Necrosis
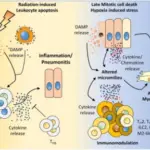
Necrosis is the premature pathologic death of cells in living tissue.
Acute inflammation can result in the death of a large group of cells which will cause necrosis.
Necrosis is always pathologic.
Necrosis is never physiologic.
The patterns of necrosis include:
- Coagulative necrosis
- Liquefactive necrosis
- Gangrenous necrosis
- Fat necrosis
- Caseous necrosis
Coagulative Necrosis
In coagulative necrosis the necrotic tissue remains firm, end organ structure is maintained, and even cellular structure is maintained; however the nuclei disappear.
Ischemic infarctions are known to cause coagulative necrosis in most tissues.
Infarctions may be wedge shaped.
After an ischemic infarction if blood is reintroduced to loosely organized tissue a red infarction may occur.
Note the lack of tiny blue nuclei in necrotic tissue.
Coagulative necrosis does not happen in the brain (liquefactive necrosis will occur).
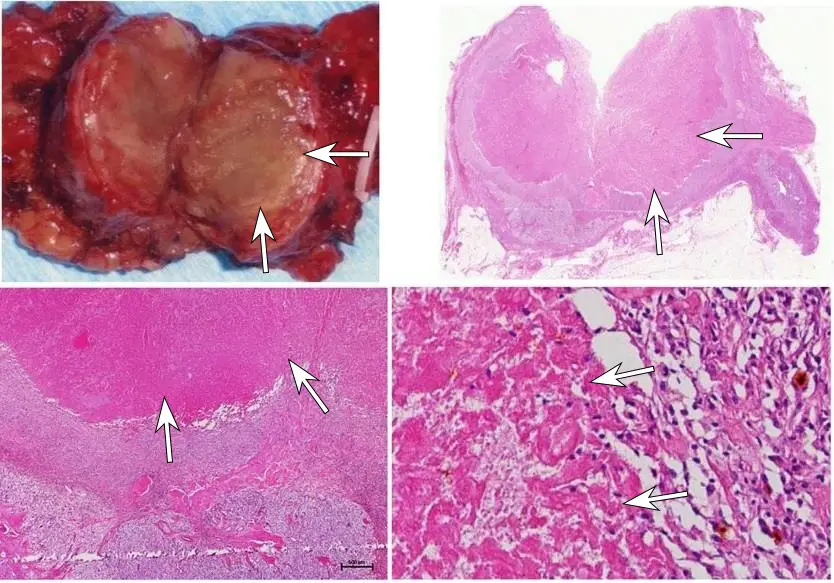
Liquefactive Necrosis
After a brain infarction the proteolytic enzymes that originate from microgliosis will cause hydrolysis and liquefication of the brain parenchyma.
In an abscess, the proteolytic enzymes released from the neutrophils will liquefy the tissue.
In pancreatitis, the proteolytic enzymes that originate from the pancreas will liquefy the pancreas.
