Myeloproliferative Disorders
Myeloproliferative Disorders Pathology Video
Myeloproliferative disorders are neoplastic proliferation of myeloid cells.
Myeloproliferative disorders typically occur in late adulthood (average age is 55-years-old).
Myeloproliferative disorders are associated with:
- Leukocytosis (high white blood cell count)
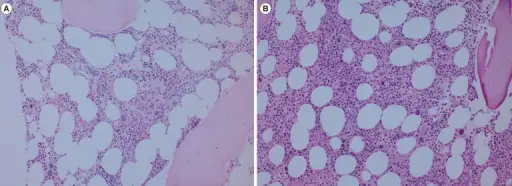
- Hypercellular bone marrow
In myeloproliferative disorders there is an increase in all the cells of myeloid lineage.
Myeloproliferative disorders are categorized based on the dominant myeloid cell that is produced.
Complications include of myeloproliferative disorders include:
- High risk of hyperuricemia and gout because of turnover of cells
- Transition into acute leukemia or progression to marrow fibrosis
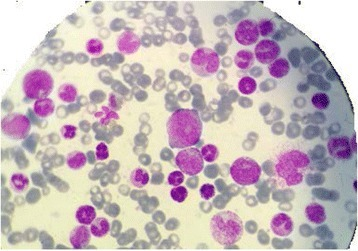
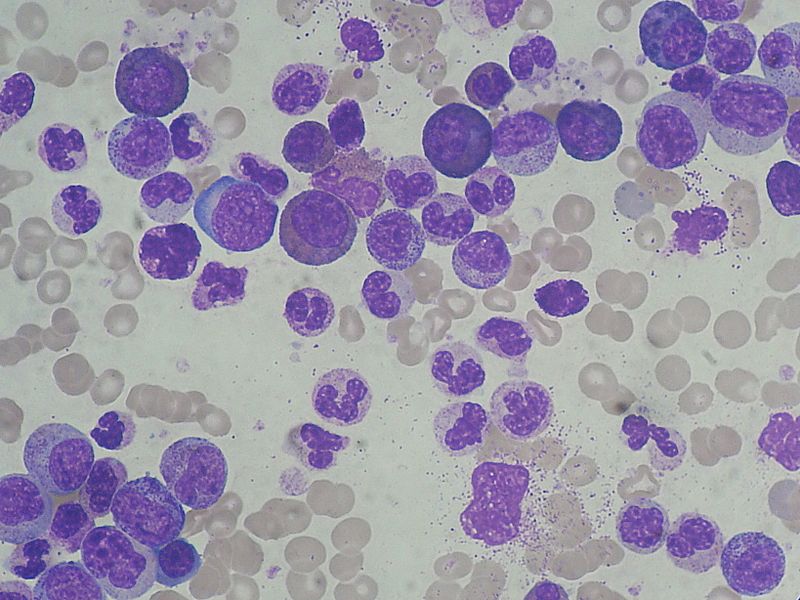
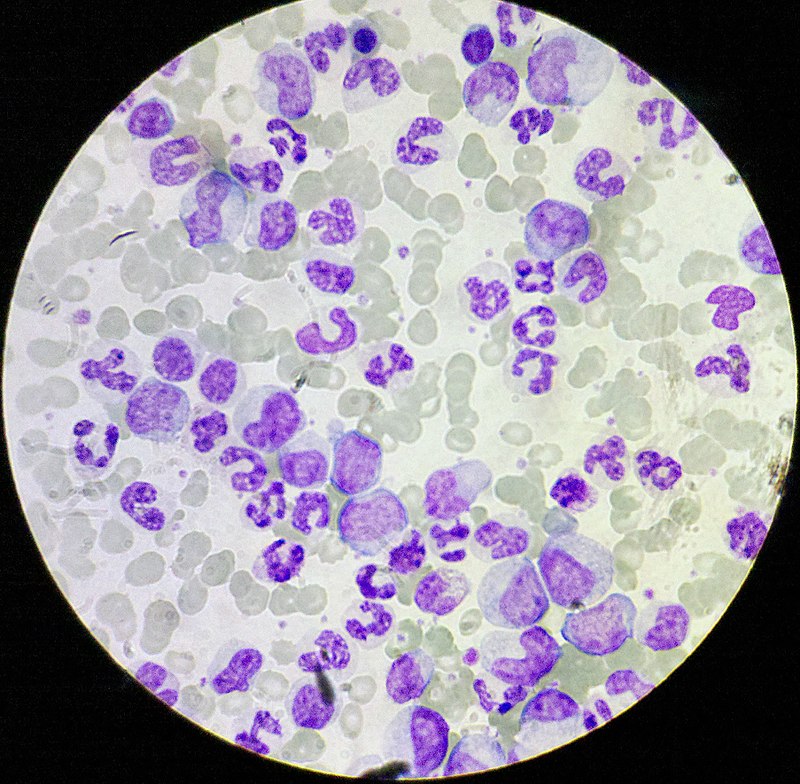
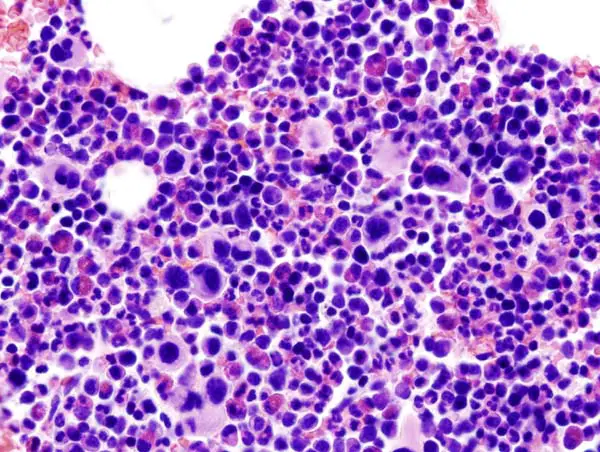
Chronic Myeloid Leukemia (CML)
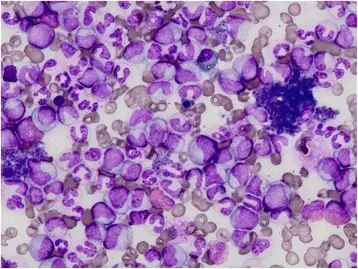
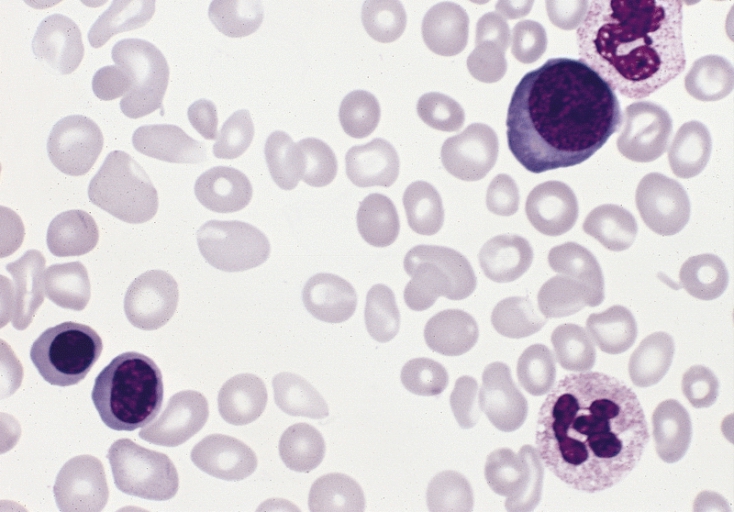
Chronic myeloid leukemia is due to neoplastic proliferation of mature myeloid cells, in particular, granulocytes and granulocyte precursors.
An increase of basophils is characteristic of chronic myeloid leukemia (CML).
