In myocardial infarction, troponin I levels:
- Rise 2 – 4 hours after infarction
- Peak at 24 hours
- Return to normalcy in 7 – 10 days
CK-MB is helpful to detect re-infarction that occurs days after an initial myocardial infarction (MI).
Creatine kinase MB (CK-MB) levels rise four to six hours after infarction, peak at 24 hours, and return to normalcy by 72 hours.
Treatment of myocardial infarction (MI) includes:
MONA BASH
- M-Morphine, 2.0 to 4.0 mg IV PRN for severe pain (May repeat dose of 2 to 8 mg at 5 to 15-minute intervals)
- O-Oxygen with nasal cannula to keep SaO2 > 92% to minimize ischemia
- N-Nitroglycerin 0.3-0.6 mg SL q5min PRN chest pain (Max: 3 doses within 15 minutes; this is done to vasodilate arteries and promote blood flow)
- A-Aspirin in chewable form first 325 mg (chew) if possible, then 81mg QD after that (avoid enteric coated Aspirin; this limits thrombosis)
- B-Beta-blocker such as Metoprolol tartrate 25mg po q6h to decrease the physical demand on the heart
- A-ACE inhibitor such as Lisinopril 5mg po BID if you are concerned about the patient’s blood pressure to reduce left ventricular dilation
- S-Statin that is high intensity such Atorvastatin 80mg po Qbedtime or rosuvastatin 20-40 mg daily
- H-Heparin for patients with non-ST elevations, to help anticoagulate them to limit thrombosis
Treatment of a myocardial infarction (MI) may result in a reperfusion injury.
Reperfusion Injury
Reperfusion of irreversibly damaged myocardial cells leads to calcium influx.
The calcium influx causes hypercontraction of myofibrils (contraction band necrosis).
Return of oxygen and inflammatory cells can result in free radical generation, which further damages myocytes resulting in reperfusion injury.
Sudden Cardiac Death
Sudden cardiac death is the unexpected death because of cardiac disease.
Sudden cardiac death occurs without symptoms or less than 1 hour after symptoms show up.
Sudden cardiac death is typically due to:
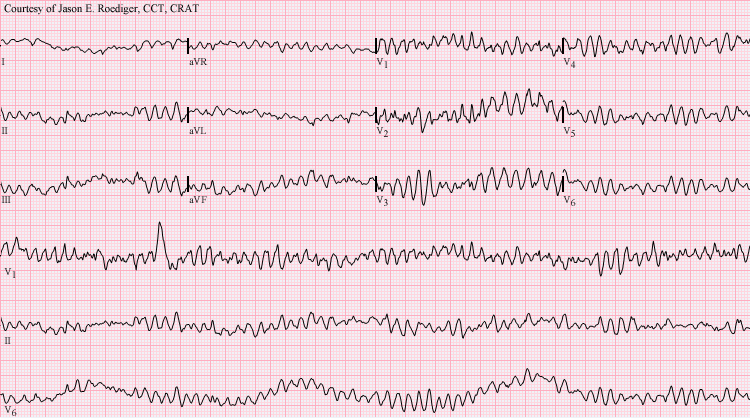
- Fatal ventricular arrhythmia
- Acute ischemia is the most common etiology
Risk factors for sudden cardiac death include:
- Atherosclerosis
- Mitral valve prolapse
- Cardiomyopathy
- Cocaine abuse
Ninety percent of patients that die from sudden cardiac death have preexisting severe atherosclerosis.
Chronic Ischemic Heart Disease
Chronic ischemic heart disease results in poor myocardial function because of chronic ischemic damage (with or without infarction).
Chronic ischemic heart disease may progress to congestive heart failure (CHF).