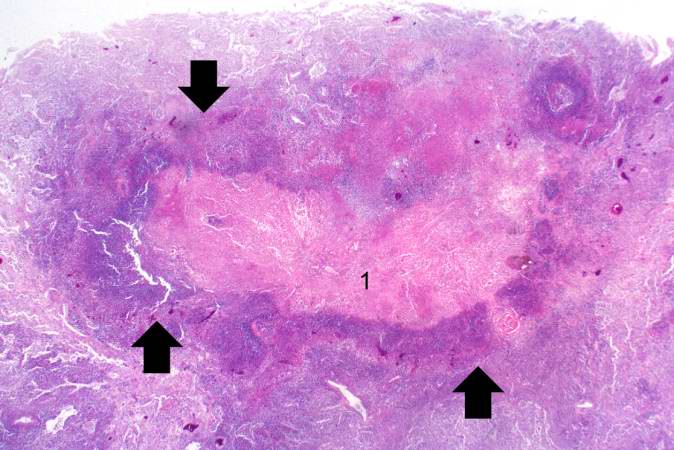
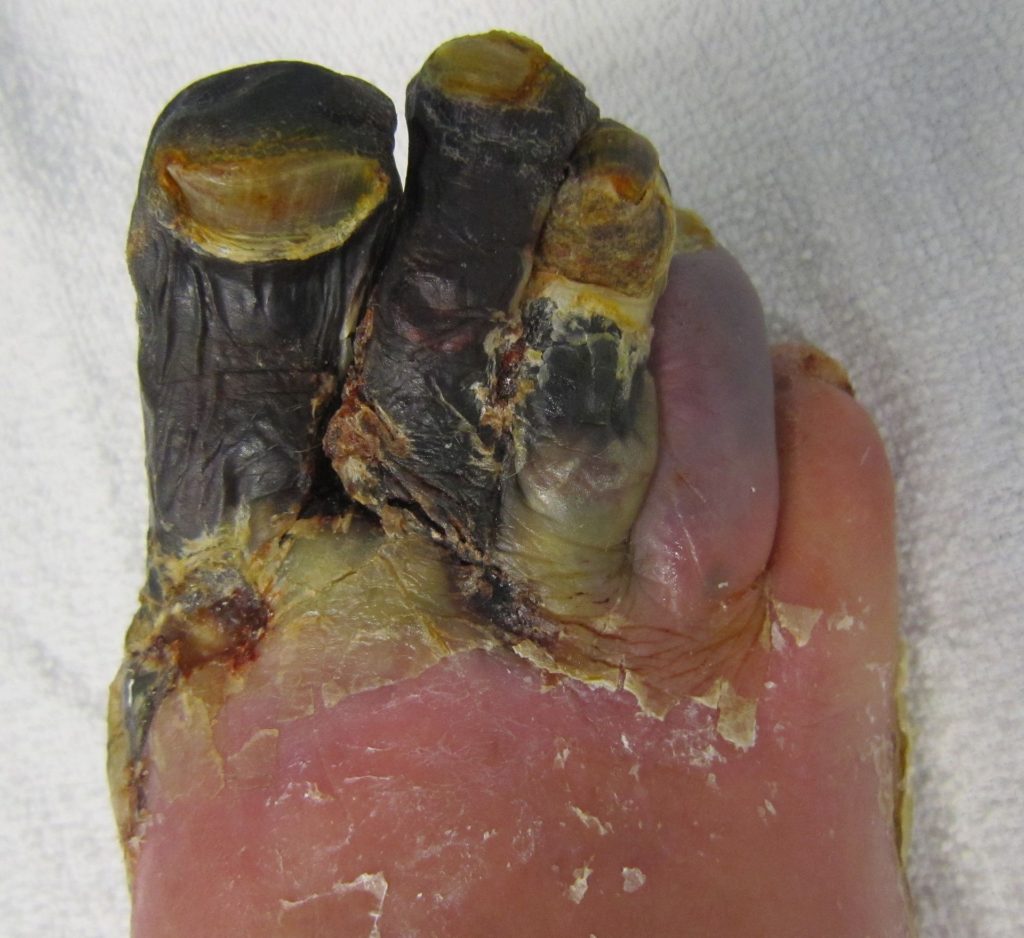
Gangrenous Necrosis
Gangrenous necrosis results from a lack of blood supply that leads to lack of oxygen reaching a tissue that leads to cell death and tissue damage.
There are multiple types of gangrenous necrosis to be aware of, which include:
- Dry gangrene
- Wet gangrene
- Gas gangrene
- Internal gangrene
- Necrotizing fasciitis
- Fournier gangrene
Dry gangrene is a form of coagulative necrosis that resembles mummified corpses, which usually effects the distal appendages.
Wet gangrene is gangrenous necrosis that is infected by bacteria that promote liquefactive necrosis.
Gas gangrene is a medical emergency due to gangrenous necrosis that is infected by bacteria that produce gas (such as Clostridium perfringens).
Internal gangrene is gangrene that occurs when blood flow to an internal organ is blocked (such as an incarcerated hernia).
Necrotizing fasciitis is also known as flesh eating disease, and is a type of aggressive coagulative necrosis with superimposed infection by group A streptococcus (GAS) bacteria that effect the skin and fascia.
Fournier gangrene is a type of necrotizing fasciitis that usually affects the male genitals and groin region.
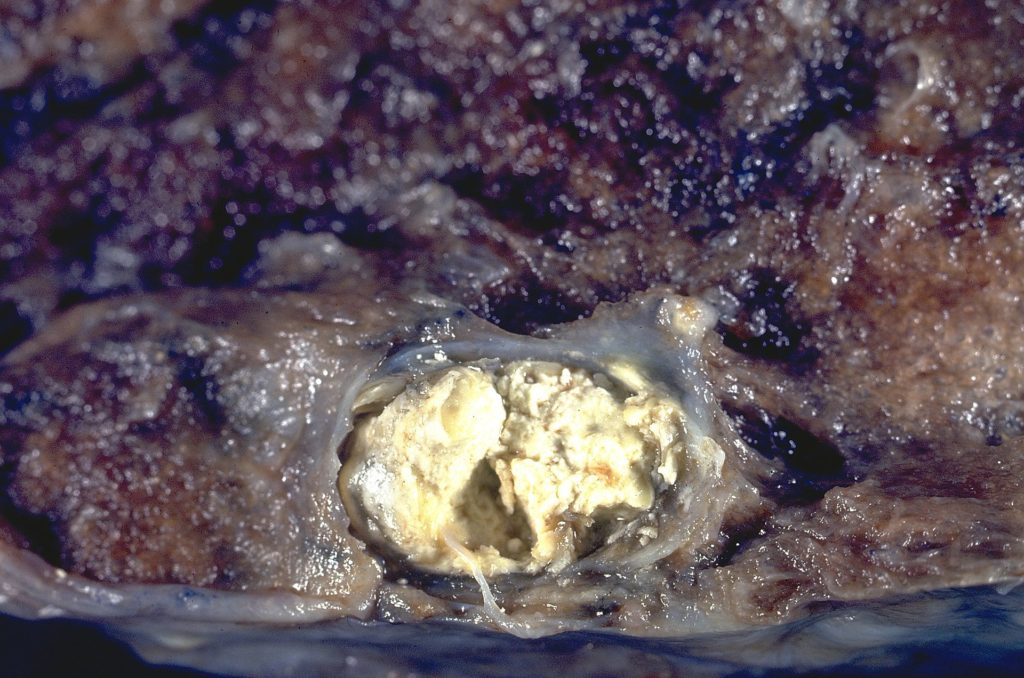
Caseous Necrosis
Caseous necrosis has the appearance of a congealed cheese.