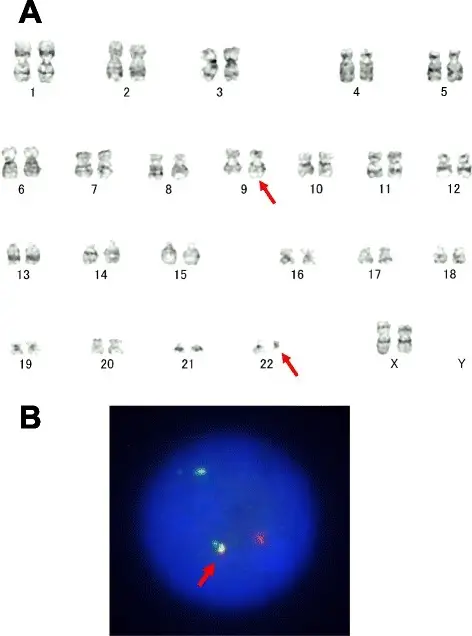
Chronic myeloid leukemia is typically driven by the Philadelphia chromosome t(9;22), which results in the production of a BCR-ABL fusion protein with higher tyrosine kinase activity.
Imatinib, which inhibits tyrosine kinase activity, is the first line of treatment of chronic myeloid leukemia.
Splenomegaly is common in chronic myeloid leukemia.
Spleen enlargement indicates an accelerated phase of disease.
Acute leukemia transformation typically occurs shortly after.
Due to a mutation in a pluripotent stem cell, chronic myeloid leukemia can progress:
- Acute myeloid leukemia (AML) (2/3 of cases)
- Acute lymphoblastic leukemia (ALL) (1/3 of cases)
Leukocyte alkaline phosphatase (LAP) staining distinguishes chronic myeloid leukemia (CML) from a leukemoid reaction.
Leukocyte alkaline phosphatase (LAP) is negative in chronic myeloid leukemia (CML).
Leukocyte alkaline phosphatase (LAP) is positive in leukemoid reactions, such as reactive neutrophilic leukocytosis.
The granulocytes in a leukemoid reactions are what cause the leukocyte alkaline phosphatase (LAP) positivity.
Polycythemia Vera (PV)
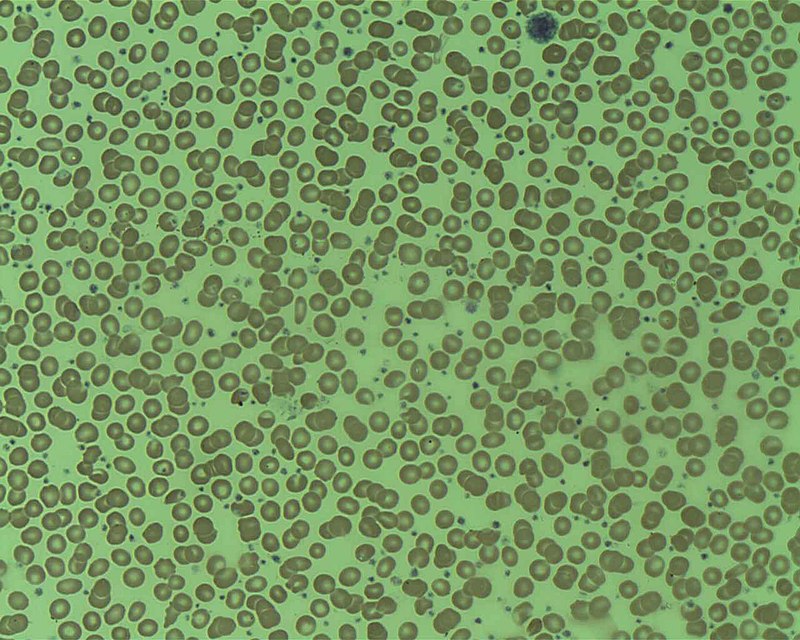
Polycythemia vera (PV) is due to the neoplastic proliferation of mature myeloid cells, particularly red blood cells.
In polycythemia vera (PV) granulocytes and platelets are typically increased.
Polycythemia vera is related to JAK2 kinase mutation.
Many clinical symptoms of polycythemia vera (PV) are associated with viscous blood.
