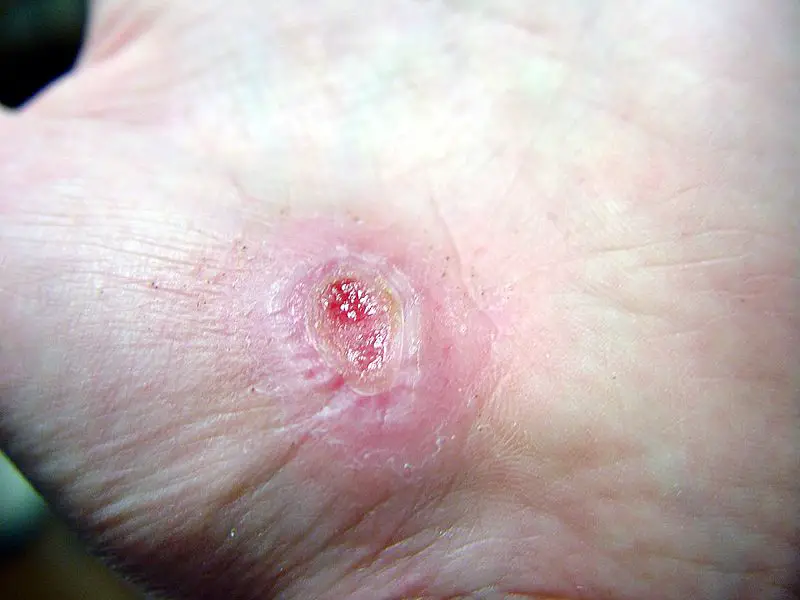
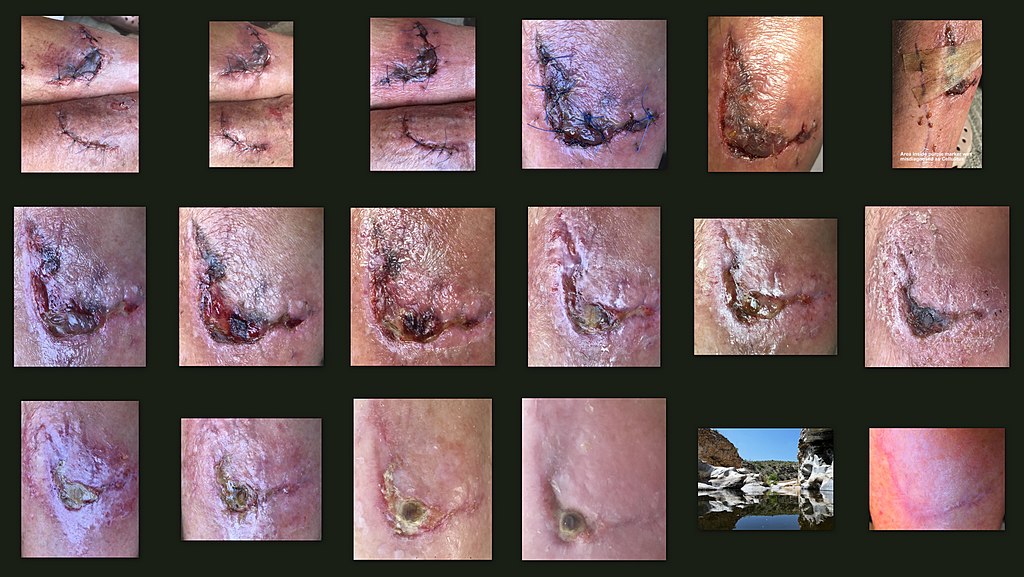
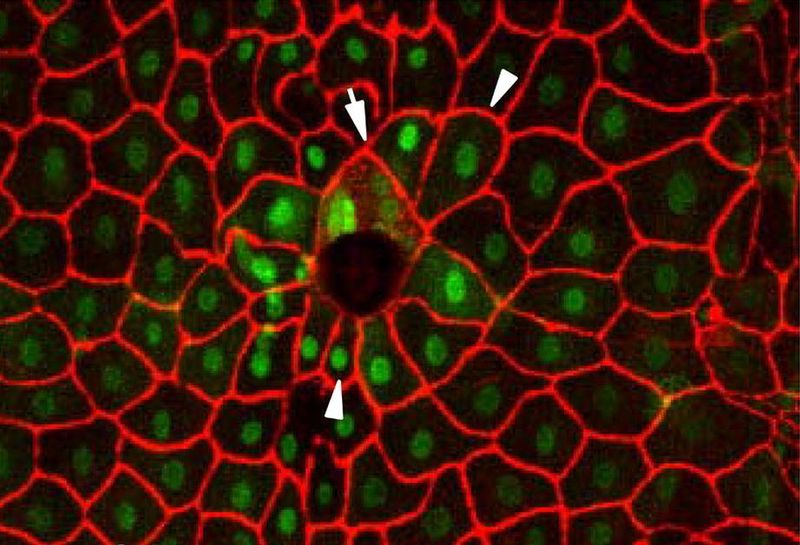
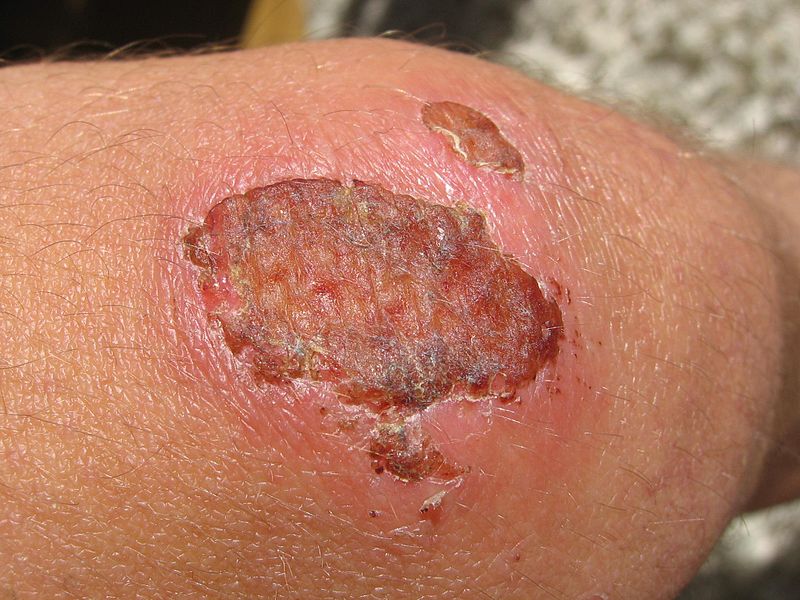
Wound Healing
When inflammation starts, the healing process is initiated.
Healing occurs as a result of:
- Regeneration of tissue with native tissue cells
- Repair of tissue with fibrous scar tissue
Regeneration
Native tissue is used to replace damaged tissue.
Based on their ability to regenerate, tissues are classified into three different types:
- Labile
- Stable
- Permanent
Labile Tissue
Labile tissues are constantly regenerating, and have the best ability to regenerate.
The stem cells in labile tissues cycle continually to regenerate the tissue.
Examples of labile tissues include:
- Skin (stem cells in the basal layer)
- Bone marrow (CD34+ hematopoietic stem cells)
- Gastrointestinal tract (stem cells in the gastrointestinal crypts)
Labile tissues contain vast amounts of labile cell populations.
Stabile Tissue
Stable tissues are primarily made up of quiescent (G0) cells.
The cells that compose stable tissues have the ability to re-enter the cell cycle and regenerate tissue when necessary.
Examples of stabile tissues include:
- Liver
- Kidney (the proximal renal tubules)
The regeneration of the liver by compensatory hyperplasia following partial resection is a classic example of stable tissue.
Each hepatocyte generates new cells and then re-enters quiescence.
Permanent Tissue
Permanent tissues do not regenerate.
Permanent tissues are generally repaired by a fibrous scar, due to the inability of permanent tissues inability to regenerate tissue.
Examples of permanent tissues include:
- Brain
- Heart
- Skeletal muscle
Loss of regenerative stem cells (e.g. deep cuts in the skin) may also lead to scar formation.
Types of Collagen
In order to understand tissue repair, it is best to first understand the main types of collagen.
