Other Disorders of Hemostasis Pathology Video
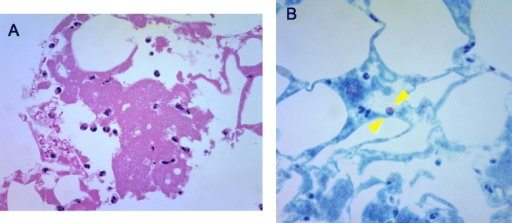
Heparin Induced Thrombocytopenia
Heparin induced thrombocytopenia is the destruction of platelets that results from heparin therapy.
Heparin induced thrombocytopenia (HIT) is an immune complication due to antibodies directed against complexes containing heparin and a platelet factor 4 (PF4).
Platelet fragments could activate remaining platelets and cause thrombosis.
Never give heparin to a patient that has experienced heparin induced thrombocytopenia (HIT).
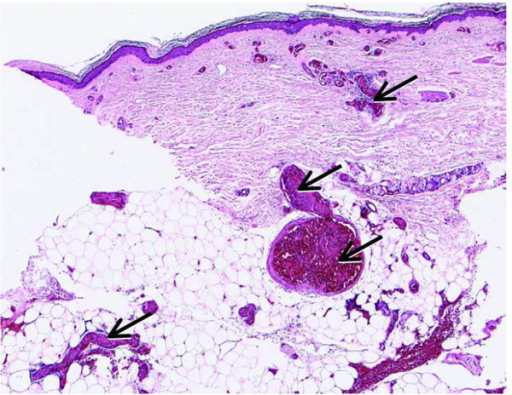
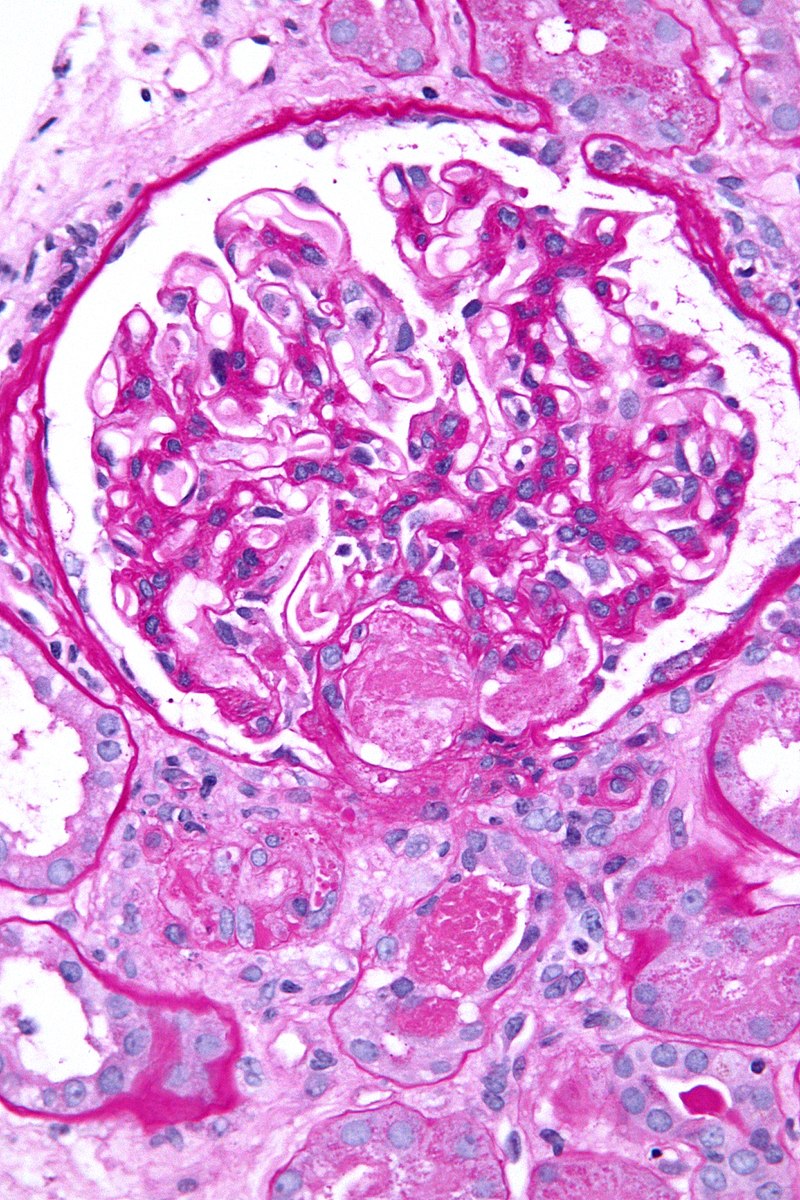
Disseminated Intravascular Coagulation
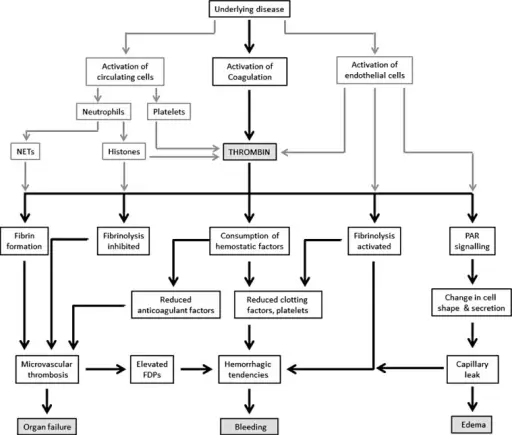
Disseminated intravascular coagulation (DIC) is due to the activation of the coagulation cascade by pathology.