The most tested form of caseous necrosis involves the granulomas of the lungs associated with tuberculosis.
Fat Necrosis
Fat necrosis is the necrosis of adipose tissue that results in the deposition of calcium.
Fat necrosis typically has a greasy, chalky white appearance.
Saponification is the biochemical reaction associated with fat necrosis.
Saponification results in a type of dystrophic calcification.
In dystrophic calcification, necrotic tissue serves as a nidus that calcification may build upon.
Classical causes of fat necrosis are:
- Pancreatitis (fat necrosis of peri-pancreatic fat, along with liquefactive necrosis of pancreatic tissue due to free pancreatic enzymes)
- Trauma to adipose tissue such as the breast
Metastatic calcification and dystrophic calcification are two completely separate entities.
The difference between metastatic and dystrophic calcification are:
- Metastatic calcification is deposition of calcium in normal tissue due to excessive calcium levels in the system
- Dystrophic calcification is deposition of calcium in pathologic tissues

Fibrinoid Necrosis
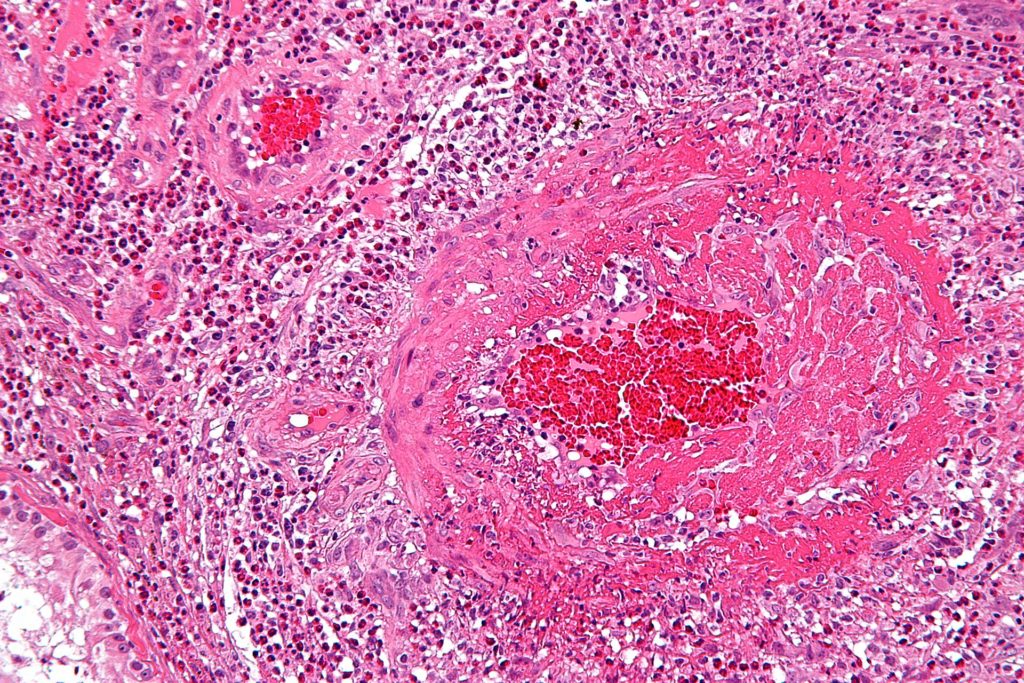
Fibrinoid necrosis is necrosis associated with fibrin deposition in blood vessel walls.
Necrotic damage to blood vessel walls may result in fibrinoid necrosis.
Fibrin may leak into the vessel wall resulting in a bright pink deposit that can be visualized microscopically on the vessel wall.
Fibrinoid necrosis is a feature of malignant hypertension, vasculitis, and in the placenta due to pre-eclampsia.