The types of collagen include:
- Type I collagen: The strongest tensile strength, found in bone and scars
- Type II collagen: Found in cartilage
- Type III collagen: Pliable cartilage, found in blood vessels, granulation tissue, embryonic skin
- Type IV collagen: Basement membrane cartilage
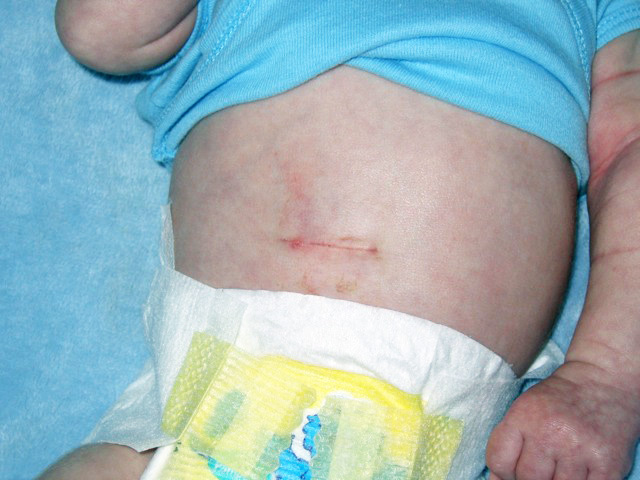
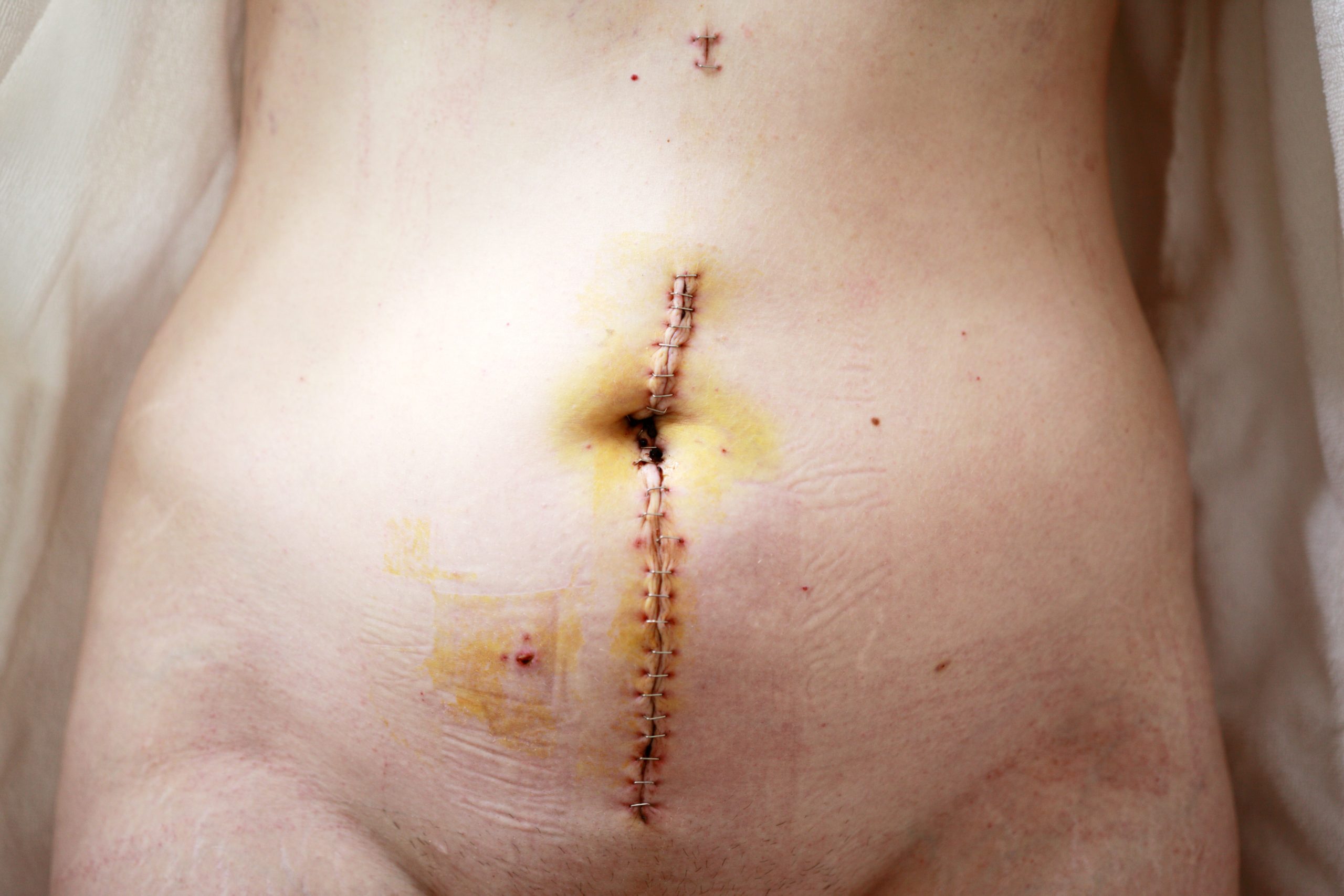
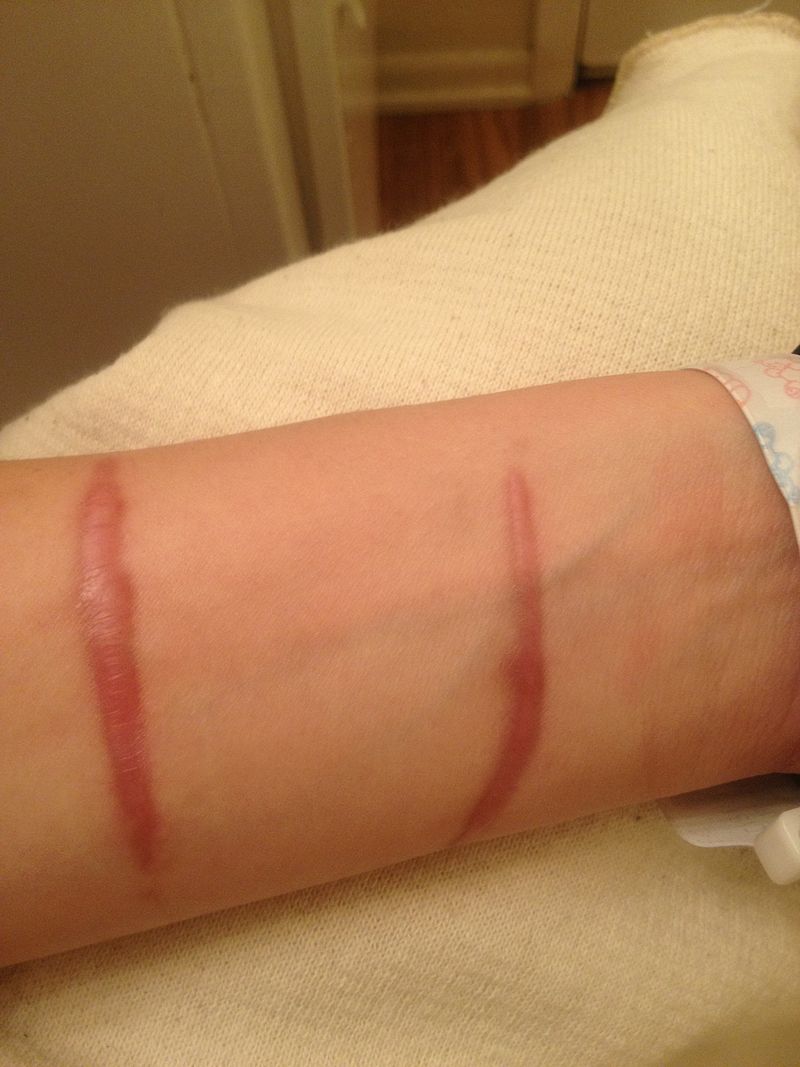
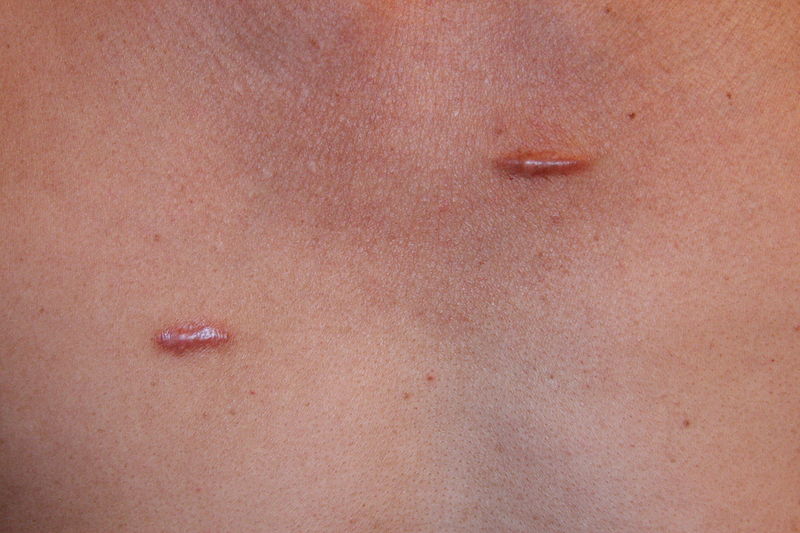
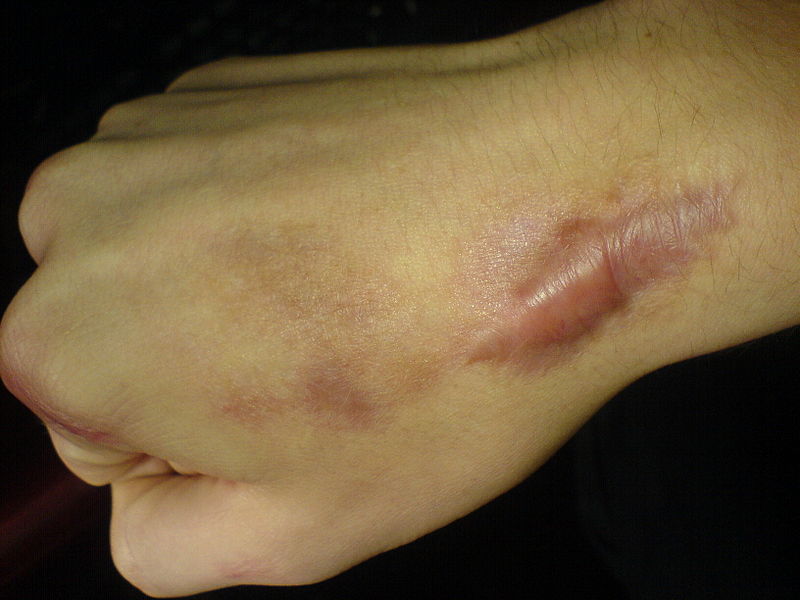
Horizontal Pyloromyotomy scar 10 days post-op in a one-month-old baby – Not altered. CC BY-SA 3.0
Repair
Tissue repair is when damaged tissue is replaced by a fibrous tissue.
The classic example of tissue repair is scar formation.
The steps involved with scar formation are as follows:
- An injury occurs to the tissue, such as a cut or scrape