Ischemia and infarction are brought on by widespread microthrombi.
Bleeding is caused by factors and platelet consumption.
Mucosal bleeding is a common symptom of disseminated intravascular coagulation (DIC).
Disseminated intravascular coagulation (DIC) is usually accompanied by another medical issue such as:
The majority of the time DIC is due to another disease process.
- Obstetric complications in which the amniotic fluid’s tissue thromboplastin initiates coagulation
- Endotoxins from the bacterial wall and macrophage derived cytokines (such as tumor necrosis factor (TNF) and interleukin-1 (IL-1)) cause endothelial cells to produce tissue factors in sepsis (particularly with E. Coli or N. meningitidis)
- Coagulation gets activated by adenocarcinoma mucin
- Primary granules in acute promyelocytic leukemia (APL)
- Coagulation activated by rattlesnake venom
Laboratory findings of disseminated intravascular coagulation (DIC) include:
- Decreased platelet count
- Decreased fibrinogen
- Increased PT
- Increased PTT
- Increased INR
- Increased D-dimer
- Peripheral smear showing helmet cells and schistocytes
Elevated fibrin split products are present, especially D-dimer.
The best screening test for disseminated intravascular coagulation (DIC) is elevated D-dimer.
The D-dimer is from splitting of cross-linked fibrin.
The D-dimer is not derived from splitting of fibrinogen.
Treatment of disseminated intravascular coagulation (DIC) includes:
- Addressing the underlying cause as well
- Transfusing cryoprecipitate (contains coagulation factors) and blood products if clinically indicated
Disorders of Fibrinolysis
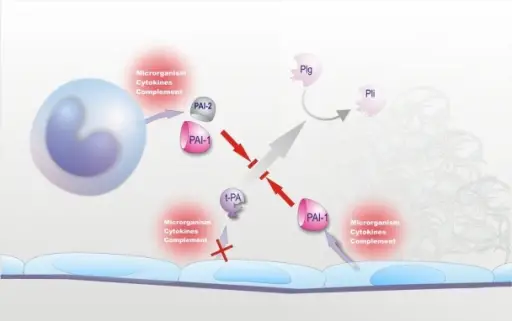
After the injured vessel heals, the thrombus is removed by normal fibrinolysis.
Plasminogen is transformed into plasmin by tissue plasminogen activator (TPA).
Plasmin breaks down coagulation components, degrades serum fibrinogen and fibrin, and prevents platelet aggregation.
Plasmin is deactivated by alpha2-antiplasmin (a2AP).
Plasmin overactivity, which results in increased cleavage of serum fibrinogen, is the cause of fibrinolysis disorders.
Examples of plasmin overactivity include:
- Radical prostatectomy due to release of urokinase causes plasmin to be activated
- Reduced synthesis of alpha2-antiplasmin (a2AP) due to liver cirrhosis
- Increases hemorrhage while presenting (resembles disseminated intravascular coagulation (DIC))
Laboratory findings in disorders of fibrinolysis include:
- Increased PT
- Increased PTT
- Increased bleeding time
- Increased fibrinogen split products without elevated D-dimer
- Normal platelet count
Plasmin destroys coagulation factors and blocks platelet aggregation.
Treatment is aminocaproic acid which prevents plasminogen activation.