Traumatic Brain Injuries Pathology Video
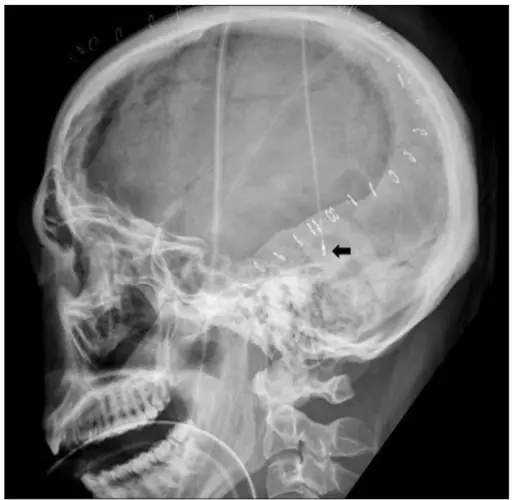
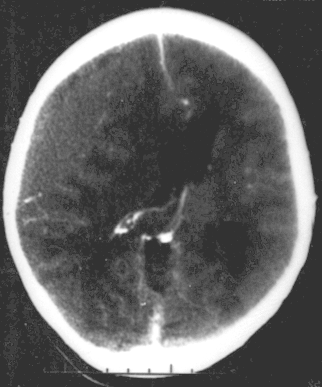
Epidural Hematoma
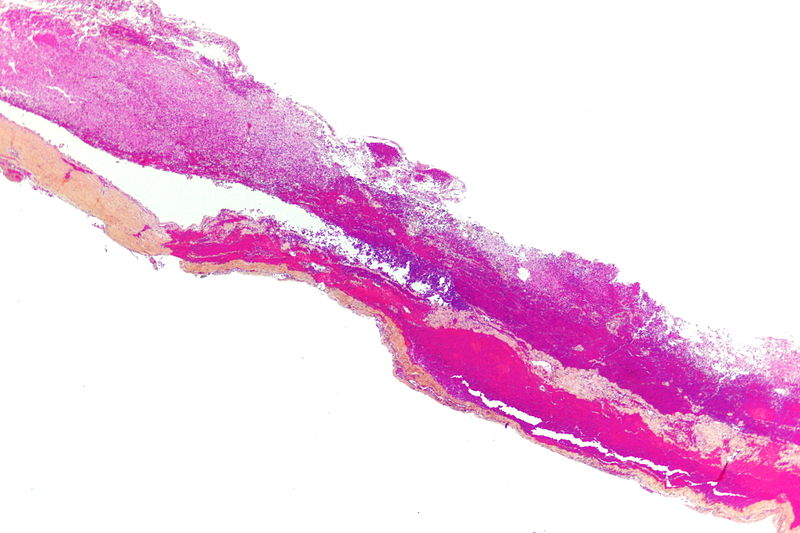
An epidural hematoma develops when blood accumulates between the skull and dura mater.
Epidural hematomas are usually the result of skull fracture and rupture of a major vessel of the brain.
Neurologic symptoms like lucid intervals may come initially.
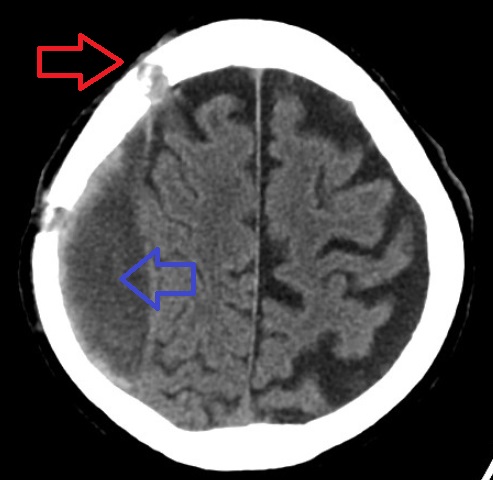
Radiology of epidural hematomas classically show a lens-shaped lesion representing the dura separated from the skull by hemorrhage.
Complications of epidural hematomas include herniation, seizure, and death.