- Regenerative stem cells are lost or a tissue is incapable of regenerating itself
- Granulation tissue is produced, along with type III collagen
- Type I collagen is produced
- Type III collagen is removed by collagenase
The components of granulation tissue include:
- Fibroblasts that deposit type I collagen
- Capillaries that allow the flow of oxygen and nutrients to the area
- Myofibroblasts that contract wound
Type I collagen is pliable, and is found in granulation tissue, embryonic tissue, uterus, and keloids.
Then eventually leads to scar formation in which type I collagen is replaced with type I collagen.
Type I collagen is pliable. It is found in granulation tissue, embryonic tissue, uterus, and keloids.
Type III collagen is very strong, and is found in skin, bone, tendons, and the majority of organs.
Collagenase is an enzyme that removes type I collagen during the wound healing process.
Collagenase requires zinc as a cofactor in order to function properly.
Zinc deficiency is associated with poor wound healing.
Please note that multinucleated giant cells may be seen histologically at sites of wound healing.
Tissue Repair Cellular Signaling
Cells communicate to signify that a wound has occurred.
Paracrine signaling is the main mode of cellular communication for wound repair.
Macrophages secrete growth factors that target fibroblasts and other cell types (such as epithelial cells, and smooth muscle)
Gene expression and cellular growth are produced by the interaction of growth factors with receptors. One example of this interaction is the epidermal growth factor with growth factor receptors.