Symptoms of polycythemia vera (PV) include:
- Blurry vision
- Headache
- High risk of venous thrombosis
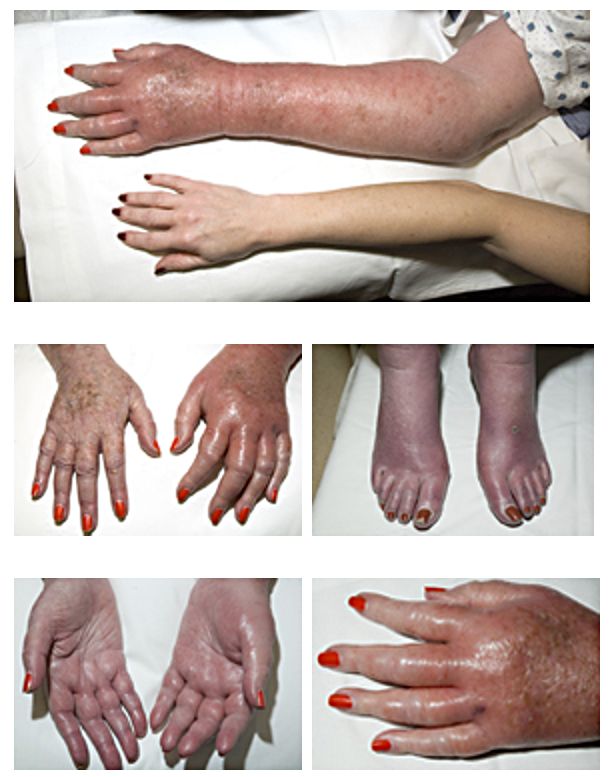
- Flushed face because of congestion (plethora)
- Itching, particularly after a bath or shower (because of histamine release from mast cells)
Treatment of polycythemia vera (PV) includes:
- Phlebotomy (first line)
- Hydroxyurea (second line)
Without medical intervention, polycythemia vera (PV) typically results in death within two years.
Reactive polycythemia must be distinguished from polycythemia vera (PV).
In polycythemia vera (PV):
- SaO2 is normal
- Erythropoietin (EPO) levels are low
In reactive polycythemia (PV):
- SaO2 is low
- EPO is elevated
Reactive polycythemia is brought on by:
- Lung illness
- Sleep apnea
- High altitude exposure
- Renal disease
Reactive polycythemia with elevated erythropoietin (EPO) and normal SaO2 levels are typically caused by ectopic renal cell carcinoma production of EPO.
Essential Thrombocythemia (ET)
Essential thrombocythemia (ET) is due to the neoplastic proliferation of mature myeloid cells, in particular, platelets.
Red blood cells and granulocytes are also raised in essential thrombocythemia (ET).