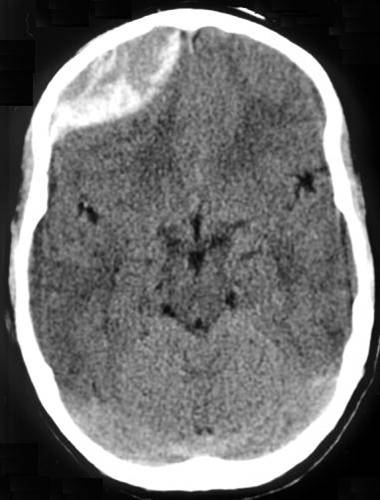
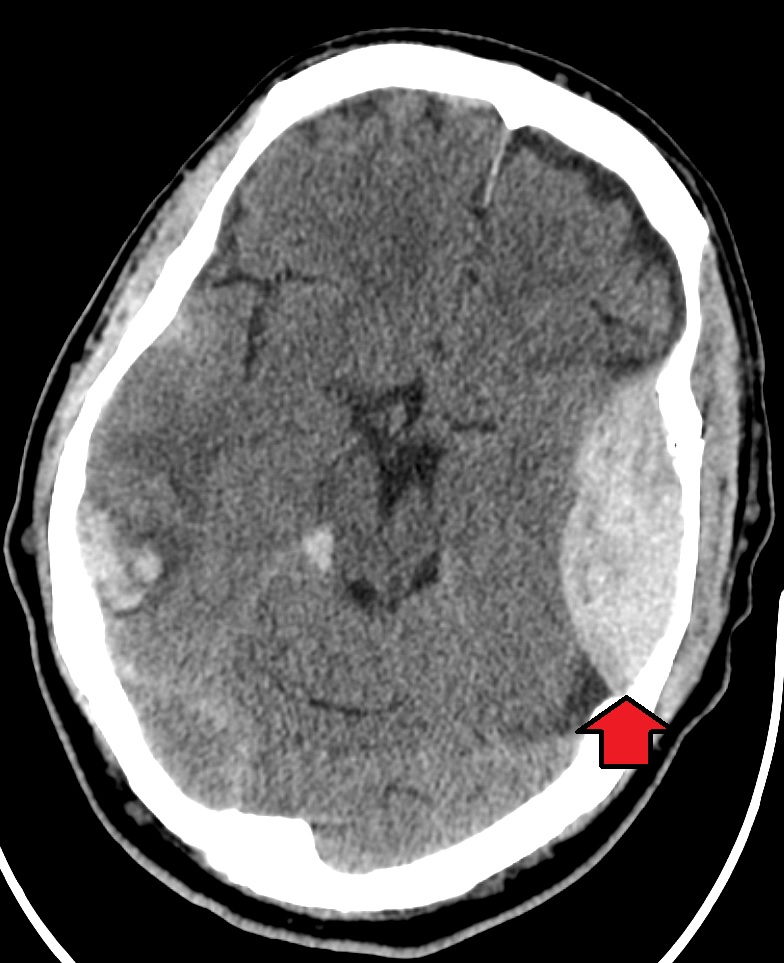
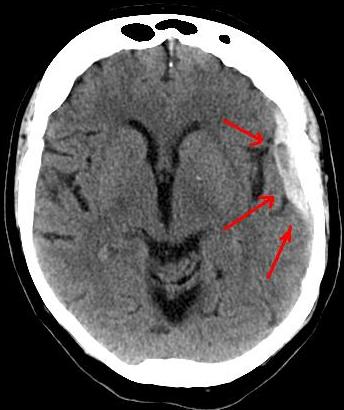
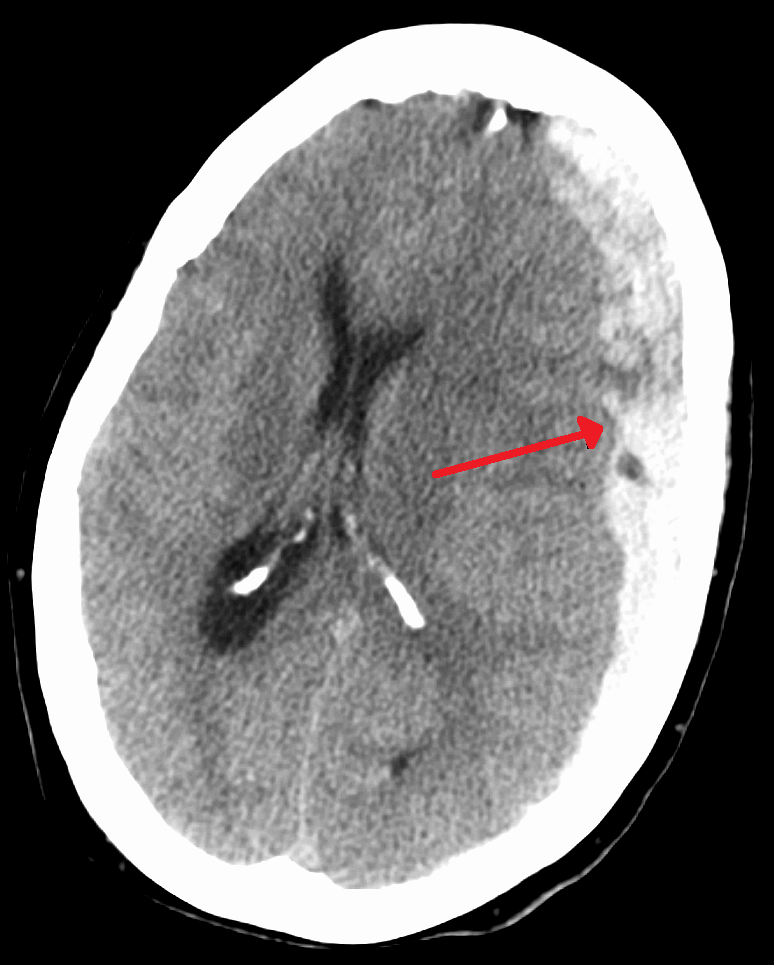
Subdural Hematoma
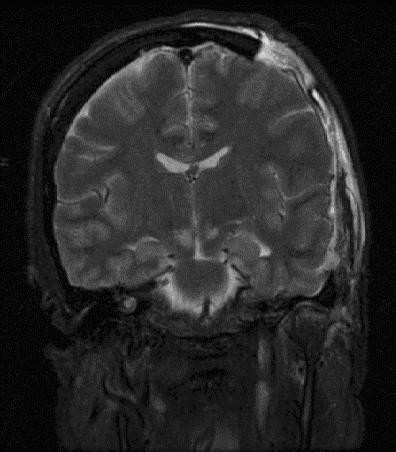
An accumulation of blood on the surface of the brain is known as a subdural hematoma.
Subdural hematomas develop after trauma because the bridging veins between the dura and arachnoid rupture.
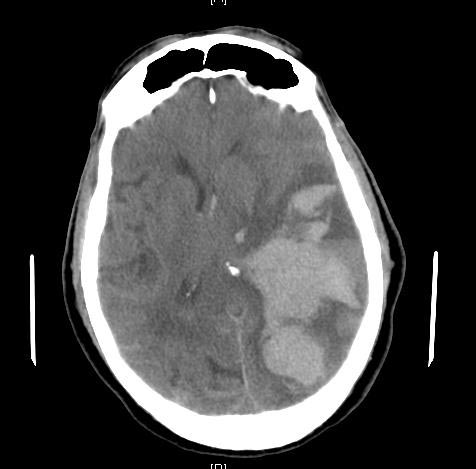
Radiology of subdural hematomas reveal a lesion with a crescent shape.
Subdural hematomas may present with neurologic symptoms that progress with the severity of the hematoma.
Age-related cerebral atrophy, which stretches the veins, contributes to an increased incidence rate of subdural hematomas in the elderly.
Herniation is a potentially lethal complication of a subdural hematoma.