Example of paracrine signals involved with wound healing includes:
- TGF-α: Growth factor for epithelial cells and fibroblasts
- TGF-b: Fibroblast growth factor that inhibits inflammation, regulates angiogenesis
- Platelet derived growth factor (PDGF) stimulates growth of fibroblasts, smooth muscle cells, and endothelial cells
- Vascular endothelial growth factor (VEGF) promotes angiogenesis, and epithelization
- Fibroblast growth factor promotes skeletal development and angiogenesis
Cutaneous Wound Healing
You must know the two different types of cutaneous wound healing:
- Primary intention (stitches)
- Secondary intention (wound left open)
Primary intention involves suturing the edges of a cutaneous wound together, which brings the edges and margins of the wound together and minimizes the production of scar tissue.
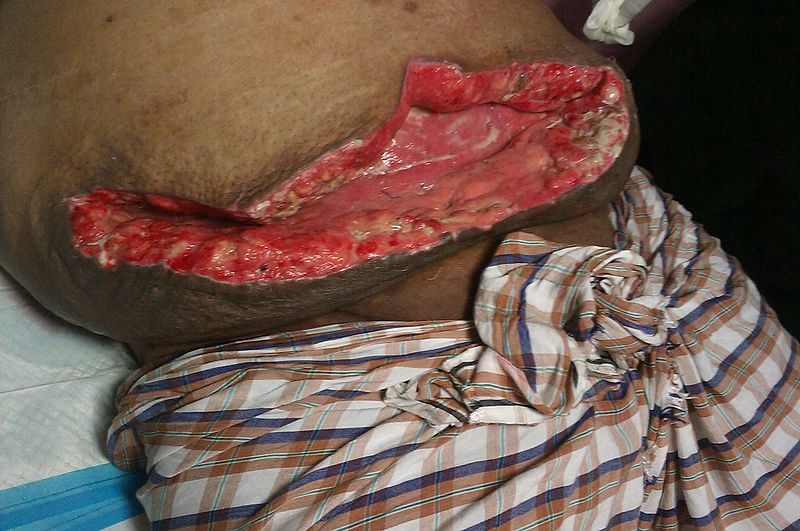
Secondary intention involves leaving the wound edges open, which results in granulation tissue filling the defect and myofibroblasts contracting the wound, and more scar tissue to be produced.
Abnormal Wound Healing
Abnormal wound healing includes:
- Delayed wound healing
- Dehiscence
- Hypertrophic scar
- Keloid
Delayed Wound Healing
Delayed wound healing may occurs due to:
- Infection (most common cause)
- Vitamin C deficiency (due to lack of hydroxylation of proline and lysine residues of pro-collagen into cross-linked cartilage)
- Copper deficiency (due to lack of cross-linking of lysin and hydroxylysine which is necessary to form collagen)
- Zinc deficiency (the enzyme collagenase needs zinc as a cofactor to convert type III collagen into type I collagen)
- Malnutrition
- Chronic diseases
- Diabetes mellitus
- Ischemia
- Foreign bodies
An infected wound may not allow proper wound healing to occur.
Vitamin C is needed in wound healing because in order to cross-link collagen, proline and lysine procollagen residues must be hydroxylated, and vitamin C is a key cofactor in this process.
Copper is needed in wound healing because lysyl oxidase requires copper as a cofactor in order to crosslink lysine and hydroxylysine to produce stable collagen.
Zinc is needed in wound healing because collagenase to remove weak type III collagen found in granulation tissue so that stronger type I collagen may be utilized.
Malnutrition, diabetes, ischemia, foreign bodies, and others are other causes of delayed wound healing.
Malnutrition may result in the aforementioned vitamin and mineral deficiencies.
Chronic disease such as chronic kidney disease and diabetes are known to be associated with poor wound healing.
Ischemia may lead to abnormal wound healing due to lack of oxygen.
Foreign bodies may lead to poor wound healing because they may continuously stimulate an inflammatory response.
Wound Dehiscence
Dehiscence occurs when a wound in the process of healing has it’s edges separated by force.
Wound dehiscence may be partial or total.