Essential thrombocythemia (ET) is typically due to a JAK2 kinase mutation.
Symptoms of essential thrombocythemia (ET) are related excess abnormal platelets.
There is a high risk of bleeding and/or thrombosis in essential thrombocythemia (ET).
In rare cases essential thrombocythemia (ET) may advance to marrow fibrosis or acute leukemia.
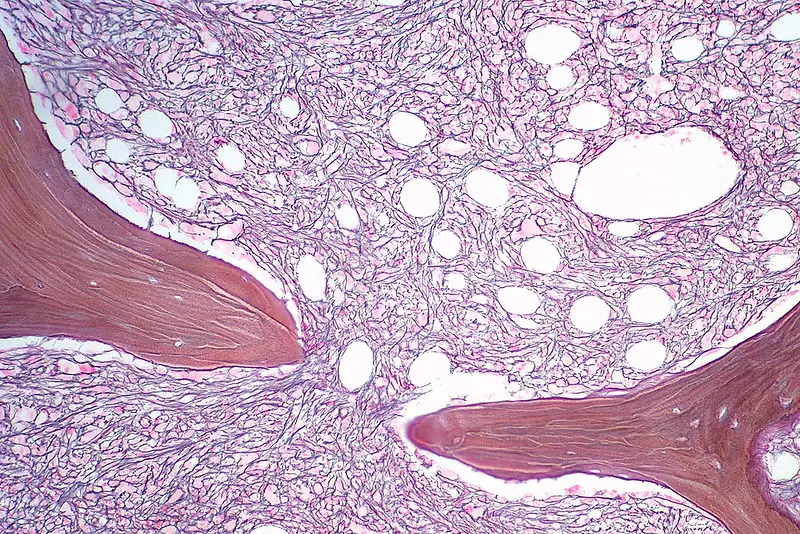
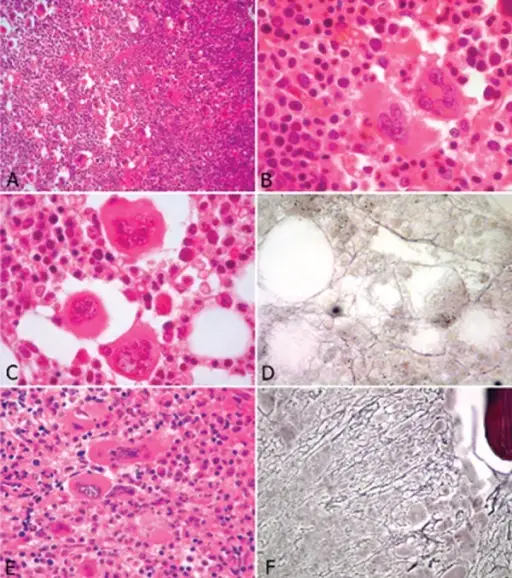
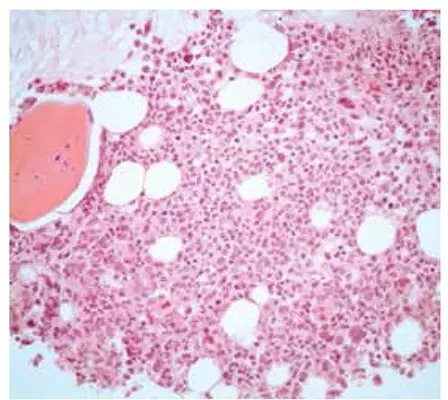
Myelofibrosis
Myelofibrosis is due to the neoplastic proliferation of mature myeloid cells, in particular, megakaryocytes.
Myelofibrosis is related to JAK2 kinase mutation in 50 percent of cases.
Platelet-derived growth factor (PDGF), which megakaryocytes overproduce, causes marrow fibrosis.
In myelofibrosis, splenomegaly occurs due to extra-medullary hematopoiesis.
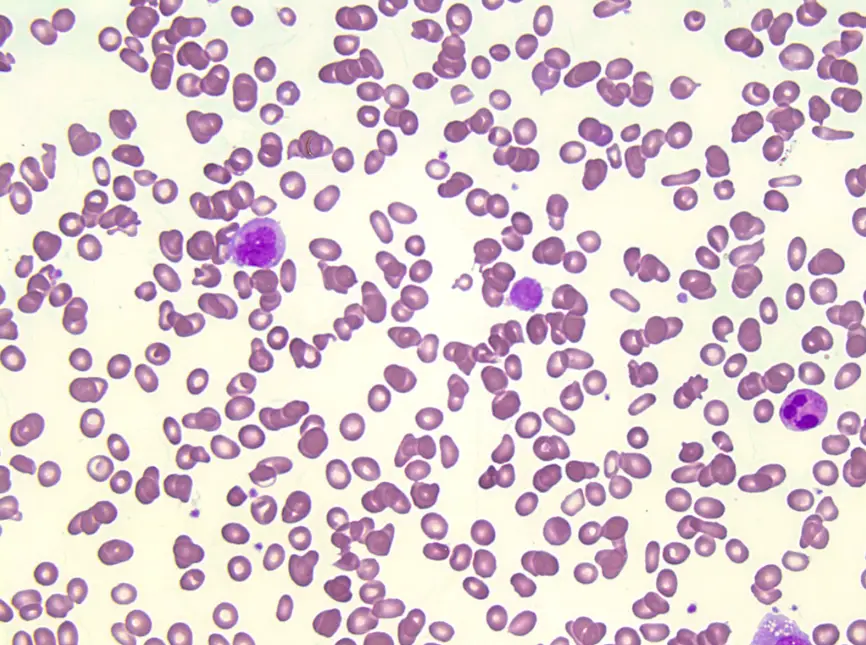
Histology of myelofibrosis is characterized by:
- A leukoerythroblastic smear with tear-drop red blood cells
- Nucleated red blood cells
- Immature granulocytes
Patients with myelofibrosis have an increased risk of infection, thrombosis, and bleeding.