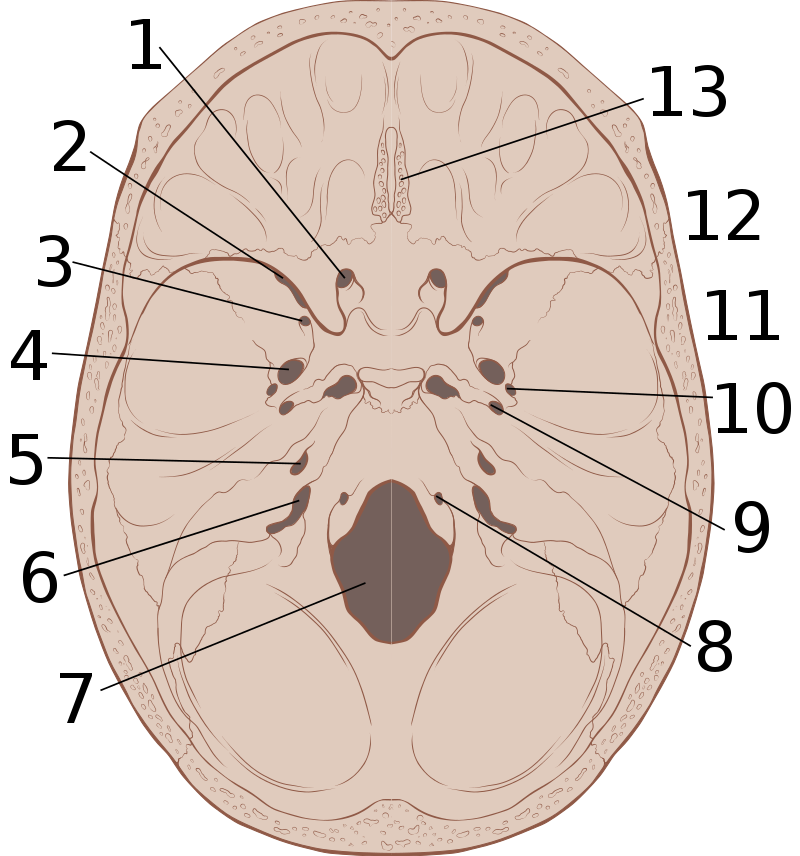
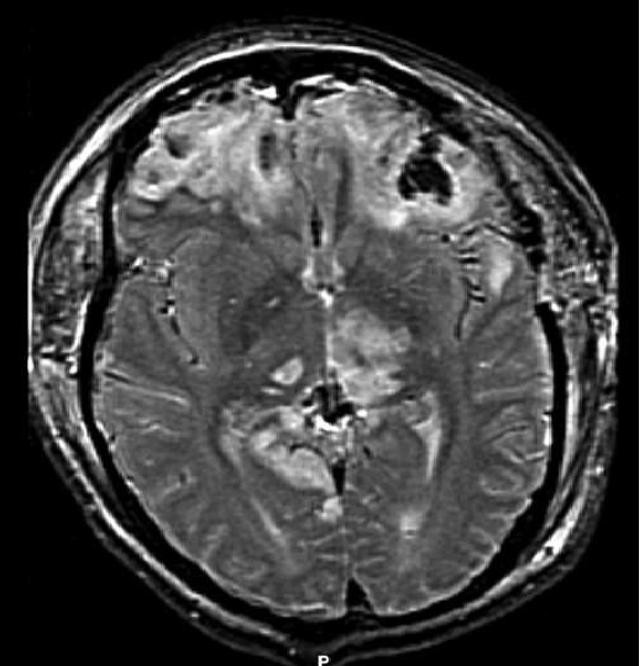
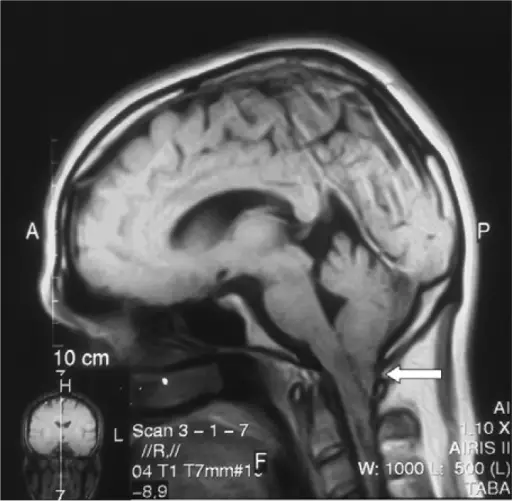
Herniation
The displacement of brain tissue as a result of a force or higher intracranial pressure is known as herniation.
The most frequent type of intracranial herniation is a subfalcine herniation.
In subfalcine herniation the brain tissue protrudes through the falx cerebri.
Uncal herniation is another type of herniation, in which the temporal lobe uncus is displaced under the tentorium cerebelli.
In an uncal herniation, compression of cranial nerve III, the oculomotor nerve, causes the ipsilateral eye to move “down and out” and the pupil to dilate.
Other potential complications of herniation include:
- Cardiopulmonary arrest occurs when the brain stem is compressed
- Infarction of the occipital lobe or the opposite homonymous hemianopia are caused by compression of the posterior cerebral artery
- Infarction occurs when the anterior cerebral artery is compressed
- Seizure(s)
- Death