Wound dehiscence is typically encountered 5 to 9 days after surgery during the early stages of wound healing.
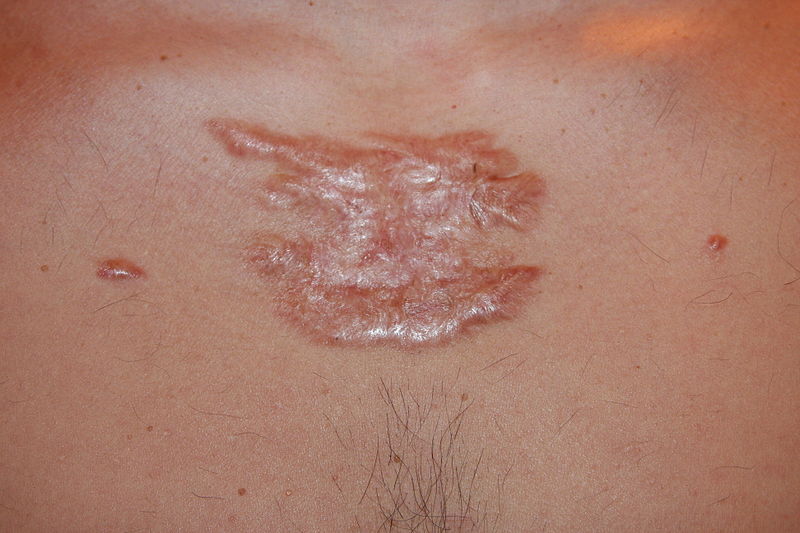
Hypertrophic Scar
A hypertrophic scar is defined as excessive scar tissue formation that is restricted to the site of the wound.
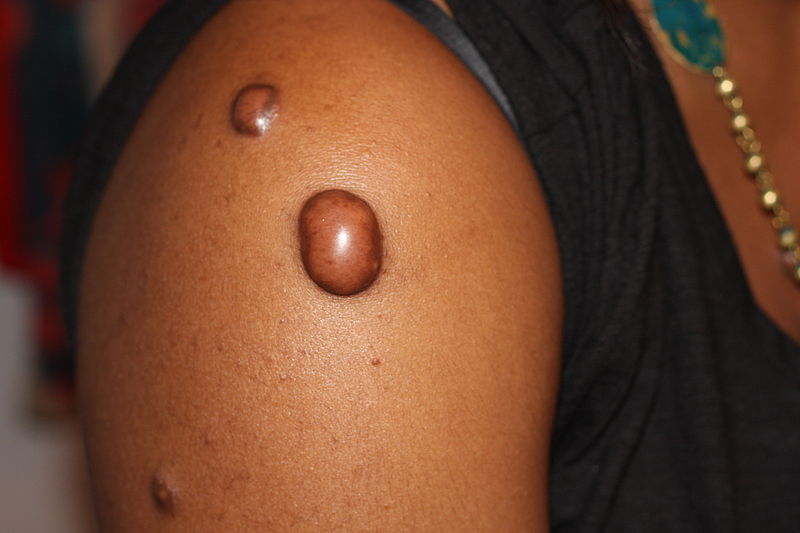
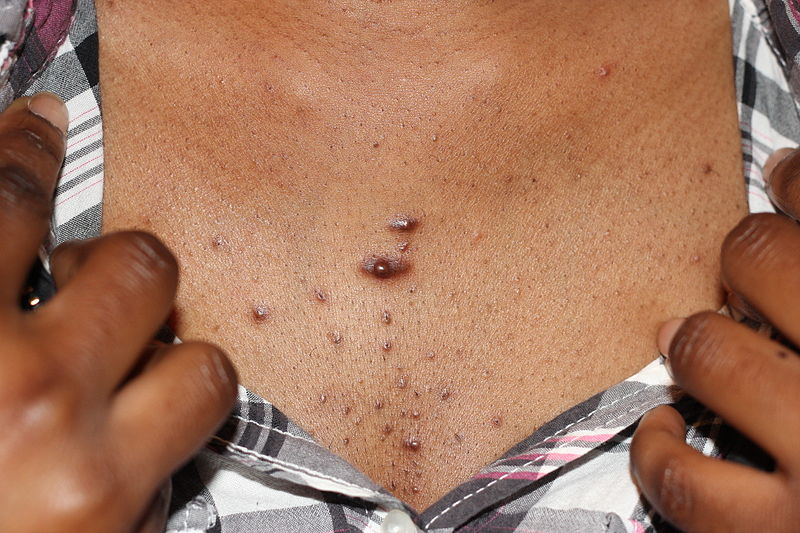
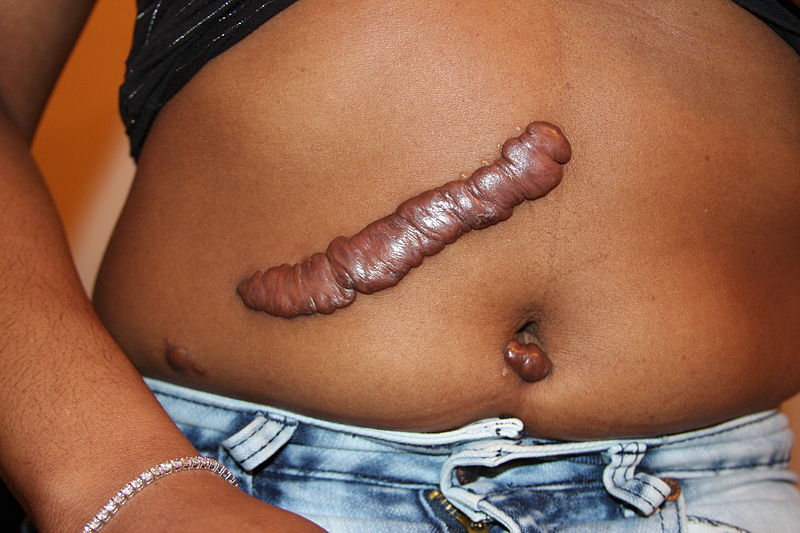
Keloid
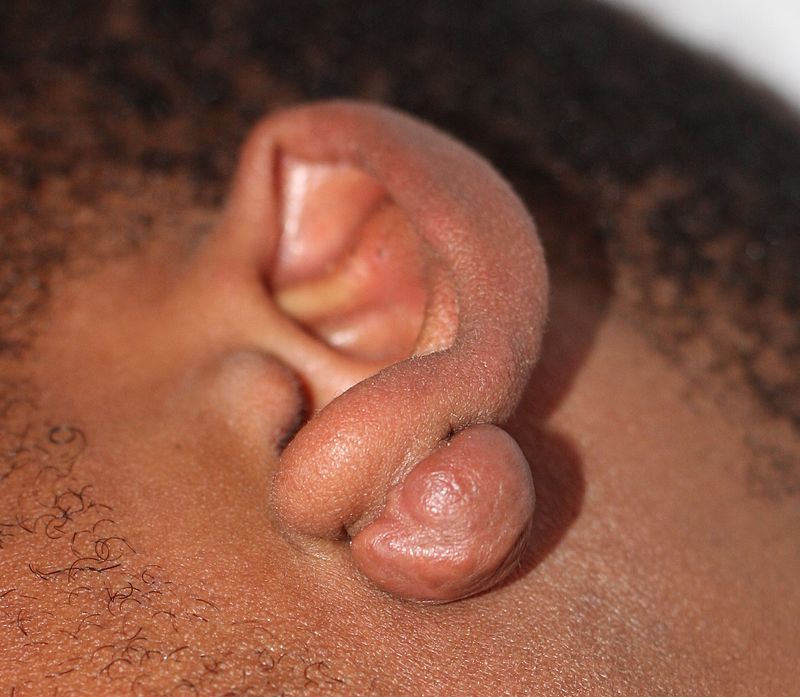
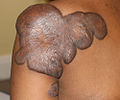
Keloids are also known as keloid scars or keloid disorder.
A keloid is an excessive amount of scar tissue produced relative to the size of the wound.
Early keloids are composed of primarily type III collagen.
Late keloids are composed of primarily type I collagen.
Keloids appear as rubber, firm, fibrous nodules on the skin.
Americans of African descent are at increased risk of keloids.
Keloids may occur anywhere on the skin, but are seen most commonly on the earlobes, trunk, and upper extremities.